Summary: A new study reports neuroinflammation could have a direct involvement in the development of CTE.
Source: Boston University Medical Center.
For the first time, researchers have shown that inflammation in the brain may have direct involvement in the development of chronic traumatic encephalopathy (CTE). In addition, they found that the number of years one plays contact sports may predict the occurrence of CTE and that this association is partly due to increased inflammation in the brain.
The findings, which appear in online in Acta Neuropathologica Communications, are important steps in understanding how CTE develops and may help efforts to identify and treat CTE during life.
CTE is a progressive degenerative disease of the brain found in athletes and others with a history of repetitive brain trauma, including symptomatic concussions as well as asymptomatic subconcussive hits to the head.
Brains from former American football players and non-athlete controls were examined after death for CTE pathology and markers of inflammation in the brain. Researchers from Boston University School of Medicine (BUSM) and the VA Boston Healthcare System studied the numbers of inflammatory cells in the frontal cortex of the brain using markers for different cell types. They then compared the number of years playing football to the numbers of inflammatory cells, the development of CTE pathology, and the presence of dementia in life. A statistical model then tested the hypothesis that the number of years of exposure to football predicted brain inflammation, CTE pathology and the development of dementia.
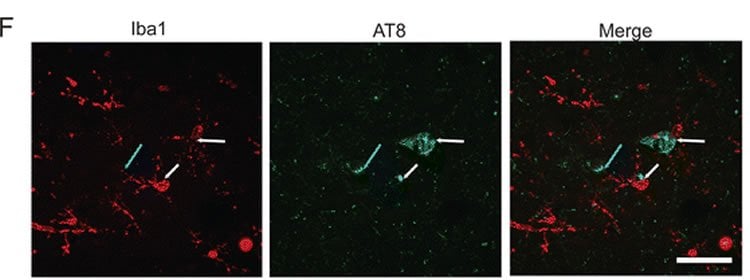
“This study provides evidence that playing football for a prolonged period can result in long-term brain inflammation and that this inflammation might lead to CTE,” said first author Jonathan Cherry, PhD, postdoctoral fellow in neurology at BUSM. “Although inflammation may be protective in the brain especially right after an injury, our study suggests that years after a period of playing football inflammation can persist in the brain and is linked to the development of CTE,” he added.
According to the researchers inflammation has an important role in a number of other degenerative diseases such as Alzheimer’s disease, Parkinson’s disease, and amyotrophic lateral sclerosis, and injury from repetitive head impacts and may play a role in the development of these diseases as well.
The researchers believe that future studies are needed to determine whether treating this inflammation can prevent or lessen the development of CTE. “Furthermore, brain inflammation could be used as a predictive biomarker to help identify patients at risk of developing CTE in life,” said Cherry.
Funding: Funding for this study was provided by National Institute of Neurological Disorders and Stroke, National Institute of Aging, Department of Veterans Affairs, Alzheimer’s Association, and the Concussion Legacy Foundation.
Source: Gina DiGravio – Boston University Medical Center
Image Source: This NeuroscienceNews.com image is credited to Cherry et al./Acta Neuropathologica Communications.
Original Research: Full open access research for “Microglial neuroinflammation contributes to tau accumulation in chronic traumatic encephalopathy” by Jonathan D. Cherry, Yorghos Tripodis, Victor E. Alvarez, Bertrand Huber, Patrick T. Kiernan, Daniel H. Daneshvar, Jesse Mez, Philip H. Montenigro, Todd M. Solomon, Michael L. Alosco, Robert A. Stern, Ann C. McKee and Thor D. Stein in Acta Neuropathologica Communications. Published online October 28 2016 doi:10.1186/s40478-016-0382-8
[cbtabs][cbtab title=”MLA”]Boston University Medical Center. “Connection Between Brain Inflammation and CTE Identified.” NeuroscienceNews. NeuroscienceNews, 2 November 2016.
<https://neurosciencenews.com/cte-neuroinflammation-neurology-5411/>.[/cbtab][cbtab title=”APA”]Boston University Medical Center. (2016, November 2). Connection Between Brain Inflammation and CTE Identified. NeuroscienceNews. Retrieved November 2, 2016 from https://neurosciencenews.com/cte-neuroinflammation-neurology-5411/[/cbtab][cbtab title=”Chicago”]Boston University Medical Center. “Connection Between Brain Inflammation and CTE Identified.” https://neurosciencenews.com/cte-neuroinflammation-neurology-5411/ (accessed November 2, 2016).[/cbtab][/cbtabs]
Abstract
Microglial neuroinflammation contributes to tau accumulation in chronic traumatic encephalopathy
The chronic effects of repetitive head impacts (RHI) on the development of neuroinflammation and its relationship to chronic traumatic encephalopathy (CTE) are unknown. Here we set out to determine the relationship between RHI exposure, neuroinflammation, and the development of hyperphosphorylated tau (ptau) pathology and dementia risk in CTE. We studied a cohort of 66 deceased American football athletes from the Boston University-Veteran’s Affairs-Concussion Legacy Foundation Brain Bank as well as 16 non-athlete controls. Subjects with a neurodegenerative disease other than CTE were excluded. Counts of total and activated microglia, astrocytes, and ptau pathology were performed in the dorsolateral frontal cortex (DLF). Binary logistic and simultaneous equation regression models were used to test associations between RHI exposure, microglia, ptau pathology, and dementia. Duration of RHI exposure and the development and severity of CTE were associated with reactive microglial morphology and increased numbers of CD68 immunoreactive microglia in the DLF. A simultaneous equation regression model demonstrated that RHI exposure had a significant direct effect on CD68 cell density (p < 0.0001) and ptau pathology (p < 0.0001) independent of age at death. The effect of RHI on ptau pathology was partially mediated through increased CD68 positive cell density. A binary logistic regression demonstrated that a diagnosis of dementia was significantly predicted by CD68 cell density (OR = 1.010, p = 0.011) independent of age (OR = 1.055, p = 0.007), but this effect disappeared when ptau pathology was included in the model. In conclusion, RHI is associated with chronic activation of microglia, which may partially mediate the effect of RHI on the development of ptau pathology and dementia in CTE. Inflammatory molecules may be important diagnostic or predictive biomarkers as well as promising therapeutic targets in CTE.
“Microglial neuroinflammation contributes to tau accumulation in chronic traumatic encephalopathy” by Jonathan D. Cherry, Yorghos Tripodis, Victor E. Alvarez, Bertrand Huber, Patrick T. Kiernan, Daniel H. Daneshvar, Jesse Mez, Philip H. Montenigro, Todd M. Solomon, Michael L. Alosco, Robert A. Stern, Ann C. McKee and Thor D. Stein in Acta Neuropathologica Communications. Published online October 28 2016 doi:10.1186/s40478-016-0382-8






