Summary: Schwann cells are much more prolific in generating myelin than previously believed. Knocking out the fbxw7 gene in mouse models, researchers discovered individual Schwann cells began to spread myelin across many axons.
Source: Oregon Health & Sciences University
Scientists have discovered that a special type of cell is much more prolific in generating a protective sheath covering nerve fibers than previously believed.
The revelation about Schwann cells raises the possibility of new avenues to treat nerve injuries and various forms of neuropathy. Further research could prove useful in promoting myelin repair in central nervous system disorders such as multiple sclerosis, where damage to myelin slows or blocks electric signals from the brain.
“This totally overturns the textbook definition of the way Schwann cells work,” said senior author Kelly Monk, Ph.D., professor and co-director of the Vollum Institute at Oregon Health & Science University.
The research published today in the journal Nature Communications.
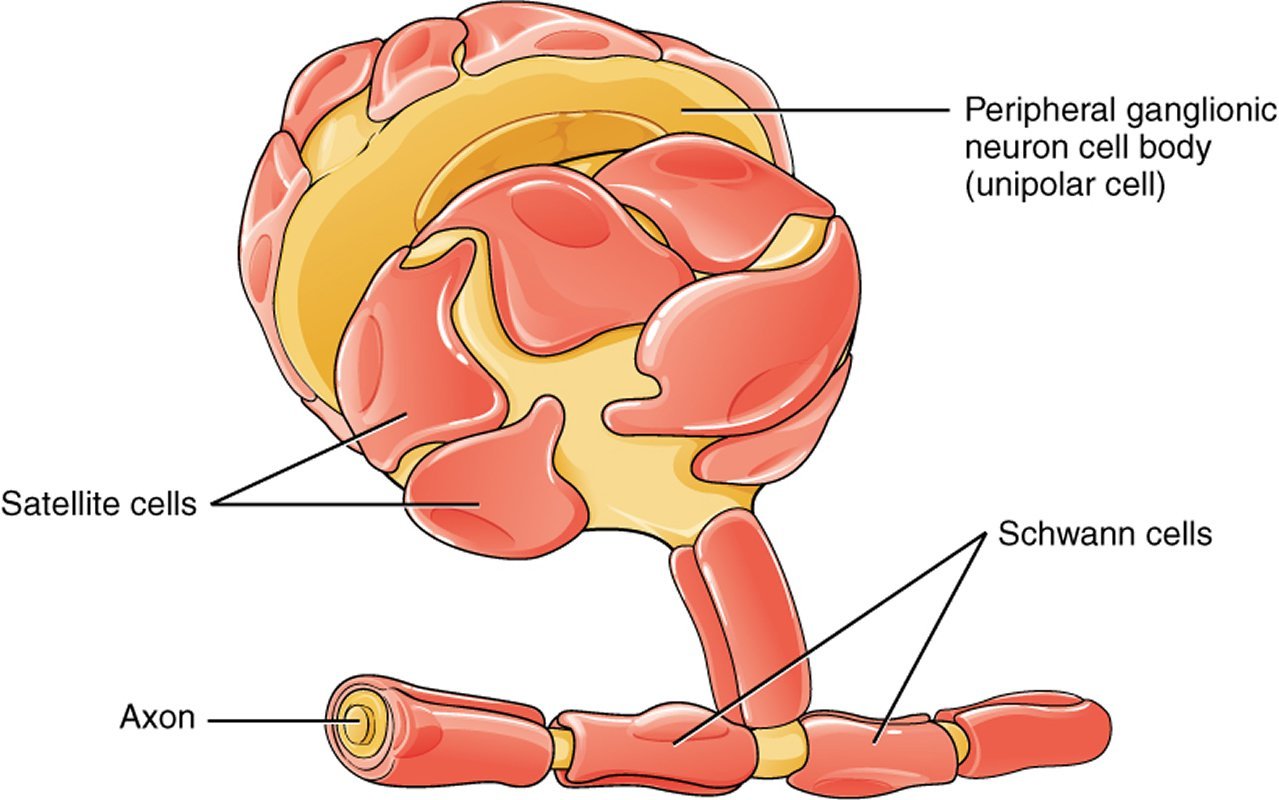
Two types of cells in the body produce myelin: oligodendrocytes in the brain and spinal cord, and Schwann cells in the rest of the body. Until now, scientists thought that only oligodendrocytes generated multiple myelin sheaths around axons, the slender projection of a nerve cell that carries electrical signals between cells.
The new research reveals that Schwann cells also are capable of spreading myelin across multiple axons.
Researchers made the discovery after conducting a genetic screen in zebrafish in the Monk laboratory. They discovered some fish had more myelin than expected, and those fish carried a mutation in a gene called fbxw7. When they knocked out the gene in genetically modified mice, they discovered an unexpected characteristic: individual Schwann cells began spreading myelin across many axons.
“It highlights a very plastic potential for these cells,” Monk said.
In discovering how Schwann cells generate myelin at the molecular level, the discovery may lead to new gene-therapy techniques to repair damaged myelin in peripheral nervous system disorders such as Charcot-Marie-Tooth disease, a painful inherited form of neuropathy that affects 1 in 2,500 people in the United States.
Both Schwann cells and oligodendrocytes arose at the same point in evolutionary history, with the appearance of jaws in the vertebrate lineage. Invertebrates lack myelin, and some, like the modern squid, uses thick axons to quickly transmit signals between neurons.
“We could have evolved that way, but our spinal cord would be the diameter of a giant sequoia tree,” Monk said.
Instead, vertebrate axons evolved myelin to protect axons and speed up signal transmission. To create myelin, Schwann cells evolved to produce it around a single axon in the peripheral nervous system. Oligodendrocytes, in turn, generated myelin along multiple axons within the more confined environment of the brain and spine – the central nervous system.
“The real estate is fundamentally different in the central nervous system than in the peripheral nervous system,” Monk said.
Monk theorizes that Schwann cells evolved a mechanism to repair damaged myelin on a cell by cell basis since it would have been common for injuries to occur without necessarily killing the entire organism. Those traits would have been passed down and strengthened through generations of evolution.
By contrast, remyelination in the central nervous system tended to be an evolutionary dead end since few would have survived a severe whack to the brain or spine.
“There’s no selective pressure in repairing myelin damage in the central nervous system because you’re probably going to die,” Monk said.
However, the discovery published today suggests a new opportunity to heal the brain and spine.
“Targeting the fbxw7 gene – or downstream pathway molecules – could be a powerful way to promote myelin repair in the central nervous system,” Monk said.
Funding: This work was supported by the National Institute of Neurological Disorders and Stroke, of the National Institutes of Health, award numbers F31 NS094004; F31 NS087801; F31 NS096814; R01 NS042595; and R01NS062796. Co-author David A. Lyons, Ph.D., of the University of Edinburgh is a Wellcome Senior Research Fellow. Monk receives support from the Edward J. Mallinckrodt Jr. Foundation, the Race to Erase MS Foundation, and she is a Harry Weaver Neuroscience Scholar of the National Multiple Sclerosis Society.
Source:
Oregon Health & Sciences University
Media Contacts:
Erik Robinson – Oregon Health & Sciences University
Image Source:
The image is credited to OpenStax. Licensed CC BY 4.0.
Original Research: Open access
“Myelinating Schwann cells ensheath multiple axons in the absence of E3 ligase component Fbxw7”. Breanne L. Harty, Fernanda Coelho, Sarah E. Pease-Raissi, Amit Mogha, Sarah D. Ackerman, Amy L. Herbert, Robert W. Gereau IV, Judith P. Golden, David A. Lyons, Jonah R. Chan & Kelly R. Mon.
Nature Communications. doi:10.1038/s41467-019-10881-y
Abstract
Myelinating Schwann cells ensheath multiple axons in the absence of E3 ligase component Fbxw7
In the central nervous system (CNS), oligodendrocytes myelinate multiple axons; in the peripheral nervous system (PNS), Schwann cells (SCs) myelinate a single axon. Why are the myelinating potentials of these glia so fundamentally different? Here, we find that loss of Fbxw7, an E3 ubiquitin ligase component, enhances the myelinating potential of SCs. Fbxw7 mutant SCs make thicker myelin sheaths and sometimes appear to myelinate multiple axons in a fashion reminiscent of oligodendrocytes. Several Fbxw7 mutant phenotypes are due to dysregulation of mTOR; however, the remarkable ability of mutant SCs to ensheathe multiple axons is independent of mTOR signaling. This indicates distinct roles for Fbxw7 in SC biology including modes of axon interactions previously thought to fundamentally distinguish myelinating SCs from oligodendrocytes. Our data reveal unexpected plasticity in the myelinating potential of SCs, which may have important implications for our understanding of both PNS and CNS myelination and myelin repair.







