Summary: Teens with a particular pattern of brain development have an increased frequency of drunkenness, a new study reports. Decreased gray matter density in the frontal and temporal brain regions was associated with an increased risk of teenage over-drinking.
Source: King’s College London
A new study led by researchers at King’s College London has found that adolescents with particular patterns of brain development report an increased frequency in drunkenness. The research was published today in JAMA Psychiatry.
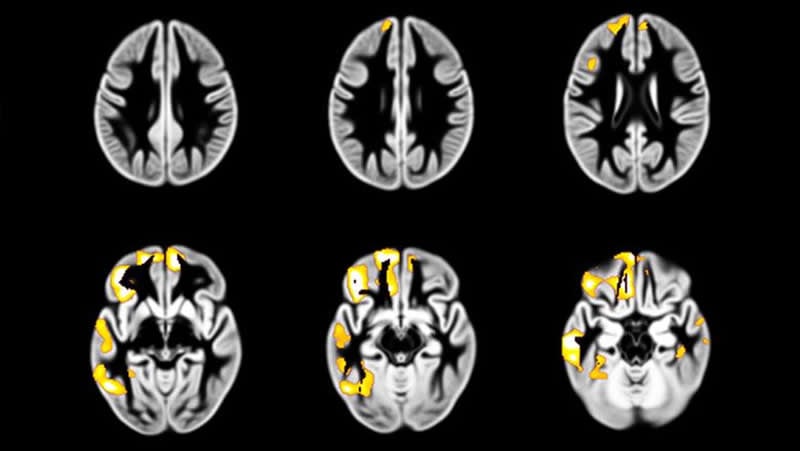
Using brain imaging data collected from 726 healthy adolescents, the researchers analysed changes in the volume of grey matter and in the frequency of drunkenness from the age of 14 years to 19 years. The results showed that those who experienced decreases in grey matter in the frontal and temporal regions of the brain over this five year period also showed an increase in how often they reported getting drunk.
Drunkenness is described as behaviours that indicate a strong intoxication, such as staggering when walking, not being able to speak properly, vomiting or not remembering what happened. Adolescents were asked how often they experienced drunkenness in the last 12 months.
There is continuing debate about how much alcohol causes changes in brain structure in adolescents or if there is a path of structural development in the brain that influences behaviour, which may put certain adolescents at greater risk of drunkenness. This new study puts into question previous interpretations of research in this area which suggest drunkenness has a harmful effect on the developing brain of healthy adolescents. Its findings indicate that structural differences in the grey matter of some healthy adolescents could predispose them to certain behaviours which result in more frequent drunkenness. The study does not investigate changes in brain structure in adolescents who were drinking heavily.
The association between changes in grey matter in the brain over time and increased drunkenness in girls was particularly strong. The research team also investigated the role of impulsivity and found that only boys showed an association between impulsivity and increased drunkenness, suggesting there may be independent developmental pathways leading to drunkenness for boys that is different from that in girls.
“Our research showed that, in this group of healthy European adolescents, brain changes in the frontal and temporal lobes might happen even before the onset of alcohol use. This means that claims that teenage drinking will damage your brain are over-simplistic and do not reflect the complexity of the interactions between brain development and the environment. In adolescents who are not drinking heavily, structural changes in the brain could in fact be a predictor of alcohol use and more research is needed to identify possible risk factors that could ultimately help characterise those individuals.” Commented Professor Gunter Schumann from the Institute of Psychiatry, Psychology & Neuroscience (IoPPN), King’s College London.
The study investigated the relationship between changes in the volume of grey matter in the brain, the experience of getting drunk and personality measures such as impulsivity and openness.
The data was sourced from the European Union-funded FP6 Integrated Project IMAGEN study which has collected MRI brain scans and data from healthy adolescents from the UK, France, Germany and Ireland at 14 years old, 16 years old and 19 years old. The follow-up at 19 years was funded by the Medical Research Council (MRC) and the German Federal Ministry of Research & Education (BMBF). The relationship between heavy alcohol use and brain development in adolescents was not studied.
Huge developmental changes occur in the brain during adolescence and this is also the time when individuals tend to start substance use so there is a longstanding debate about the causality between brain development, drug use and mental disorders. Our findings indicate that certain patterns of brain development can promote certain behaviours and, under given circumstances, this could result in an increased frequency of drunkenness. To get a more precise overview of the role of brain development in substance use disorders, we would like to focus on the individuals with the most severe decreases in grey matter and monitor the onset of substance use disorders over time.” Said Dr Gabriel Robert from the IoPPN and the University of Rennes.
The research was published in JAMA Psychiatry. There were two co-lead researchers: Gabriel Robert from King’s College London and the University of Rennes 1, France and Qiang Luo from Fudan University, Shanghai.
Source:
King’s College London
Media Contacts:
Franca Davenport – King’s College London
Image Source:
The image is credited to King’s College London.
Original Research: Open access
“Association of Gray Matter and Personality Development With Increased Drunkenness Frequency During Adolescence”. Gunter Schumann et al.
New England Journal of Medicine doi:10.1001/jamapsychiatry.2019.4063.
Abstract
Association of Gray Matter and Personality Development With Increased Drunkenness Frequency During Adolescence
Importance
Alcohol abuse correlates with gray matter development in adolescents, but the directionality of this association remains unknown.
Objective
To investigate the directionality of the association between gray matter development and increase in frequency of drunkenness among adolescents.
Design, Setting, and Participants
This cohort study analyzed participants of IMAGEN, a multicenter brain imaging study of healthy adolescents in 8 European sites in Germany (Mannheim, Dresden, Berlin, and Hamburg), the United Kingdom (London and Nottingham), Ireland (Dublin), and France (Paris). Data from the second follow-up used in the present study were acquired from January 1, 2013, to December 31, 2016, and these data were analyzed from January 1, 2016, to March 31, 2018. Analyses were controlled for sex, site, socioeconomic status, family history of alcohol dependency, puberty score, negative life events, personality, cognition, and polygenic risk scores. Personality and frequency of drunkenness were assessed at age 14 years (baseline), 16 years (first follow-up), and 19 years (second follow-up). Structural brain imaging scans were acquired at baseline and second follow-up time points.
Main Outcomes and Measures
Increases in drunkenness frequency were measured by latent growth modeling, a voxelwise hierarchical linear model was used to observe gray matter volume, and tensor-based morphometry was used for gray matter development. The hypotheses were formulated before the data analyses.
Results
A total of 726 adolescents (mean [SD] age at baseline, 14.4 [0.38] years; 418 [58%] female) were included. The increase in drunkenness frequency was associated with accelerated gray matter atrophy in the left posterior temporal cortex (peak: t1,710 = –5.8; familywise error (FWE)–corrected P = 7.2 × 10−5; cluster: 6297 voxels; P = 2.7 × 10−5), right posterior temporal cortex (cluster: 2070 voxels; FWE-corrected P = .01), and left prefrontal cortex (peak: t1,710 = –5.2; FWE-corrected P = 2 × 10−3; cluster: 10 624 voxels; P = 1.9 × 10−7). According to causal bayesian network analyses, 73% of the networks showed directionality from gray matter development to drunkenness increase as confirmed by accelerated gray matter atrophy in late bingers compared with sober controls (n = 20 vs 60; β = 1.25; 95% CI, −2.15 to −0.46; t1,70 = 0.3; P = .004), the association of drunkenness increase with gray matter volume at age 14 years (β = 0.23; 95% CI, 0.01-0.46; t1,584 = 2; P = .04), the association between gray matter atrophy and alcohol drinking units (β = −0.0033; 95% CI, −6 × 10−3 to −5 × 10−4; t1,509 = −2.4; P = .02) and drunkenness frequency at age 23 years (β = −0.16; 95% CI, −0.28 to −0.03; t1,533 = −2.5; P = .01), and the linear exposure-response curve stratified by gray matter atrophy and not by increase in frequency of drunkenness.
Conclusions and Relevance
This study found that gray matter development and impulsivity were associated with increased frequency of drunkenness by sex. These results suggest that neurotoxicity-related gray matter atrophy should be interpreted with caution.






