Summary: The protein ACBP directly influences neurons that help both rodents and humans maintain a healthy weight.
Source: CRCHUM
Regardless of how much you exercise or how balanced your diet is, controlling your weight is more brain-related than you might have thought. In a study published in the Journal of Clinical Investigation, researchers from the University of Montreal Hospital Research Centre (CRCHUM) show for the first time in mice that the acyl-CoA-binding protein, or ACBP, has a direct influence on the neurons that allow rodents and humans to maintain a healthy weight.
In April 2015, Thierry Alquier, a CRCHUM researcher and the lead author of this study, had already revealed, with his team, that this same protein allowed astrocytes, cells that support neuronal functions, to communicate variations in fatty acids and lipids in the blood to neurons. Thanks to this essential piece of information, the brain can adjust food intake and energy expenditure – and, ultimately, control its owner’s weight.
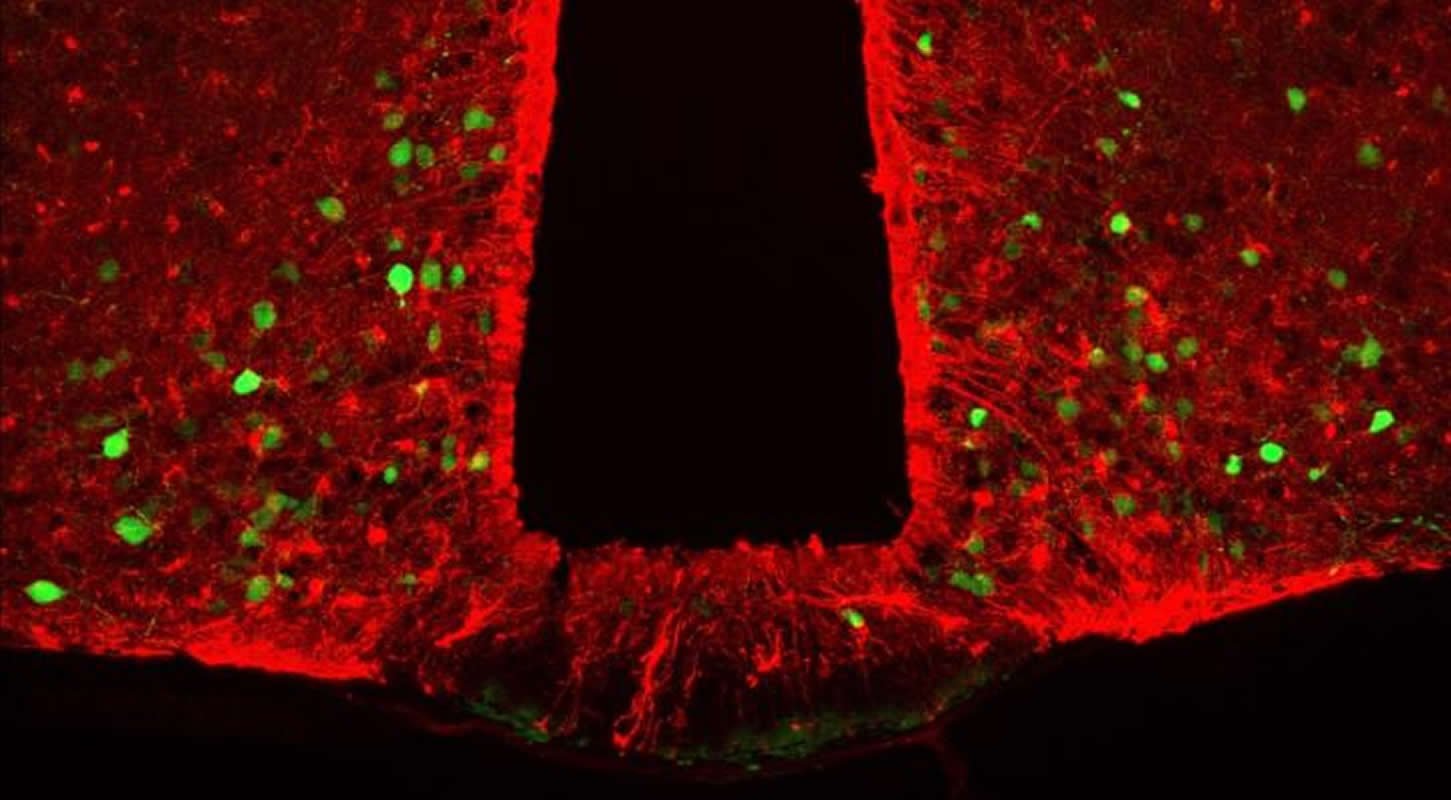
“With colleagues from the Université de Bordeaux’s NutriNeuro laboratory, we now show that neurons that reduce food intake, known as proopiomelanocortin neurons or POMC neurons, are in ‘close communication’ with astrocytes that produce the protein ACBP in a specific area of the brain: the arcuate nucleus of the hypothalamus,” said Thierry Alquier, associate professor at Université de Montréal.
Essential for the control of feeding and metabolism, this area of the hypothalamus contains two populations of neurons with opposing functions when activated: the first results in an increase in food intake; the second — POMC neurons common to animals and humans — promotes a reduction of food intake and an increase in energy expenditure.
A species issue?
“Genetic mutations explain five to 10 per cent of obesity cases,” said Alquier. “Among these cases, a large proportion is related to a disruption of this neuronal pathway commonly known as the melanocortin pathway. We observed that the deletion of the ACBP gene in astrocytes of the arcuate nucleus promotes obesity. In mice that were genetically modified to be obese, we observed in the laboratory that injecting them daily with ACBP led to a reduction of food intake and weight loss in the order of 5 per cent over five days, a mechanism that relies on the activation of POMC neurons.”
However, the researcher urged caution in translating this discovery to humans. This study is at the basic research stage and was carried out in the laboratory on mice.
Recognized by the World Health Organization as a global public health problem, obesity is a major risk factor for certain chronic illnesses, such as type 2 diabetes, cardiovascular diseases and certain cancers, and for musculoskeletal disorders and premature death.
Funding: This research was funded by the Canadian Institutes of Health Research; the Cardiometabolic Health, Diabetes and Obesity Research Network of the Fonds de Recherche du Québec-Santé; Diabetes Québec; Diabetes Canada; the Marie Curie Foundation; the Société Francophone du Diabète; the French National Institute for Health and Research and the French National Research Agency.
Source:
CRCHUM
Media Contacts:
Bruno Geoffroy – CRCHUM
Image Source:
The image is credited to Khalil Bouyakdan / CHUM 2019.
Original Research: Open access
“The gliotransmitter ACBP controls feeding and energy homeostasis via the melanocortin system”. Khalil Bouyakdan et al.
Journal of Clinical Investigation. doi:10.1172/JCI123454
Abstract
The gliotransmitter ACBP controls feeding and energy homeostasis via the melanocortin system
Glial cells have emerged as key players in the central control of energy balance and etiology of obesity. Astrocytes play a central role in neural communication via the release of gliotransmitters. Acyl-CoA–binding protein–derived (ACBP-derived) endozepines are secreted peptides that modulate the GABAA receptor. In the hypothalamus, ACBP is enriched in arcuate nucleus (ARC) astrocytes, ependymocytes, and tanycytes. Central administration of the endozepine octadecaneuropeptide (ODN) reduces feeding and improves glucose tolerance, yet the contribution of endogenous ACBP in energy homeostasis is unknown. We demonstrated that ACBP deletion in GFAP+ astrocytes, but not in Nkx2.1-lineage neural cells, promoted diet-induced hyperphagia and obesity in both male and female mice, an effect prevented by viral rescue of ACBP in ARC astrocytes. ACBP+ astrocytes were observed in apposition with proopiomelanocortin (POMC) neurons, and ODN selectively activated POMC neurons through the ODN GPCR but not GABAA, and suppressed feeding while increasing carbohydrate utilization via the melanocortin system. Similarly, ACBP overexpression in ARC astrocytes reduced feeding and weight gain. Finally, the ODN GPCR agonist decreased feeding and promoted weight loss in ob/ob mice. These findings uncover ACBP as an ARC gliopeptide playing a key role in energy balance control and exerting strong anorectic effects via the central melanocortin system.






