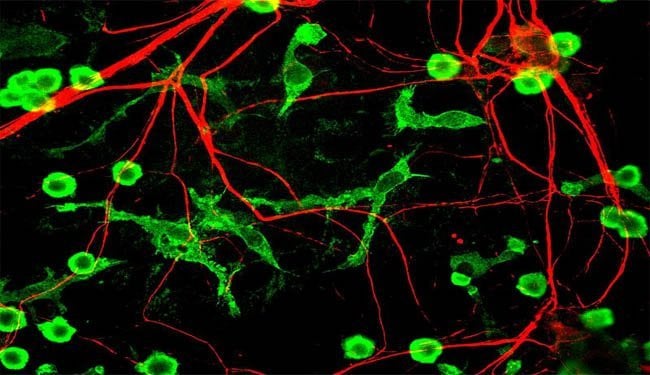
Immune cells “sculpt” circuits in the brain by eating away excess connections
Findings offer a fresh look at developmental and degenerative brain diseases
We’re born with our brains prewired, but as information comes in from our environment, this circuitry is updated. A study from Boston Children’s Hospital provides a new glimpse of how this happens: Brain cells known as microglia, tuned into the crosstalk between neurons, literally engulf unnecessary connections, known as synapses, and prune them away.
The study, led by Beth Stevens, PhD, and Dori Schafer, PhD, of the Department of Neurology and the F.M. Kirby Neurobiology Center at Boston Children’s Hospital, is the first to capture microglia, previously thought of as immune cells, in the act of eliminating synapses in the healthy, developing brain. The study further shows that microglia take their cues from neurons’ activity patterns and from a set of signals called the complement cascade, used by the immune system to rid the body of unwanted pathogens and debris. When complement signaling is disrupted, pruning of synapses is diminished.
The findings, reported online May 23 in the journal Neuron, may have implications for understanding neurodegenerative diseases in which synapses are lost, or developmental disorders such as autism in which synapses are dysfunctional.
Microglia were once thought to play mainly a supportive role in the brain, protecting against disease. Only recently have scientists begun to recognize their involvement in healthy brain development.
“They’re gatekeepers that are extremely responsive to changes in the environment,” says Stevens, senior investigator on the study. “They’re in the brain all the time it’s wiring up, and they can move and sense changes in activity.”
Stevens first showed in 2007 that defects in the complement system inhibit pruning of synapses, and that neurons are loaded with complement proteins soon after birth, just when pruning is at its peak. In the new paper, she and Schafer demonstrate that microglia have receptors that recognize the complement protein C3 – the same protein found on synapses that are destined for elimination.
“We think that weaker synapses are being tagged with C3, and that microglia are eliminating them just as macrophages would eliminate bacteria,” says Schafer, first author on the paper. “C3 is like an ‘eat me’ signal.”
Mice lacking C3 receptors, or whose microglia had these receptors blocked with a drug, did not eliminate weaker synapses, the researchers showed.
Because microglia are so active, the researchers tracked their activity in mice, using dyes as tracers, and focused on the visual system connecting the eyes and brain, because it is well understood and relatively easy to manipulate.
Stevens thinks that their findings might shed light on diseases that involve synapse loss or dysfunction. In neurodegenerative diseases such as glaucoma, Alzheimer’s disease, Lou Gehrig’s disease, Huntington’s disease and Parkinson’s disease, scientists have noted subtle changes in synapses that might cause them to be targeted for elimination. In the healthy adult brain, microglia are in a resting state, but in these diseases, both microglia and the complement system become activated. Stevens and Schafer speculate that targeting microglia, their complement receptors or complement proteins themselves could prevent synapse loss in these diseases.
There are also data suggesting that microglia and/or the complement cascade may be involved in neurodevelopmental disorders such as autism, epilepsy or schizophrenia, perhaps altering the brain’s normal balance of synapses.
“All this is still very speculative,” Stevens cautions. “We first need to understand normal development.”
About this neuroscience research article
The study was funded by the Smith Family Foundation, the Dana Foundation, the John Merck Scholars Program, the National Institute of Neurological Disorders and Stroke, an NIH National Research Service Award, the National Institute on Drug Abuse, and the National Institutes of Health.
Boston Children’s Hospital is home to the world’s largest research enterprise based at a pediatric medical center, where its discoveries have benefited both children and adults since 1869. More than 1,100 scientists, including nine members of the National Academy of Sciences, 11 members of the Institute of Medicine and nine members of the Howard Hughes Medical Institute comprise Boston Children’s research community. Founded as a 20-bed hospital for children, Boston Children’s today is a 395 bed comprehensive center for pediatric and adolescent health care. Boston Children’s also is the primary pediatric teaching affiliate of Harvard Medical School.
Contact: Meghan Weber – Boston Children’s Hospital
Press release submitted to Neuroscience News by: Meghan Weber
Additional Source: Boston Children’s Hospital
Image Source: Neurology image adapted from Wikimedia Commons user Gerry Shaw. Licensed under the Creative Commons Attribution-Share Alike 3.0 Unported.
Original Research: Summary for “Microglia Sculpt Postnatal Neural Circuits in an Activity and Complement-Dependent Manner” by Dorothy P. Schafer, Emily K. Lehrman, Amanda G. Kautzman, Ryuta Koyama, Alan R. Mardinly, Ryo Yamasaki, Richard M. Ransohoff, Michael E. Greenberg, Ben A. Barres, Beth Stevens. Published in Neuron, Volume 74, Issue 4, 24 May 2012, Pages 691–7052. http://dx.doi.org/10.1016/j.neuron.2012.03.026