Summary: An imbalance in gut bacteria can cause the reduction of some metabolites, resulting in depression-like symptoms. The findings contribute to the growing body of evidence for the role the microbiome plays in brain function and mental health.
Source: Institut Pasteur
Depression is a mental disorder that affects more than 264 million people of all ages worldwide. Understanding its mechanisms is vital for the development of effective therapeutic strategies. Scientists from the Institut Pasteur, Inserm and the CNRS recently conducted a study showing that an imbalance in the gut bacterial community can cause a reduction in some metabolites, resulting in depressive-like behaviors.
These findings, which show that a healthy gut microbiota contributes to normal brain function, were published in Nature Communications on December 11, 2020.
The bacterial population in the gut, known as the gut microbiota, is the largest reservoir of bacteria in the body. Research has increasingly shown that the host and the gut microbiota are an excellent example of systems with mutually beneficial interactions. Recent observations also revealed a link between mood disorders and damage to the gut microbiota.
This was demonstrated by a consortium of scientists from the Institut Pasteur, the CNRS and Inserm, who identified a correlation between the gut microbiota and the efficacy of fluoxetine, a molecule frequently used as an antidepressant. But some of the mechanisms governing depression, the leading cause of disability worldwide, remained unknown.
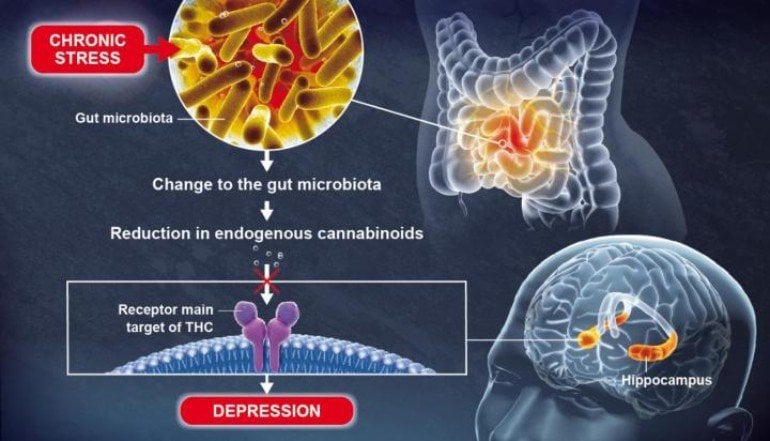
Using animal models, scientists recently discovered that a change to the gut microbiota brought about by chronic stress can lead to depressive-like behaviors, in particular by causing a reduction in lipid metabolites (small molecules resulting from metabolism) in the blood and the brain.
These lipid metabolites, known as endogenous cannabinoids (or endocannabinoids), coordinate a communication system in the body which is significantly hindered by the reduction in metabolites. Gut microbiota plays a role in brain function and mood regulation
Endocannabinoids bind to receptors that are also the main target of THC, the most widely known active component of cannabis. The scientists discovered that an absence of endocannabinoids in the hippocampus, a key brain region involved in the formation of memories and emotions, resulted in depressive-like behaviors.
The scientists obtained these results by studying the microbiotas of healthy animals and animals with mood disorders. As Pierre-Marie Lledo, Head of the Perception and Memory Unit at the Institut Pasteur (CNRS/Institut Pasteur) and joint last author of the study, explains: “Surprisingly, simply transferring the microbiota from an animal with mood disorders to an animal in good health was enough to bring about biochemical changes and confer depressive-like behaviors in the latter.”
The scientists identified some bacterial species that are significantly reduced in animals with mood disorders. They then demonstrated that an oral treatment with the same bacteria restored normal levels of lipid derivatives, thereby alleviating the depressive-like behaviors. These bacteria could therefore serve as an antidepressant. Such treatments are known as “psychobiotics”.
“This discovery shows the role played by the gut microbiota in normal brain function,” continues Gérard Eberl, Head of the Microenvironment and Immunity Unit (Institut Pasteur/Inserm) and joint last author of the study. If there is an imbalance in the gut bacterial community, some lipids that are vital for brain function disappear, encouraging the emergence of depressive-like behaviors. In this particular case, the use of specific bacteria could be a promising method for restoring a healthy microbiota and treating mood disorders more effectively.
About this microbiome and depression research news
Source: Institut Pasteur
Contact: Aurelie Perthuison – Institut Pasteur
Image: The image is credited to Institut Pasteur / Pascal Marseaud
Original Research: Open access.
“Effect of gut microbiota on depressive-like behaviors in mice is mediated by the endocannabinoid system” by Grégoire Chevalier, Eleni Siopi, Laure Guenin-Macé, Maud Pascal, Thomas Laval, Aline Rifflet, Ivo Gomperts Boneca, Caroline Demangel, Benoit Colsch, Alain Pruvost, Emeline Chu-Van, Aurélie Messager, François Leulier, Gabriel Lepousez, Gérard Eberl & Pierre-Marie Lledo. Nature Communications
Abstract
Effect of gut microbiota on depressive-like behaviors in mice is mediated by the endocannabinoid system
Depression is the leading cause of disability worldwide. Recent observations have revealed an association between mood disorders and alterations of the intestinal microbiota. Here, using unpredictable chronic mild stress (UCMS) as a mouse model of depression, we show that UCMS mice display phenotypic alterations, which could be transferred from UCMS donors to naïve recipient mice by fecal microbiota transplantation. The cellular and behavioral alterations observed in recipient mice were accompanied by a decrease in the endocannabinoid (eCB) signaling due to lower peripheral levels of fatty acid precursors of eCB ligands. The adverse effects of UCMS-transferred microbiota were alleviated by selectively enhancing the central eCB or by complementation with a strain of the Lactobacilli genus. Our findings provide a mechanistic scenario for how chronic stress, diet and gut microbiota generate a pathological feed-forward loop that contributes to despair behavior via the central eCB system.







