Summary: Researchers identify new biomarkers associated with multiple sclerosis pathogenesis.
Source: Kazan Federal University.
Novel study of proinflammatory cytokines in serum and cerebrospinal fluid of multiple sclerosis patients was conducted by Kazan University’s Institute of Fundamental Medicine and Biology.
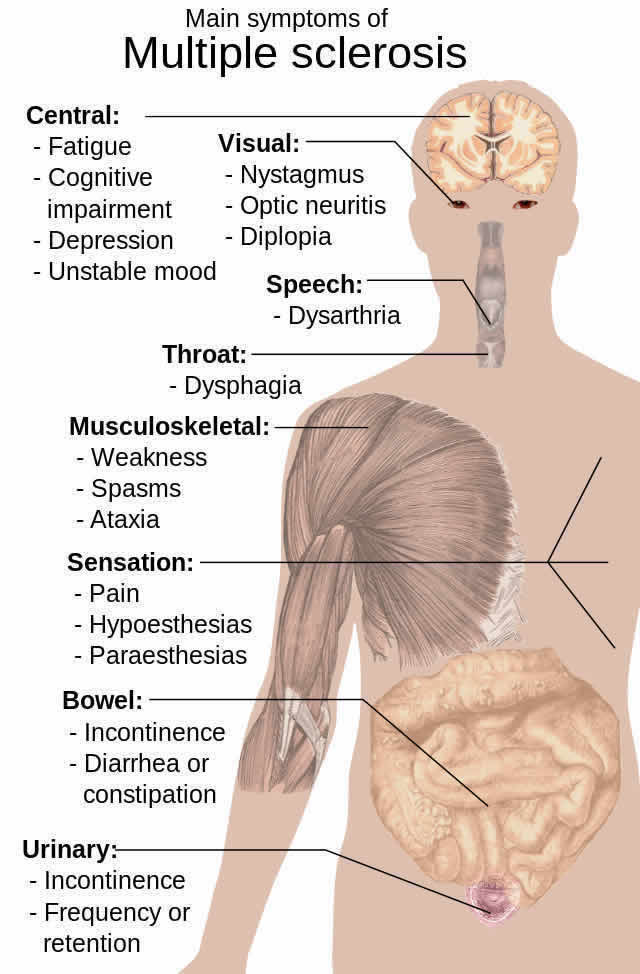
Multiple sclerosis (MS) is a chronic debilitating inflammatory disease targeting the brain. The pathogenesis of MS remains largely unknown. It is believed that brain tissue damage is due to immune cells targeting and breaking up the myelin basic protein (MBP), which is essential for nerve cells function. The majority of brain lesions is found near small veins and has prominent immune cells (lymphocytes and macrophages) infiltration, supporting the hypothesis of the brain lesions to be due to leukocyte damage to neurons.
Clinical data as well as evidence collected using animal model of MS suggests that leukocytes cross the blood-brain barrier (BBB) and localize in brain lesions.
However, it is still unclear whether inflammation in the brain is initiated within the CNS or is the result of leukocyte migration across the BBB driven by systemic inflammation.
International team led by Dr Svetlana Khaiboullina, the Leading Scientist at the Nevada Center for Biomedical Research, USA, Professor Albert Rizvanov, Chief Researcher at the Institute of Fundamental Medicine and Biology of Kazan Federal University, Russia, and Dr Timur Khaibullin, Republican Clinical Neurological Center, Kazan, Russia, presented novel data on cytokine activation in serum and cerebrospinal fluid (CSF) from multiple sclerosis (MS) patients. This data suggests a central role for interferon gamma (IFNγ) in brain inflammation in MS.
Authors propose that high serum IFNγ could activate astrocytes triggering production of a novel subset of chemokines establishing an inflammatory milieu and promoting migration of autoreactive encephalitic T lymphocytes into the brain. The study was approved by the ethical committee, supported by the Ministry of Healthcare of Tatarstan and published in Frontiers in Immunology, 18 May 2017. .
Researchers state that collected data supports the hypothesis of activation of specific subset of cytokines regulating Th1 and Th17 type immune response in MS. However, the most interesting finding was that the CSF and serum cytokine profiles differ in MS. Authors have shown an increased IFNγ and IL12(p40) levels in CSF suggesting upregulation of Th1 leukocytes in the brain, while a high level of IL17 was found in serum, indicating Th17 leukocytes activation in the circulation.
Funding:
Source: Yury Nurmeev – Kazan Federal University
Image Source: NeuroscienceNews.com image is in the public domain.
Original Research: Full open access research for “Elevated Levels of Proinflammatory Cytokines in Cerebrospinal Fluid of Multiple Sclerosis Patients” by Timur Khaibullin, Vilena Ivanova, Ekaterina Martynova, Georgy Cherepnev, Farit Khabirov, Evgenii Granatov, Albert Rizvanov and Svetlana Khaiboullina in Frontiers in Immunology. Published online May 18 2017 doi:10.3389/fimmu.2017.00531
[cbtabs][cbtab title=”MLA”]Kazan Federal University “New Biomarkers For Multiple Sclerosis Pathogenesis.” NeuroscienceNews. NeuroscienceNews, 19 May 2017.
<https://neurosciencenews.com/multiple-scleosis-pathogensis-6730/>.[/cbtab][cbtab title=”APA”]Kazan Federal University (2017, May 19). New Biomarkers For Multiple Sclerosis Pathogenesis. NeuroscienceNew. Retrieved May 19, 2017 from https://neurosciencenews.com/multiple-scleosis-pathogensis-6730/[/cbtab][cbtab title=”Chicago”]Kazan Federal University “New Biomarkers For Multiple Sclerosis Pathogenesis.” https://neurosciencenews.com/multiple-scleosis-pathogensis-6730/ (accessed May 19, 2017).[/cbtab][/cbtabs]
Abstract
Elevated Levels of Proinflammatory Cytokines in Cerebrospinal Fluid of Multiple Sclerosis Patients
Multiple sclerosis (MS) is an autoimmune neurodegenerative disease characterized by chronic brain inflammation. Leukocyte infiltration of brain tissue causes inflammation, demyelination, and the subsequent formation of sclerotic plaques, which are a hallmark of MS. Activation of proinflammatory cytokines is essential for regulation of lymphocyte migration across the blood–brain barrier. We demonstrate increased levels of many cytokines, including IL-2RA, CCL5, CCL11, MIF, CXCL1, CXCL10, IFNγ, SCF, and TRAIL, were upregulated in cerebrospinal fluid (CSF), whereas IL-17, CCL2, CCL3, CCL4, and IL-12(p40) were activated in MS serum. Interaction analysis of cytokines in CSF demonstrated a connection between IFNγ and CCL5 as well as MIF. Many cells can contribute to production of these cytokines including CD8 and Th1 lymphocytes and astrocytes. Therefore, we suggest that IFNγ released by Th1 lymphocytes can activate astrocytes, which then produce chemoattractants, including CCL5 and MIF. These chemokines promote an inflammatory milieu and interact with multiple chemokines including CCL27 and CXCL1. Of special note, upregulation of CCL27 was found in CSF of MS cases. This observation is the first to demonstrate CCL27 as a potential contributor of brain pathology in MS. Our data suggest that CCL27 may be involved in activation and migration of autoreactive encephalitogenic immune effectors in the brain. Further, our data support the role of Th1 lymphocytes in the pathogenesis of brain inflammation in MS, with several cytokines playing a central role.
“Elevated Levels of Proinflammatory Cytokines in Cerebrospinal Fluid of Multiple Sclerosis Patients” by Timur Khaibullin, Vilena Ivanova, Ekaterina Martynova, Georgy Cherepnev, Farit Khabirov, Evgenii Granatov, Albert Rizvanov and Svetlana Khaiboullina in Frontiers in Immunology. Published online May 18 2017 doi:10.3389/fimmu.2017.00531






