Summary: Researchers report a molecular pathway that activates during fasting could help halt the spread of intestinal bacteria into the bloodstream.
Source: Salk Institute.
A molecular pathway that is activated in the brain during fasting helps halt the spread of intestinal bacteria into the bloodstream, according to a new study by a team of researchers at the Salk Institute.
The study, published the week of May 16, 2016 in the Proceedings of the National Academy of Sciences, shows a molecular pathway by which the brain communicates with the gastrointestinal (GI) tract to prevent unnecessary activation of the immune system during fasting by strengthening the barrier against gut microbes. The discovery of this brain-gut signal in fruit flies, which has many parallels to humans, could eventually inform the treatment of inflammatory bowel diseases in people.
In addition to its role in promoting the absorption of nutrients from food, the GI tract is host to a panoply of bacteria. These microbes actually help in the digestive process by producing chemicals that break down complex fats and carbohydrates.
“Fasting has a positive value that spills over not just into the metabolic system, but also inflammation and brain function,” says the study’s lead investigator Marc Montminy, professor in the Clayton Foundation Laboratories for Peptide Biology and holder of the J.W. Kieckhefer Foundation Chair. “Understanding how the gut maintains this barrier, and creating drugs to enhance that barrier, may have important benefits for people with inflammatory bowel disease.”
The new study is part of an ongoing collaborative effort by the Montminy lab and the lab of Salk Professor John Thomas to pin down the mechanisms that a genetic switch in the brain called Crtc uses to control energy balance. A constant network of communication–between our brains and the GI tract, as well as other tissues–helps our bodies keep tabs on our energy expenditure and stores. Crtc interacts with another molecule called CREB, and fasting activates both proteins and boosts formation of long-term memories.
The Montminy and Thomas teams used fruit flies to study the Crtc switch, in part because flies express many of the same metabolism-related genes as humans do. Previous experiments by the two labs have shown that flies whose Crtc gene is deleted become sensitized to fasting–they only survive about half as long without food compared to flies with the Crtc gene. The researchers were aiming to understand why the deletion of Crtc caused flies to die sooner and had hypothesized it was because these mutant flies have fewer fat and sugar stores.
What the team–along with Salk Assistant Professor Janelle Ayres’ group–found in the new study, however, was surprising and more complicated. The guts of the flies without Crtc expressed several molecules indicating that their immune system was keyed up. When postdoctoral researcher Run Shen entered Montminy’s lab with the evidence–pictures taken from the microscope of fluorescently stained cells lining the flies’ guts–“it was totally unexpected,” he says.
The new results suggest that the flies are more sensitive to starvation because the immune system is activated, which is energetically taxing. This amped-up immune response suggests that without Crtc, bacteria leak from the gut into the fly’s circulation. The researchers found that the normal role of Crtc is to fortify the barriers of the gut to prevent bacteria from entering the bloodstream and awakening the immune system. Without Crtc, the connections between cells that line the gut tube become disrupted, causing bacteria to leak out, activating the immune response and depleting energy reserves.
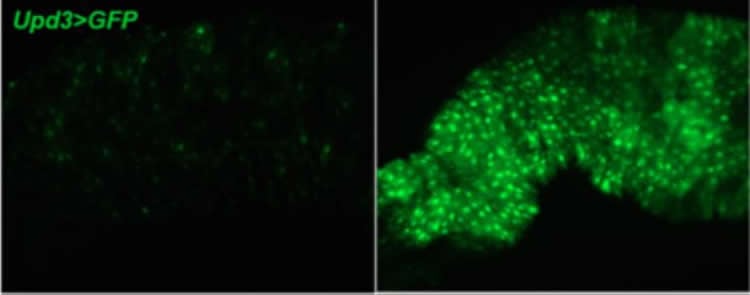
While looking for molecular partners of Crtc, the researchers uncovered a protein called short neuropeptide F (sNPF), which is also found in the brain and has an equivalent in humans (called neuropeptide Y). This peptide is known to cause flies and mammals to search for food in response to hunger signals. Without sNPF in the brain, the flies showed signs of gut inflammation similar to those flies missing Crtc. What’s more, the normally tight seals along the gastrointestinal tract were broken down in the sNPF-lacking flies, letting bacteria out.
Conversely, flies expressing more than the normal amounts of Crtc or sNPF in their neurons were able to survive longer without food and showed less disruption to the tight junctions that maintain their gastrointestinal barriers.
The researchers are conducting more experiments to understand how the neuropeptides activate the gut receptors that help protect it from bacterial invasion.
Other authors on the work were Biao Wang and Maria Giribaldi of the Salk Institute.
Funding: The work was supported by the National Institutes of Health, the Leona M. and Harry B. Helmsley Charitable Trust and the Glenn Centers for Research in Aging.
Source: Salk Institute
Image Source: This NeuroscienceNews.com image is credited to Salk Institute.
Original Research: The study will appear in PNAS during the week of May 16 2016.
[cbtabs][cbtab title=”MLA”]Salk Institute. “Genetic Switch Turned on During Fasting Helps Stop Inflammation.” NeuroscienceNews. NeuroscienceNews, 17 May 2016.
<https://neurosciencenews.com/fasting-genetics-neuroinflammation-4238/>.[/cbtab][cbtab title=”APA”]Salk Institute. (2016, May 17). Genetic Switch Turned on During Fasting Helps Stop Inflammation. NeuroscienceNews. Retrieved May 17, 2016 from https://neurosciencenews.com/fasting-genetics-neuroinflammation-4238/[/cbtab][cbtab title=”Chicago”]Salk Institute. “Genetic Switch Turned on During Fasting Helps Stop Inflammation.” NeuroscienceNews.
https://neurosciencenews.com/fasting-genetics-neuroinflammation-4238/ (accessed May 17, 2016).[/cbtab][/cbtabs]







