Summary: Researchers report dysfunctional mitophagy may contribute to the development of Alzheimer’s disease. When mitophagy is improved, symptoms of Alzheimer’s almost disappeared in animal models of the disease.
Source: University of Copenhagen.
Scientists around the world are still struggling to understand Alzheimer’s better in order to be able to treat and potentially prevent the development of the debilitating disease in the future. No new medications have been approved during recent years.
In a new study in the scientific journal Nature Neuroscience, an international team of researchers from the University of Copenhagen, National Institutes of Health and the University of Oslo among others have come closer to a new way of attacking the disease. They target the efforts towards the cleaning process in the brain cells called mitophagy.
‘When the cleaning system does not work properly, there will be an accumulation of defective mitochondria in the brain cells. And this may be really dangerous. At any rate, the poor cleaning system is markedly present in cells from both humans and animals with Alzheimer’s. And when we improve the cleaning in live animals, their Alzheimer’s symptoms almost disappear,’ says Vilhelm Bohr, author of the study and affiliate professor at the Center for Healthy Aging and National Institutes of Health.
Defect Energy Factories
The researchers have looked more closely at the cleaning process in brain cells from deceased Alzheimer’s patients, in Alzheimer’s-induced stem cells and in live mice and roundworms with Alzheimer’s. In addition, they have also tested active substances targeted at the cleaning process in the animal models.
‘It significantly strengthens our results that the cleaning process seems to be important in both human cells and across different animal species. And then it is encouraging that in living animals we are able to improve the central Alzheimer’s symptoms, memory and learning,’ says Vilhelm Bohr.
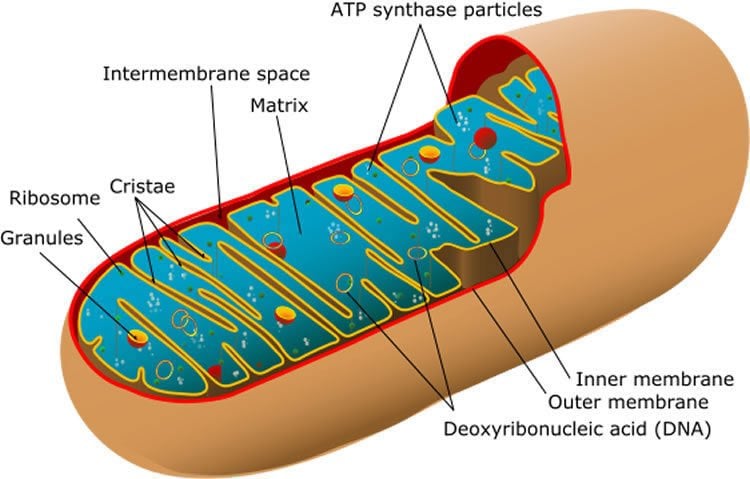
The mitochondria lie inside the cell and can be seen as the cell’s energy factories. Mitophagy breaks down defective mitochondria and reuses the proteins that they consist of. It is known from previous research that dysfunctional mitophagy is associated with poor function and survival of nerve cells, but so far, no connection with Alzheimer’s has been shown.
Slowing Down the Accumulation
In both Alzheimer’s and other states of dementia, there is an accumulation of the proteins tau and beta amyloid in the brain, leading to cell death. In the new animal models, the researchers show that when boosting the mitophagy, such accumulation will slow down.
The researchers believe that altogether their findings indicate that the cleaning process is a potential target for the treatment of Alzheimer’s, which should be further investigated. They therefore plan to start clinical trials in humans in the near future.
Funding: The research at the Center for Healthy Aging is supported by Nordea-Fonden.
The researchers behind the study have a research and development agreement with ChromaDex and Elysium Health.
Source: Vilhelm Bohr – University of Copenhagen
Publisher: Organized by NeuroscienceNews.com.
Image Source: NeuroscienceNews.com image is in the public domain.
Original Research: Abstract for “Mitophagy inhibits amyloid-β and tau pathology and reverses cognitive deficits in models of Alzheimer’s disease” by Evandro F. Fang, Yujun Hou, Konstantinos Palikaras, Bryan A. Adriaanse, Jesse S. Kerr, Beimeng Yang, Sofie Lautrup, Md Mahdi Hasan-Olive, Domenica Caponio, Xiuli Dan, Paula Rocktäschel, Deborah L. Croteau, Mansour Akbari, Nigel H. Greig, Tormod Fladby, Hilde Nilsen, M. Zameel Cader, Mark P. Mattson, Nektarios Tavernarakis & Vilhelm A. Bohr in Nature Neuroscience. Published February 11 2019.
doi:10.1038/s41593-018-0332-9
[cbtabs][cbtab title=”MLA”]University of Copenhagen”‘Lack of Cleaning’ in Brain Cells is Central to Alzheimer’s.” NeuroscienceNews. NeuroscienceNews, 15 February 2019.
<https://neurosciencenews.com/mitochondria-alzheimers-10744/>.[/cbtab][cbtab title=”APA”]University of Copenhagen(2019, February 15). ‘Lack of Cleaning’ in Brain Cells is Central to Alzheimer’s. NeuroscienceNews. Retrieved February 15, 2019 from https://neurosciencenews.com/mitochondria-alzheimers-10744/[/cbtab][cbtab title=”Chicago”]University of Copenhagen”‘Lack of Cleaning’ in Brain Cells is Central to Alzheimer’s.” https://neurosciencenews.com/mitochondria-alzheimers-10744/ (accessed February 15, 2019).[/cbtab][/cbtabs]
Abstract
Mitophagy inhibits amyloid-β and tau pathology and reverses cognitive deficits in models of Alzheimer’s disease
Accumulation of damaged mitochondria is a hallmark of aging and age-related neurodegeneration, including Alzheimer’s disease (AD). The molecular mechanisms of impaired mitochondrial homeostasis in AD are being investigated. Here we provide evidence that mitophagy is impaired in the hippocampus of AD patients, in induced pluripotent stem cell-derived human AD neurons, and in animal AD models. In both amyloid-β (Aβ) and tau Caenorhabditis elegans models of AD, mitophagy stimulation (through NAD+ supplementation, urolithin A, and actinonin) reverses memory impairment through PINK-1 (PTEN-induced kinase-1)-, PDR-1 (Parkinson’s disease-related-1; parkin)-, or DCT-1 (DAF-16/FOXO-controlled germline-tumor affecting-1)-dependent pathways. Mitophagy diminishes insoluble Aβ1–42 and Aβ1–40 and prevents cognitive impairment in an APP/PS1 mouse model through microglial phagocytosis of extracellular Aβ plaques and suppression of neuroinflammation. Mitophagy enhancement abolishes AD-related tau hyperphosphorylation in human neuronal cells and reverses memory impairment in transgenic tau nematodes and mice. Our findings suggest that impaired removal of defective mitochondria is a pivotal event in AD pathogenesis and that mitophagy represents a potential therapeutic intervention.







