Summary: A new discovery could help answer the question as to how extra ApoE4 may cause Alzheimer’s disease.
Source: Salk Institute.
For decades, scientists have known that people with two copies of a gene called apolipoprotein E4 (ApoE4) are much more likely to have Alzheimer’s disease at age 65 than the rest of the population. Now, researchers at the Salk Institute have identified a connection between ApoE4 and protein build-up associated with Alzheimer’s that provides a possible biochemical explanation for how extra ApoE4 causes the disease.
“The big picture here is that we’ve found a very different way of thinking about how the proteins in Alzheimer’s disease might be regulated,” says Alan Saghatelian, Salk professor and holder of the Dr. Frederik Paulsen Chair in Salk’s Clayton Foundation Laboratories for Peptide Biology. Their findings, which appear in the August 2016 issue of the Journal of the American Chemical Society underscore the importance of looking at genes and proteins not classically associated with Alzheimer’s to make progress in understanding the disease.
Late-onset Alzheimer’s disease–the subset of the disorder occurring in people age 65 and over–affects more than 5 million Americans, and is characterized by progressive memory loss and dementia. Scientists have put forth a variety of hypotheses on its causes, including the accumulation of protein clusters called beta-amyloid plaques and tau tangles in the brain.
Apolipoprotein E comes in three versions, or variants, called ApoE2, ApoE3 and ApoE4. All the ApoE proteins have the same normal function: carrying fats, cholesterols and vitamins throughout the body, including into the brain. While ApoE2 is protective and ApoE3 appears to have no effect, a mutation in ApoE4 is a well-established genetic risk factor for late-onset Alzheimer’s disease. Previous reports have suggested that ApoE4 may affect how the brain clears out beta-amyloid, but what was happening at the molecular level wasn’t clear.
“ApoE4 is the most predictive genetic change for late onset Alzheimer’s, but no one has really understood what’s going on at the molecular level,” says Saghatelian. Scientists had previously uncovered hints, however, that ApoE4 might degrade differently than the other variants, but the protein that carried out this breakdown of ApoE4 was unknown.
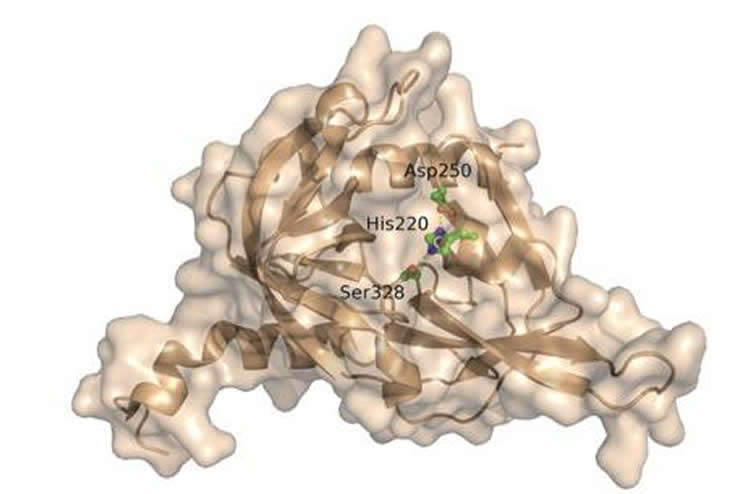
To find the protein responsible for degrading ApoE4, Saghatelian and research associate Qian Chu, first author of the new paper, screened tissues for potential suspects and homed in on one enzyme called high-temperature requirement serine peptidase A1 (HtrA1).
When they compared how HtrA1 degraded ApoE4 with ApoE3, they found that the enzyme processed more ApoE4 than ApoE3, chewing ApoE4 into smaller, less stable fragments. The researchers confirmed the observation in both isolated proteins and human cells. The finding suggests that people with ApoE4 could have less ApoE overall in their brain cells–and more of the breakdown products of the protein.
“There’s been an idea tossed around that ApoE4 breakdown products could be toxic,” said Saghatelian. “Now, knowing the enzyme that breaks it down, we have a way to actually test this idea.”
But it’s not just a lack of full-length ApoE or an increase in its fragments that may be causing Alzheimer’s in people with ApoE4. Saghatelian and Chu also found that ApoE4–because it binds so well to HtrA1–keeps the enzyme from breaking down the tau protein, responsible for tau tangles associated with Alzheimer’s.
“People have thought about tau or amyloid beta as things that cause Alzheimer’s, but this suggests that we need to think more globally about proteins that could be impacting tau or amyloid through biochemical pathways,” Saghatelian said.
The results need be tested and confirmed in animal studies before researchers can be sure that HtrA1 is the link between ApoE4 and Alzheimer’s in humans. But if they hold true, they could point toward a better understanding of the disease and potential new treatment strategies.
Other researchers on the study were Jolene K. Diedrich, Joan M. Vaughan, Cynthia J. Donaldson, Michael F. Nunn, and Kuo-Fen Lee of the Salk Institute.
Funding: The work and the researchers involved were supported by grants from the National Institutes of Health, the Clayton Foundation, the Schlink Foundation, the Gemcon Family Foundation, the Hewitt Fellowship, the Joe W. and Dorothy Dorsett Brown Foundation, the Helen McLoraine Chair in Molecular Neurobiology, the National Cancer Center and the Leona M. and Harry B. Helmsley Charitable Trust.
Source: Salk Institute
Image Source: This NeuroscienceNews.com image is credited to Salk Institute.
Original Research: Abstract for “HtrA1 Proteolysis of ApoE In Vitro Is Allele Selective” by Qian Chu, Jolene K. Diedrich, Joan M. Vaughan, Cynthia J. Donaldson, Michael F. Nunn, Kuo-Fen Lee, and Alan Saghatelian in Journal of the American Chemical Society. Published online July 5 2016 doi:10.1021/jacs.6b03463
[cbtabs][cbtab title=”MLA”]Salk Institute. “New Mechanism Discovered for Alzheimer’s Risk Gene.” NeuroscienceNews. NeuroscienceNews, 18 August 2016.
<https://neurosciencenews.com/apoe4-alzheimers-genetics-4868/>.[/cbtab][cbtab title=”APA”]Salk Institute. (2016, August 18). New Mechanism Discovered for Alzheimer’s Risk Gene. NeuroscienceNew. Retrieved August 18, 2016 from https://neurosciencenews.com/apoe4-alzheimers-genetics-4868/[/cbtab][cbtab title=”Chicago”]Salk Institute. “New Mechanism Discovered for Alzheimer’s Risk Gene.” https://neurosciencenews.com/apoe4-alzheimers-genetics-4868/ (accessed August 18, 2016).[/cbtab][/cbtabs]
Abstract
HtrA1 Proteolysis of ApoE In Vitro Is Allele Selective
Apolipoprotein E (ApoE) belongs to a large class of proteins that solubilize lipids for physiological transport. Humans have three different APOE alleles, APOE ε2, APOE ε3, and APOE ε4, and genetic studies identified ApoE4 as the strongest genetic risk factor for Alzheimer’s disease (AD). People who are homozygous for ApoE4 (i.e., ApoE4/E4) are an order of magnitude more likely to develop late-onset AD (LOAD) than ApoE3/E3 carriers. Several differences between ApoE3 and ApoE4 may contribute to AD including the observation that ApoE4 is degraded to a greater extent than ApoE3 in the human brain. Experiments with high-temperature requirement serine peptidase A1 (HtrA1), which is found in the nervous system, demonstrate that HtrA1 is an allele-selective ApoE-degrading enzyme that degrades ApoE4 more quickly than ApoE3. This activity is specific to HtrA1, as similar assays with HtrA2 showed minimal ApoE4 proteolysis and trypsin had no preference between ApoE4 and ApoE3. HtrA1 has also been reported to cleave the tau protein (Tau) and the amyloid protein precursor (APP) to hinder the formation of toxic amyloid deposits associated with AD. Competition assays with ApoE4, ApoE3, and Tau revealed that ApoE4 inhibits Tau degradation. Thus, the identification of ApoE4 as an in vitro HtrA1 substrate suggests a potential biochemical mechanism that links ApoE4 regulation of AD proteins such as Tau.
“HtrA1 Proteolysis of ApoE In Vitro Is Allele Selective” by Qian Chu, Jolene K. Diedrich, Joan M. Vaughan, Cynthia J. Donaldson, Michael F. Nunn, Kuo-Fen Lee, and Alan Saghatelian in Journal of the American Chemical Society. Published online July 5 2016 doi:10.1021/jacs.6b03463






