Summary: Progressive supranuclear palsy (PSP) and corticobasal syndrome (CBS), two atypical parkinsonian syndromes, may be twice as common as previously believed, researchers report.
Source: UCL
Two rare degenerative neurological disorders, namely Progressive Supranuclear Palsy (PSP) and CorticoBasal Degeneration (CBD), may be twice as common as previously thought, a UCL-led study finds.
Initial results from the PROSPECT study, published in JAMA Neurology, estimates that up to 10,000 people may be living with PSP & CBD in the UK.
The PROSPECT study is a longitudinal research program, funded by PSPA, which uses MRI scanning, blood and cerebrospinal fluid samples, genetics, and clinical assessments to find ways of tracking disease progression and improving diagnosis.
Baseline data from the first five years of the PROSPECT study has shown that 50% of people living with PSP had a delayed diagnosis because they initially presented with symptoms similar to other neurodegenerative conditions such as Parkinson’s disease and frontotemporal dementia.
The study, led by Professor Huw Morris and Dr Edwin Jabbari (both UCL Queen Square Institute of Neurology), found that the different forms of PSP & CBD had distinct patterns of clinical, cognitive, MRI and blood protein results that can be used to improve early and accurate diagnosis in the clinic.
Professor Morris said: “With the support of patients, carers and PSPA we have completed the primary stage of the PSP – PROPSECT study.
“Surprisingly, recently described rarer presentations of PSP are as frequent as the classical form of PSP, indicating that the disease may be twice as common as previously thought.
“We hope that this improved understanding of the disease spectrum will lead to better, earlier diagnosis and ultimately to better treatments.”
Now baselining of the initial data collection has been completed, the study is entering into the second phase which will provide one year follow up data on disease progression in participants.
As the study continues Prof Morris and his team of researchers hope to discover biomarkers and diagnostic tools which will enable better outcomes for people with PSP & CBD in the future.
Dr Wendy Edwards, Research Manager at PSPA, said: “The initial results of the PROSPECT study provide an exciting development in our fight against PSP & CBD. PSP & CBD are regularly misdiagnosed with other neurodegenerative conditions such as Parkinson’s and Alzheimer’s due to the lack of specialist knowledge about these rare diseases. These latest ground breaking findings give PSPA the ammunition we need to campaign for increased awareness, better diagnosis and improved care for those living with PSP & CBD.”
The PROSPECT study is the core research project of the UK PSP Research Network, which was established in 2012. The study began five years ago in 2014 and -will been funded by PSPA until 2023.
The aim of the study is to:
- Expand recruitment to create the world’s largest PSP & CBD cohort
- Improve diagnosis by discovering diagnostic markers of PSP & CBD
- Better understand the progression of PSP & CBD to help define new treatments
- Support upcoming clinical trials and ultimately accelerate the discovery of future treatments.
Alongside UCL, the PROSPECT study, represents a UK-wide collaborative effort with data also collected and analysed by Professor James Rowe (University of Cambridge), Professor Michele Hu (University of Oxford), Professor Nicola Pavese and Professor David Burn (Newcastle University), Professor Nigel Leigh (Brighton and Sussex Medical School) Dr Alistair Church (Royal Gwent Hospital) and Dr Chris Kobylecki and Dr Alex Gerhard (both University of Manchester).
Funding: Additional funding for the study has come from UCL, CBD Solutions and other organisations.
Source:
UCL
Media Contacts:
Henry Killworth – UCL
Image Source:
The image is credited to UCL.
Original Research: Open access
“Diagnosis Across the Spectrum of Progressive Supranuclear Palsy and Corticobasal Syndrome”. Edwin Jabbarin et al.
JAMA Neurology doi:10.1001/jamaneurol.2019.4347.
Abstract
Diagnosis Across the Spectrum of Progressive Supranuclear Palsy and Corticobasal Syndromer
Importance
Atypical parkinsonian syndromes (APS), including progressive supranuclear palsy (PSP), corticobasal syndrome (CBS), and multiple system atrophy (MSA), may be difficult to distinguish in early stages and are often misdiagnosed as Parkinson disease (PD). The diagnostic criteria for PSP have been updated to encompass a range of clinical subtypes but have not been prospectively studied.
Objective
To define the distinguishing features of PSP and CBS subtypes and to assess their usefulness in facilitating early diagnosis and separation from PD.
Design, Setting, Participants
This cohort study recruited patients with APS and PD from movement disorder clinics across the United Kingdom from September 1, 2015, through December 1, 2018. Patients with APS were stratified into the following groups: those with Richardson syndrome (PSP-RS), PSP-subcortical (including PSP-parkinsonism and progressive gait freezing subtypes), PSP-cortical (including PSP-frontal and PSP-CBS overlap subtypes), MSA-parkinsonism, MSA-cerebellar, CBS–Alzheimer disease (CBS-AD), and CBS–non-AD. Data were analyzed from February 1, through May 1, 2019.
Main Outcomes and Measures
Baseline group comparisons used (1) clinical trajectory; (2) cognitive screening scales; (3) serum neurofilament light chain (NF-L) levels; (4) TRIM11, ApoE, and MAPT genotypes; and (5) volumetric magnetic resonance imaging measures.
Results
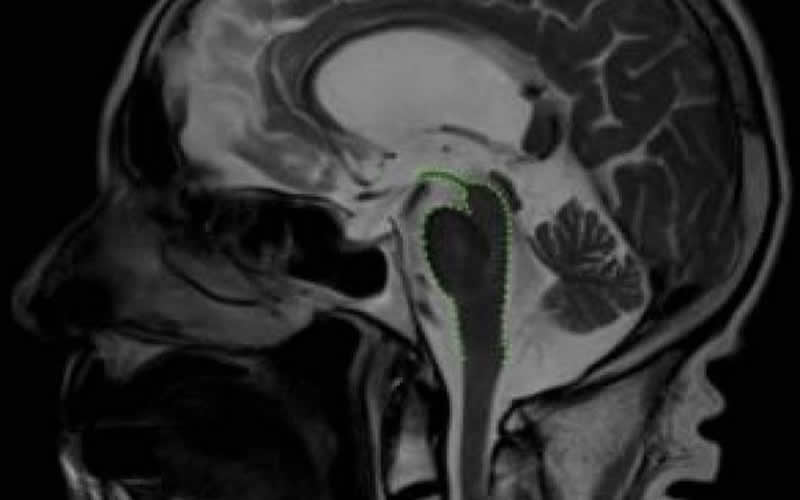
A total of 222 patients with APS (101 with PSP, 55 with MSA, 40 with CBS, and 26 indeterminate) were recruited (129 [58.1%] male; mean [SD] age at recruitment, 68.3 [8.7] years). Age-matched control participants (n = 76) and patients with PD (n = 1967) were included for comparison. Concordance between the antemortem clinical and pathologic diagnoses was achieved in 12 of 13 patients with PSP and CBS (92.3%) undergoing postmortem evaluation. Applying the Movement Disorder Society PSP diagnostic criteria almost doubled the number of patients diagnosed with PSP from 58 to 101. Forty-nine of 101 patients with reclassified PSP (48.5%) did not have the classic PSP-RS subtype. Patients in the PSP-subcortical group had a longer diagnostic latency and a more benign clinical trajectory than those in PSP-RS and PSP-cortical groups. The PSP-subcortical group was distinguished from PSP-cortical and PSP-RS groups by cortical volumetric magnetic resonance imaging measures (area under the curve [AUC], 0.84-0.89), cognitive profile (AUC, 0.80-0.83), serum NF-L level (AUC, 0.75-0.83), and TRIM11 rs564309 genotype. Midbrain atrophy was a common feature of all PSP groups. Eight of 17 patients with CBS (47.1%) undergoing cerebrospinal fluid analysis were identified as having the CBS-AD subtype. Patients in the CBS-AD group had a longer diagnostic latency, relatively benign clinical trajectory, greater cognitive impairment, and higher APOE-ε4 allele frequency than those in the CBS–non-AD group (AUC, 0.80-0.87; P < .05). Serum NF-L levels distinguished PD from all PSP and CBS cases combined (AUC, 0.80; P < .05).
Conclusions and Relevance
These findings suggest that studies focusing on the PSP-RS subtype are likely to miss a large number of patients with underlying PSP tau pathology. Analysis of cerebrospinal fluid defined a distinct CBS-AD subtype. The PSP and CBS subtypes have distinct characteristics that may enhance their early diagnosis.