Summary: Combining carboplatin, a common chemotherapy drug, with everolimus, a drug that blocks mTOR, is effective at inducing apoptosis and slowing tumor growth in patients with pediatric low-grade glioma brain cancer.
Source: Johns Hopkins Medicine
A new combination treatment aimed at resistant and recurrent low-grade gliomas slowed tumor growth and killed tumor cells in laboratory and mouse models.
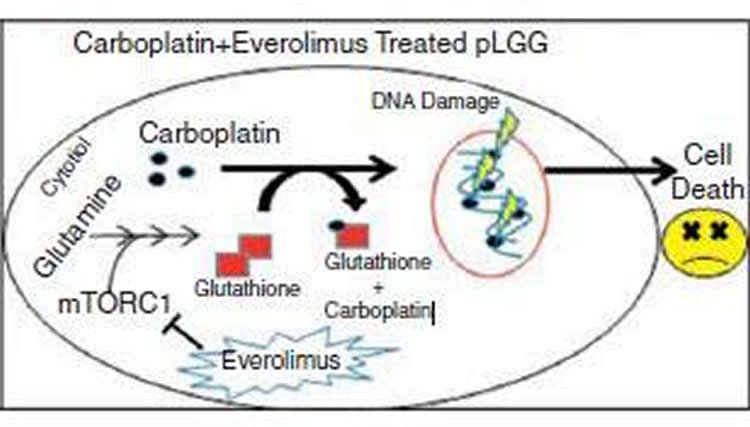
Researchers at the Johns Hopkins Kimmel Cancer Center and the Johns Hopkins University School of Medicine combined carboplatin, a standard chemotherapy drug that works well against these brain tumors, and everolimus, which blocks an enzyme called mTOR that was shown in earlier research to fuel the growth of these tumors. The combination increased DNA damage and cell death in laboratory models. Their findings were published in the Feb. 14, 2019, issue of Neuro-Oncology.
Pediatric low-grade glioma is the most common brain tumor in children and can often be treated with surgery alone. However, some patients have tumors in locations that make surgery too risky, such as near optic nerves or in the mid-brain area, or have their tumors grow back after surgery.
Eric Raabe, M.D., Ph.D., associate professor of oncology and pediatric brain tumor expert at the Johns Hopkins Kimmel Cancer Center, says tumors recur in about 50 percent of patients treated for low-grade glioma and require additional treatment with chemotherapy. Recurring tumors are often resistant to chemotherapy. The researchers wondered whether combining carboplatin and everolimus would be more effective.
When treated with carboplatin alone, four different human cell lines of low-grade glioma cancer cells did not respond to the drug or kept growing. Similarly, some cell lines were resistant to everolimus alone.
When they treated the same cell lines with a combination of carboplatin and everolimus, the cells died or grew slower, and the researchers saw similar results in mouse models with no added toxicity.
“We saw dramatic growth inhibition after only a low concentration of everolimus was combined with the carboplatin,” says Raabe. “We found that everolimus disrupted a key mechanism the cancer cells use to detoxify carboplatin. The ability of everolimus to increase the power of carboplatin suggests this combination could be used effectively in patients.”
In a previous clinical study in 2014, Raabe and other researchers were able to confirm the safety of the mTOR-blocking drug everolimus in patients with pediatric low-grade glioma and found some patients responded to the medicine. However, they never tested tumor tissue from those patients to understand the molecular role of mTOR.
“The current nationwide clinical study of everolimus in pediatric low-grade glioma requires that some tumor tissue from each patient be evaluated for expression of mTOR markers that might predict response to everolimus,” Raabe says. “In this way, we hope to figure out who is most likely to respond to the drug, so that we can move closer to our goal of giving the right medicine to the right patient at the right time. In the future, we may be able to give everolimus along with carboplatin to patients with high-level mTOR expression. Based on our research, we predict that these tumors will likely be resistant to carboplatin unless we simultaneously block mTOR.”
In addition to Raabe, other researchers in the study include Brad Poore, Ming Yuan, Antje Arnold, Antoinette Price, Jesse Alt, Jeffrey A. Rubens, Barbara S. Slusher, and Charles G. Eberhart.
Funding: This work was supported by Johns Hopkins Institute of Clinical and Translational Sciences, the Sidney Kimmel Comprehensive Cancer Center, Giant Food Pediatric Cancer Research Fund, Imagine an Answer to Kids’ Brain Cancer foundation, and A Kids’ Brain Tumor Cure foundation.
There were no conflicts of interest in connection with this study.
Source:
Johns Hopkins Medicine
Media Contacts:
Larry Frum – Johns Hopkins Medicine
Image Source:
The image is credited to Johns Hopkins Kimmel Cancer Center.
Original Research: Closed access
Brad Poore, Ming Yuan, Antje Arnold, Antoinette Price, Jesse Alt, Jeffrey A Rubens, Barbara S Slusher, Charles G Eberhart, Eric H Raabe, “Inhibition of mTORC1 in pediatric low-grade glioma depletes glutathione and therapeutically synergizes with carboplatin”, Neuro-Oncology, Volume 21, Issue 2, February 2019, Pages 252–263, doi:10.1093/neuonc/noy150
Abstract
Inhibition of mTORC1 in pediatric low-grade glioma depletes glutathione and therapeutically synergizes with carboplatin
Background
Pediatric low-grade glioma (pLGG) often initially responds to front-line therapies such as carboplatin, but more than 50% of treated tumors eventually progress and require additional therapy. With the discovery that pLGG often contains mammalian target of rapamycin (mTOR) activation, new treatment modalities and combinations are now possible for patients. The purpose of this study was to determine if carboplatin is synergistic with the mTOR complex 1 inhibitor everolimus in pLGG.
Methods
We treated 4 pLGG cell lines and 1 patient-derived xenograft line representing various pLGG genotypes, including neurofibromatosis type 1 loss, proto-oncogene B-Raf (BRAF)-KIAA1549 fusion, and BRAFV600E mutation, with carboplatin and/or everolimus and performed assays for growth, cell proliferation, and cell death. Immunohistochemistry as well as in vivo and in vitro metabolomics studies were also performed.
Results
Carboplatin synergized with everolimus in all of our 4 pLGG cell lines (combination index <1 at Fa 0.5). Combination therapy was superior at inhibiting tumor growth in vivo. Combination treatment increased levels of apoptosis as well as gamma-H2AX phosphorylation compared with either agent alone. Everolimus treatment suppressed the conversion of glutamine and glutamate into glutathione both in vitro and in vivo. Exogenous glutathione reversed the effects of carboplatin and everolimus.
Conclusions
The combination of carboplatin and everolimus was effective at inducing cell death and slowing tumor growth in pLGG models. Everolimus decreased the amount of available glutathione inside the cell, preventing the detoxification of carboplatin and inducing increased DNA damage and apoptosis.






