Summary: Shorter sleep duration can increase the risk of children developing depression, anxiety, and cognitive problems. Children who routinely suffered sleep disruptions or shorter sleep durations had reduced brain volume in the orbitofrontal cortex, prefrontal cortex, precuneus, supramarginal gyrus, and temporal cortex.
Source: University of Warwick
Depression, anxiety, impulsive behavior and poor cognitive performance in children is affected by the amount of sleep they have researchers from the University of Warwick have found.
Sleep states are active processes that support the reorganisation of brain circuitry. This makes sleep especially important for children, whose brains are developing and reorganizing rapidly.
In the paper ‘Sleep duration, brain structure, and psychiatric and cognitive problems in children.’ published in the journal Molecular Psychiatry, 11,000 children aged 9-11 from the Adolescent Brain Cognitive Development dataset had the relationship between sleep duration and brain structure examined by researchers Professor Jianfeng Feng, Professor Edmund Rolls, Dr. Wei Cheng and colleagues from the University of Warwick’s Department of Computer Science and Fudan University.
Measures of depression, anxiety, impulsive behavior and poor cognitive performance in the children were associated with shorter sleep duration. Moreover, the depressive problems were associated with short sleep duration one year later.
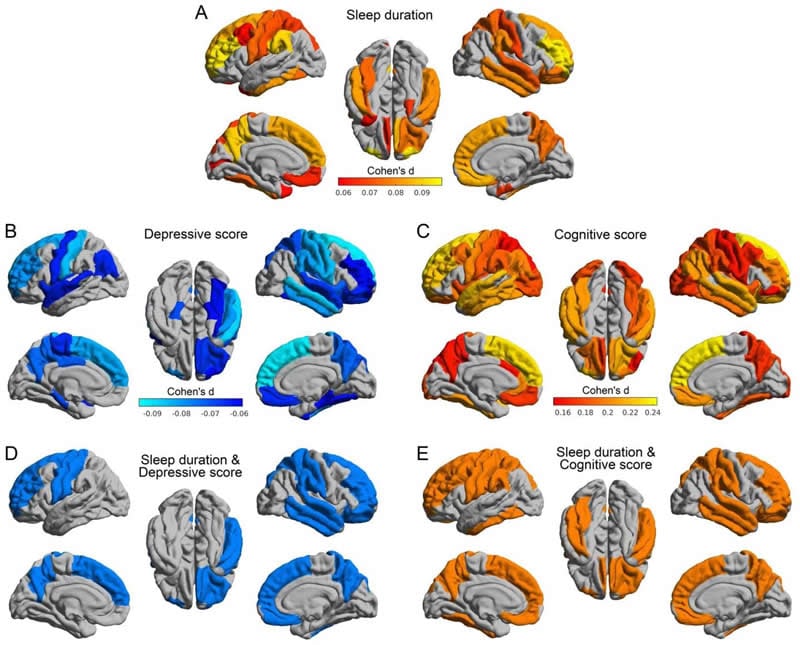
Lower brain volume of brain areas involved the orbitofrontal cortex, prefrontal and temporal cortex, precuneus, and supramarginal gyrus was found to be associated with the shorter sleep duration by using big data analysis approach.
Professor Jianfeng Feng, from the University of Warwick’s Department of Computer Science comments:
“The recommended amount of sleep for children 6 to 12 years of age is 9-12 hours. However, sleep disturbances are common among children and adolescents around the world due to the increasing demand on their time from school, increased screen time use, and sports and social activities.
A previous study showed that about 60% of adolescents in the United States receive less than eight hours of sleep on school nights.
“Our findings showed that the behavior problems total score for children with less than 7 hours sleep were 53% higher on average and the cognitive total score was 7.8% lower on average than for children with 9-11 hours of sleep. It highlights the importance of enough sleep in both cognition and mental health in children.”
Professor Edmund Rolls from the University of Warwick’s Department of Computer Science also commented:
“These are important associations that have been identified between sleep duration in children, brain structure, and cognitive and mental health measures, but further research is needed to discover the underlying reasons for these relationships.”
Source:
University of Warwick
Media Contacts:
Alice Scott – University of Warwick
Image Source:
The image is credited to University of Warwick.
Original Research: Closed access
“Sleep duration, brain structure, and psychiatric and cognitive problems in children”. Wei Cheng, Edmund Rolls, Weikang Gong, Jingnan Du, Jie Zhang, Xiao-Yong Zhang, Fei Li & Jianfeng Feng.
Molecular Psychiatry doi:10.1038/s41380-020-0663-2.
Abstract
Sleep duration, brain structure, and psychiatric and cognitive problems in children
Low sleep duration in adults is correlated with psychiatric and cognitive problems. We performed for the first time a large-scale analysis of sleep duration in children, and how this relates to psychiatric problems including depression, to cognition, and to brain structure. Structural MRI was analyzed in relation to sleep duration, and psychiatric and cognitive measures in 11,067 9–11-year-old children from the Adolescent Brain Cognitive Development (ABCD) Study, using a linear mixed model, mediation analysis, and structural equation methods in a longitudinal analysis. Dimensional psychopathology (including depression, anxiety, impulsive behavior) in the children was negatively correlated with sleep duration. Dimensional psychopathology in the parents was also correlated with short sleep duration in their children. The brain areas in which higher volume was correlated with longer sleep duration included the orbitofrontal cortex, prefrontal and temporal cortex, precuneus, and supramarginal gyrus. Longitudinal data analysis showed that the psychiatric problems, especially the depressive problems, were significantly associated with short sleep duration 1 year later. Further, mediation analysis showed that depressive problems significantly mediate the effect of these brain regions on sleep. Higher cognitive scores were associated with higher volume of the prefrontal cortex, temporal cortex, and medial orbitofrontal cortex. Public health implications are that psychopathology in the parents should be considered in relation to sleep problems in children. Moreover, we show that brain structure is associated with sleep problems in children, and that this is related to whether or not the child has depressive problems.






