Summary: Researchers have discovered a new cellular mechanism that may be a root cause of multiple sclerosis.
Source: University of Exeter.
A new study has made a major new discovery towards finding the cause of multiple sclerosis, potentially paving the way for research to investigate new treatments.
Ahead of MS Awareness Week, which starts today (Monday April 24), an international team involving the University of Exeter Medical School and the University of Alberta has discovered a new cellular mechanism– an underlying defect in brain cells — that may cause the disease, and a potential hallmark that may be a target for future treatment of the autoimmune disorder.
The study was recently published in the Journal of Neuroinflammation and part funded by the Royal Devon & Exeter NHS Foundation Trust.
Professor Paul Eggleton, of the University of Exeter Medical School, said: “Multiple sclerosis can have a devastating impact on people’s lives, affecting mobility, speech, mental ability and more. So far, all medicine can offer is treatment and therapy for the symptoms – as we do not yet know the precise causes, research has been limited. Our exciting new findings have uncovered a new avenue for researchers to explore. It is a critical step, and in time, we hope it might lead to effective new treatments for MS.”
Multiple sclerosis affects around 2.5 million people around the world. Typically, people are diagnosed in their 20s and 30s, and it is more common in women than men.
Although the cause has so far been a mystery, the disease causes the body’s own immune system to attack myelin – the fatty “sheaths” that protect nerves in the brain and spinal cord. This leads to brain damage, a reduction in blood supply and oxygen and the formation of lesions in the body. Symptoms can be wide-ranging, and can include muscle spasms, mobility problems, pain, fatigue, and problems with speech.
Scientists have long suspected that mitochondria, the energy-creating “powerhouse” of the cell, plays a link in causing multiple sclerosis.
The joint Exeter-Alberta research team was the first to combine clinical and laboratory experiments to explain how mitochondria becomes defective in people with MS. Using human brain tissue samples , they found that a protein called Rab32 is present in large quantities in the brains of people with MS, but is virtually absent in healthy brain cells.
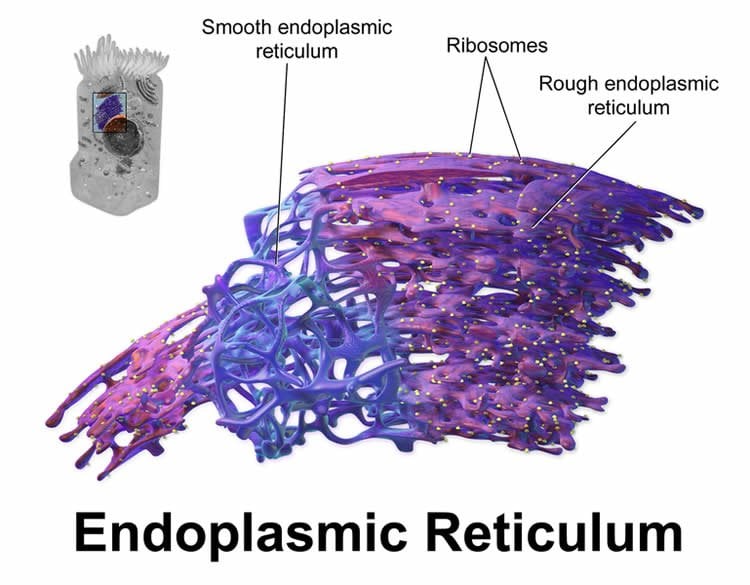
Where Rab32 is present, the team discovered that a part of the cell that stores calcium (endoplasmic reticulum or ER) gets too close to the mitochondria. The resulting miscommunication with the calcium supply triggers the mitochondria to misbehave, ultimately causing toxicity for brain cells people with MS.
Researchers do not yet know what causes an unwelcome influx of Rab32 but they believe the defect could originate at the base of the ER organelle.
The finding will enable scientists to search for effective treatments that target Rab32 and embark on determining whether there are other proteins that may pay a role in triggering MS.
Dr David Schley, Research Communications Manager at the MS Society, said:
“No one knows for sure why people develop MS and we welcome any research that increases our understanding of how to stop it. There are currently no treatments available for many of the more than 100,000 people in the UK who live with this challenging and unpredictable condition. We want people with MS to have a range of treatments to choose from, and be able to get the right treatment at the right time.”
Source: Louise Vennells – University of Exeter
Image Source: NeuroscienceNews.com image is credited to BruceBlaus and is licensed CC BY 3.0.
Original Research: Full open access research for “Rab32 connects ER stress to mitochondrial defects in multiple sclerosis” by Yohannes Haile, Xiaodan Deng, Carolina Ortiz-Sandoval, Nasser Tahbaz, Aleksandra Janowicz, Jian-Qiang Lu, Bradley J. Kerr, Nicholas J. Gutowski, Janet E. Holley, Paul Eggleton, Fabrizio Giuliani and Thomas Simmen in Journal of Neuroinflammation. Published online January 23 2017 doi:10.1186/s12974-016-0788-z
[cbtabs][cbtab title=”MLA”]University of Exeter “A Step Closer to Unraveling Mystery Cause of Multiple Sclerosis.” NeuroscienceNews. NeuroscienceNews, 24 April 2017.
<https://neurosciencenews.com/multiple-sclerosis-cause-6482/>.[/cbtab][cbtab title=”APA”]University of Exeter (2017, April 24). A Step Closer to Unraveling Mystery Cause of Multiple Sclerosis. NeuroscienceNew. Retrieved April 24, 2017 from https://neurosciencenews.com/multiple-sclerosis-cause-6482/[/cbtab][cbtab title=”Chicago”]University of Exeter “A Step Closer to Unraveling Mystery Cause of Multiple Sclerosis.” https://neurosciencenews.com/multiple-sclerosis-cause-6482/ (accessed April 24, 2017).[/cbtab][/cbtabs]
Abstract
Rab32 connects ER stress to mitochondrial defects in multiple sclerosis
Background
Endoplasmic reticulum (ER) stress is a hallmark of neurodegenerative diseases such as multiple sclerosis (MS). However, this physiological mechanism has multiple manifestations that range from impaired clearance of unfolded proteins to altered mitochondrial dynamics and apoptosis. While connections between the triggering of the unfolded protein response (UPR) and downstream mitochondrial dysfunction are poorly understood, the membranous contacts between the ER and mitochondria, called the mitochondria-associated membrane (MAM), could provide a functional link between these two mechanisms. Therefore, we investigated whether the guanosine triphosphatase (GTPase) Rab32, a known regulator of the MAM, mitochondrial dynamics, and apoptosis, could be associated with ER stress as well as mitochondrial dysfunction.
Methods
We assessed Rab32 expression in MS patient and experimental autoimmune encephalomyelitis (EAE) tissue, via observation of mitochondria in primary neurons and via monitoring of survival of neuronal cells upon increased Rab32 expression.
Results
We found that the induction of Rab32 and other MAM proteins correlates with ER stress proteins in MS brain, as well as in EAE, and occurs in multiple central nervous system (CNS) cell types. We identify Rab32, known to increase in response to acute brain inflammation, as a novel unfolded protein response (UPR) target. High Rab32 expression shortens neurite length, alters mitochondria morphology, and accelerates apoptosis/necroptosis of human primary neurons and cell lines.
Conclusions
ER stress is strongly associated with Rab32 upregulation in the progression of MS, leading to mitochondrial dysfunction and neuronal death.
“Rab32 connects ER stress to mitochondrial defects in multiple sclerosis” by Yohannes Haile, Xiaodan Deng, Carolina Ortiz-Sandoval, Nasser Tahbaz, Aleksandra Janowicz, Jian-Qiang Lu, Bradley J. Kerr, Nicholas J. Gutowski, Janet E. Holley, Paul Eggleton, Fabrizio Giuliani and Thomas Simmen in Journal of Neuroinflammation. Published online January 23 2017 doi:10.1186/s12974-016-0788-z






