Summary: Researchers have identified and isolated a gut bacterium which appears to have a significant link to depression.
Source: DOE/Argonne National Laboratory.
Research team studies the compelling connection between one of NIH’s “most wanted” bacteria and mental health.
Researchers have established a correlation between depression and a group of neurotransmitter-producing bacteria found in the human gut.
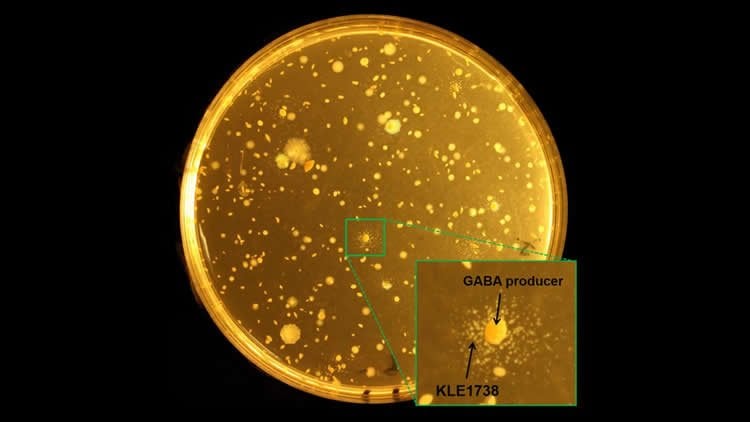
The research team from the U.S. Department of Energy’s (DOE) Argonne National Laboratory, Northeastern University and elsewhere made the connection by first isolating the KLE1738, a bacterium that has a surprising dependency upon a brain chemical called gamma-aminobutyric acid (GABA).
“The association of microbial GABAmetabolism with mental health is highly compelling,” said Jack Gilbert, group leader for microbial ecology at Argonne who also holds new faculty appointments at the University of California, San Diego, in the Department of Pediatrics and at Scripps Institution of Oceanography. “The general ability of the microbiome to produce and/or consume GABA has not been as broadly described before, and a bacterium dependent on GABAhas never been reported.”
Gilbert and 18 co-authors published their findings on December 10, 2018, in Nature Microbiology.
“Because of its unique growth requirements, nobody else has reported growing KLE1738,” said Philip Strandwitz, the article’s lead author and a postdoctoral research associate at Northeastern University’s Antimicrobial Discovery Center. Strandwitz and his colleagues have proposed the name Evtepia gabavorous for KLE1738. They will more fully describe the bacterium in a future publication.
KLE1738 had previously appeared on the “most wanted list” of the National Institutes of Health, meaning that it had yet to be cultured, despite its relative prevalence in the human gut. The bacterium has been detected in nearly 20 percent of the human gut microbiomes available in the Integrated Microbial Next Generation Sequencing Database.
Gut microbiota, the entire collection of microorganisms found in that habitat, affect many important functions, including the immune response and the nervous system. Nevertheless, many microorganisims residing in the human gut remain uncultured, which the research team called “an obstacle for understanding their biological roles” in the Nature Microbiology article.
More such microorganisms probably remain uncultured because they require key growth factors that are provided by neighboring bacteria in their natural environments, but not under artificial laboratory conditions. During an extensive screening process, the team found that KLE1738 required the presence of Bacteroides fragilis, a common human gut bacterium, to grow.
Further biological testing and purification led to the isolation of GABA as the growth factor produced by Bacteroides fragilis. GABA was, in fact, the only nutrient tested during the experiments that supported the growth of KLE1738.
In the next research phase, the team explored the possible connection between Bacteroides and depression. Stool samples and functional magnetic resonance imaging measurements of brain activity were collected from 23 subjects suffering from clinically diagnosed depression.
The researchers found an inverse relationship between the relative abundance of fecal Bacteroidesand functional connectivity in a part of the brain associated with elevated activity during depression. This means that low abundance of Bacteroides was associated with high activity in that part of the brain, and vice versa.
“A good first step is to repeat our findings in additional human cohorts, which we are actively exploring,” said Strandwitz of further research. “When it comes to depression, animal models are often difficult to translate, which is why we are so excited about human studies. ”
Recent work published in the journals Science and Cell have identified the presence of sensory neurons in the gut that are hard-wired to the brain. “It would be great to explore whether microbial GABA can act as a signal via that pathway,” said Anukriti Sharma, a co-author of the Nature Microbiology article and a postdoctoral scholar at Argonne.
Strandwitz and co-author Kim Lewis, a distinguished university professor at Northeastern, have founded a biotechnology company, Holobiome, to develop microbiome-based therapeutics that target diseases of the nervous system. Gilbert is a member of the company’s scientific advisory board. Additional research will be needed, however, before it may become possible to develop a treatment for people suffering from depression.
“Significant work must be done to first, validate the link between microbial GABA producers and depression,” Strandwitz said. “And second, if validated, identify the right approach to develop bacterial — or some sort of intervention — as therapeutics.”
Funding: National Institutes of Health, NIH/National Institute of General Medical Sciences funded this study.
Source: Brian Grabowski – DOE/Argonne National Laboratory
Publisher: Organized by NeuroscienceNews.com.
Image Source: NeuroscienceNews.com image is credited to Philip Strandwitz / Northeastern Universityy.
Original Research: Abstract for “GABA-modulating bacteria of the human gut microbiota” by Philip Strandwitz, Ki Hyun Kim, Darya Terekhova, Joanne K. Liu, Anukriti Sharma, Jennifer Levering, Daniel McDonald, David Dietrich, Timothy R. Ramadhar, Asama Lekbua, Nader Mroue, Conor Liston, Eric J. Stewart, Marc J. Dubin, Karsten Zengler, Rob Knight, Jack A. Gilbert, Jon Clardy & Kim Lewis in Nature Microbiology. Published February 2019.
doi:10.1038/s41564-018-0307-3
[cbtabs][cbtab title=”MLA”]DOE/Argonne National Laboratory”Newly Isolated Human Gut Bacterium Reveals Possible Link to Depression.” NeuroscienceNews. NeuroscienceNews, 13 February 2019.
<https://neurosciencenews.com/depression-gut-bacterium-10731/>.[/cbtab][cbtab title=”APA”]DOE/Argonne National Laboratory(2019, February 13). Newly Isolated Human Gut Bacterium Reveals Possible Link to Depression. NeuroscienceNews. Retrieved February 13, 2019 from https://neurosciencenews.com/depression-gut-bacterium-10731/[/cbtab][cbtab title=”Chicago”]DOE/Argonne National Laboratory”Newly Isolated Human Gut Bacterium Reveals Possible Link to Depression.” https://neurosciencenews.com/depression-gut-bacterium-10731/ (accessed February 13, 2019).[/cbtab][/cbtabs]
Abstract
GABA-modulating bacteria of the human gut microbiota
The gut microbiota affects many important host functions, including the immune response and the nervous system. However, while substantial progress has been made in growing diverse microorganisms of the microbiota, 23–65% of species residing in the human gut remain uncultured, which is an obstacle for understanding their biological roles. A likely reason for this unculturability is the absence in artificial media of key growth factors that are provided by neighbouring bacteria in situ. In the present study, we used co-culture to isolate KLE1738, which required the presence of Bacteroides fragilis to grow. Bioassay-driven purification of B. fragilis supernatant led to the isolation of the growth factor, which, surprisingly, is the major inhibitory neurotransmitter GABA (γ-aminobutyric acid). GABA was the only tested nutrient that supported the growth of KLE1738, and a genome analysis supported a GABA-dependent metabolism mechanism. Using growth of KLE1738 as an indicator, we isolated a variety of GABA-producing bacteria, and found that Bacteroides ssp. produced large quantities of GABA. Genome-based metabolic modelling of the human gut microbiota revealed multiple genera with the predicted capability to produce or consume GABA. A transcriptome analysis of human stool samples from healthy individuals showed that GABA-producing pathways are actively expressed by Bacteroides, Parabacteroides and Escherichia species. By coupling 16S ribosmal RNA sequencing with functional magentic resonance imaging in patients with major depressive disorder, a disease associated with an altered GABA-mediated response, we found that the relative abundance levels of faecal Bacteroides are negatively correlated with brain signatures associated with depression.






