A synthetic compound is able to turn off “secondary” vacuum cleaners in the brain that take up serotonin, resulting in the “happy” chemical being more plentiful, scientists from the School of Medicine at The University of Texas Health Science Center San Antonio have discovered. Their study, released June 18 by The Journal of Neuroscience, points to novel targets to treat depression.
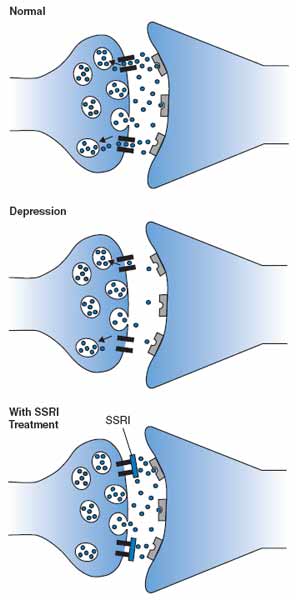
Serotonin, a neurotransmitter that carries chemical signals, is associated with feelings of wellness. Selective serotonin reuptake inhibitors (SSRIs) are commonly prescribed antidepressants that block a specific “vacuum cleaner” for serotonin (the serotonin transporter, or SERT) from taking up serotonin, resulting in more supply of the neurotransmitter in circulation in the extracellular fluid of the brain.
Delicate balance
“Serotonin is released by neurons in the brain,” said Lyn Daws, Ph.D., professor of physiology and pharmacology in the School of Medicine. “Too much or too little may be a bad thing. It is thought that having too little serotonin is linked to depression. That’s why we think Prozac-type drugs (SSRIs) work, by stopping the serotonin transporter from taking up serotonin from extracellular fluid in the brain.”
A problem with SSRIs is that many depressed patients experience modest or no therapeutic benefit. It turns out that, while SSRIs block the activity of the serotonin transporter, they don’t block other “vacuum cleaners.” “Until now we did not appreciate the presence of backup cleaners for serotonin,” Dr. Daws said. “We were not the first to show their presence in the brain, but we were among the first show that they were limiting the ability of the SSRIs to increase serotonin signaling in the brain. The study described in this new paper is the first demonstration of enhancing the antidepressant-like effect of an SSRI by concurrently blocking these backup vacuum cleaners.”
Serotonin ceiling
Even if SERT activity is blocked, the backup vacuum cleaners (called organic cation transporters) keep a ceiling on how high the serotonin levels can rise, which likely limits the optimal therapeutic benefit to the patient, Dr. Daws said.
“Right now, the compound we have, decynium-22, is not an agent that we want to give to people in clinical trials,” she said. “We are not there yet. Where we are is being able to use this compound to identify new targets in the brain for antidepressant activity and to turn to medicinal chemists to design molecules to block these secondary vacuum cleaners.”
Notes about this neuropsychopharmacology and SSRI antidepressant research
This work was supported by National Institutes of Health Grants R01-MH064489 (L.C.D.), R01-MH093320 (L.C.D., W.K.) and R03-MH086708 (G.G.G.), and a National Alliance for Research on Schizophrenia and Depression Independent Investigator Award (L.C.D.).
Contact: Will Sansom – University of Texas Health Science Center at San Antonio
Source: University of Texas Health Science Center at San Antonio press release
Image Source: The SSRI neuron image is credited to the NIH and is in the public domain.
Original Research: Abstract for “Decynium-22 Enhances SSRI-Induced Antidepressant-Like Effects in Mice: Uncovering Novel Targets to Treat Depression” by Rebecca E. Horton, Deana M. Apple, W. Anthony Owens, Nicole L. Baganz, Sonia Cano, Nathan C. Mitchell, Melissa Vitela, Georgianna G. Gould, Wouter Koek, and Lynette C. Daws in Journal of Neuroscience. Published online June 19 2013 doi:10.1523/JNEUROSCI.5687-11.2013