Summary: The fetal gut has far better developed immune capabilities than previously thought. The findings could help develop new maternal vaccines and provide early insight into potential autoimmune disorders, which may occur later in life.
Source: University of Pittsburgh
Most biology textbooks explain that the fetal immune system is largely undeveloped and that it learns after being exposed to the world at birth. New research from the University of Pittsburgh School of Medicine and UPMC Children’s Hospital of Pittsburgh challenges that paradigm and provides the first comprehensive look at the immune system of the developing gut. The findings, published today in the journal Developmental Cell, show that the fetal gut has far more well-developed immune capabilities than previously thought.
“Understanding intestinal immune development is crucial as it may have major impacts on the risk of developing autoimmune and autoinflammatory conditions like inflammatory bowel disease later on in life,” said co-senior author Liza Konnikova, M.D., Ph.D., assistant professor of pediatrics at the Pitt School of Medicine and a neonatologist at UPMC Children’s Hospital.
“It also opens the door to developing new maternal vaccines that may offer lifelong protections against major infectious diseases even before birth.”
Konnikova and her colleagues applied advanced cellular and genomic analyses to study the makeup of the immune system in gut tissues from 14- to 23-week-old fetuses and infants undergoing surgery to correct gut defects.
“We were surprised to find that almost complete immune capacity in the gut had developed as early as 14 weeks, and it remained mostly stable through infancy,” said Konnikova. The fetal gut had cells from both the innate and adaptive immune systems. The innate immune system is always present in the body and is not specific, but refers to barriers, such as skin, and immune cells that respond quickly to invaders. The adaptive immune system is created in response to a foreign substance, making it specific to that invader, but needs to be primed to recognize the pathogen before it can work, which can be achieved with immunization or prior infection.
In the innate immune system, the researchers found a large variety of antigen-presenting cells, which are crucial to priming and activating the adaptive immune system, and natural killer cells, which attack virus-infected cells and tumor cells. Other innate immune cells called neutrophils, which are recruited only to sites of inflammation were found in infants after birth, but not in the fetuses.
Konnikova and her colleagues also found abundant amounts of B cells and T cells in the fetal gut, which are part of the adaptive immune system.
Surprisingly, most of the T cells were of the “memory” type that helps the body remember past invaders in order to respond faster to repeat attacks in the future.
“Finding memory T cells was completely unexpected because these cells need to be exposed to a pathogen to form, and you would think that the placenta would prevent most pathogens from entering the womb,” Konnikova said. She speculated that the fetuses could be exposed to molecular byproducts of pathogens from the amniotic fluid that they float in, which they begin swallowing as early as 12 weeks.
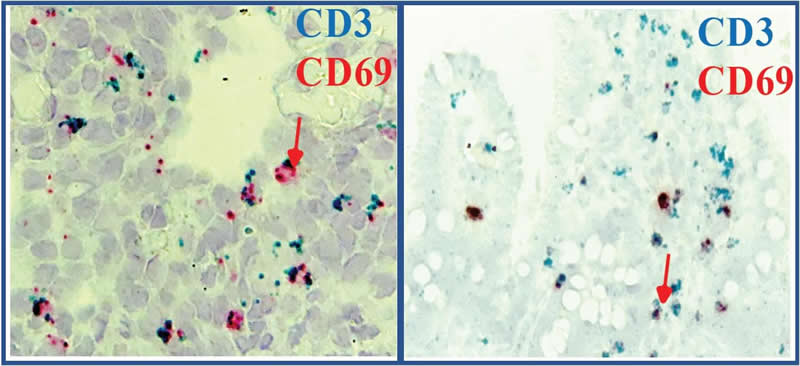
The study authors suggest that the large numbers of memory T cells could help provide some initial protection at birth, when the baby is exposed to a sudden onslaught of microbes, and also prevent it from being overactivated.
Konnikova notes that the study has a few caveats: The immune system in the gut may not reflect that in other tissues; the fetal tissue was limited to the second trimester, and the neonatal tissue was not obtained from completely healthy infants.
In the future, the researchers plan to study exactly what the fetal immune system is exposed to in the womb and whether it can be manipulated to benefit the growing fetus. The hope, according to Konnikova, is that the immune system can be monitored or manipulated before birth, potentially leading to diagnoses of disease at an extremely early stage or developing beneficial maternal vaccines.
Funding: The study was funded by Pitt.
Additional authors on this study include Stephanie Stras, Jessica Toothaker, Collin McCourt, Austin Oldham, and Oluwabunmi Olaloye all of Pitt; and Lael Warner, Ph.D., Yu Nee Lee, Ph.D., Erez Rechavi, M.D., and Dror S. Shouval, M.D., all of Tel Aviv University in Israel.
Source:
University of Pittsburgh
Media Contacts:
Arvind Suresh – University of Pittsburgh
Image Source:
The image is credited to Cell Press/Konnikova Lab.
Original Research: Open access
“Maturation of the Human Intestinal Immune System Occurs Early in Fetal Development”. Stephanie F. Stras, Lael Werner, Jessica M. Toothaker, Oluwabunmi O. Olaloye, Austin L. Oldham, Collin C. McCourt, Yu Nee Lee, Erez Rechavi, and others.
Developmental Cell doi:10.1016/j.devcel.2019.09.008.
Abstract
Maturation of the Human Intestinal Immune System Occurs Early in Fetal Development
Highlights
• CyTOF analysis of human 2nd trimester intestinal tissue shows high cellular diversity
• CD4+ and CD8+ TRM T cells that secrete TNFα present in fetal and infant intestines
• Diverse intestinal T and B cell receptor profiles exist in early 2nd trimester
• Shared T cell clones are abundant in the fetal intestine
Summary
There are limited data on fetal and early life development of human intestinal immunity. Using mass cytometry (CyTOF) and next-generation sequencing of B and T cell receptor (BCR and TCR) repertoires, we demonstrate complex intestinal immunity from 16 weeks’ gestational age (GA). Both BCR and TCR repertoires are diverse with CDRH and CDR3β length increasing with advancing GA. The difference-from-germline, CDR insertions and/or deletions, similarly occur in utero for TCR but not BCR, suggesting earlier mucosal T than B cell maturity. Innate immunity is dominated by macrophages, dendritic cells (DCs), innate lymphoid cells (ILCs), and natural killer (NK) cells. Follicular and transitional B cells are enriched in fetuses while CD69+IgM+ B cells are abundant in infants. Both CD4+ and CD8+ T cells are abundant, capable of secreting cytokines and are phenotypically of the tissue resident memory state in utero. Our data provide the foundation for a 2nd trimester and infant intestinal immune atlas and suggest that a complex innate and adaptive immune landscape exists significantly earlier than previously reported.







