Summary: A study recently presented at the International Meeting for Autism Research suggests gastrointestinal problems commonly seen in children with ASD may be a result of stress, and not diet, as previously assumed.
Source: University of Missouri Columbia.
Stress, not nutrition, likely cause of increased GI issues.
Many children with autism spectrum disorder experience significant gastrointestinal issues, but the cause of these symptoms is unknown. Professionals in the medical community have suggested a potential link between diet and gastrointestinal issues related to autism. Now, researchers from the University of Missouri School of Medicine have found that diet is not a contributing factor in these individuals. The researchers hope the findings could help lead to improved treatment options.
“Unfortunately, it’s not uncommon for those with autism to experience constipation, irritable bowel syndrome, abdominal pain and other gastrointestinal issues,” said Brad Ferguson, Ph.D., postdoctoral research fellow in the Department of Radiology at the MU School of Medicine and the MU Thompson Center for Autism and Neurodevelopmental Disorders. “We sought to find out whether nutritional intake in their individual diets was associated with gastrointestinal issues. Based on our findings, dietary intake does not appear to be the culprit for these issues, and other factors are likely at play.”
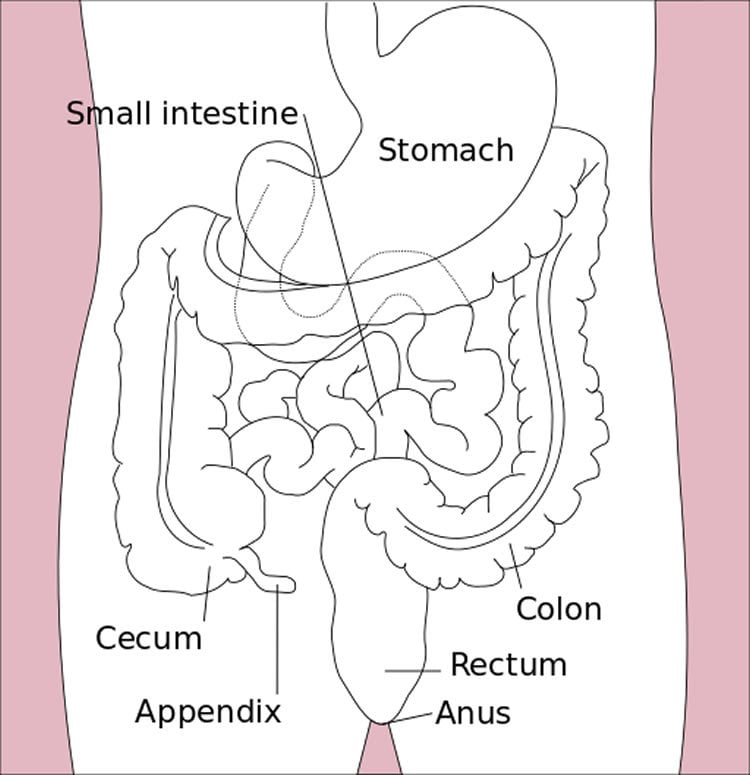
A previous study conducted by the research team identified a relationship between increased cortisol response to stress and gastrointestinal symptoms in people with autism spectrum disorder. Cortisol is a hormone released by the body in times of stress, and one of its functions is to prevent the release of substances in the body that cause inflammation. In this study, the researchers sought to confirm or rule out dietary intake as a source of gastrointestinal problems.
The team studied 75 individuals between the ages of 5 and 18 who are part of the Autism Speaks Autism Treatment Network who were treated at the MU Thompson Center for Autism and Neurodevelopmental Disorders. The individuals’ caregivers completed a questionnaire to assess the children’s gastrointestinal symptoms, as well as a questionnaire on food intake over the past month. The individuals also underwent two stress tests to measure cortisol levels.
“We looked at the reported instances of gastrointestinal issues and compared them with 32 different nutrients found in a standard diet,” Ferguson said. “Contrary to what you may initially think, dietary composition does not appear to be a driving factor between stress response and gastrointestinal function in this sample. More research is needed to better understand the causes of these issues, but an increased reaction to stress does appear to be a contributing factor.”
In addition to Ferguson, the research team includes principal investigator David Beversdorf and Micah Mazurek with the MU Thompson Center for Autism and Neurodevelopmental Disorders; Danielle Severns with the MU School of Medicine; Sarah Marler and Ethan Lee with Vanderbilt University; Margaret Bauman with Boston University; and Kara Margolis and Jeremy Veenstra-VanderWeele with Columbia University.
Funding: Research reported in this study was supported by the Autism Speaks Autism Treatment Network/Autism Intervention Research Network on Physical Health, the Health Resources and Services Administration of the U.S. Department of Health and Human Services, and an MU School of Medicine Summer Research Fellowship. The researchers have no conflicts of interest to declare related to this study. The content is solely the responsibility of the authors and does not necessarily represent the official views of the funding agencies.
Source: Derek Thompson – University of Missouri Columbia
Image Source: NeuroscienceNews.com image is in the public domain.
Original Research: The study, “Associations between Dietary Composition and Gastrointestinal Symptoms in Autism Spectrum Disorder,” recently was presented at the 2017 International Meeting for Autism Research.
[cbtabs][cbtab title=”MLA”]University of Missouri Columbia “Diet Not Connected to GI Problems in Autistic Children.” NeuroscienceNews. NeuroscienceNews, 12 July 2017.
<https://neurosciencenews.com/gi-diet-autism-7070/>.[/cbtab][cbtab title=”APA”]University of Missouri Columbia (2017, July 12). Diet Not Connected to GI Problems in Autistic Children. NeuroscienceNew. Retrieved July 12, 2017 from https://neurosciencenews.com/gi-diet-autism-7070/[/cbtab][cbtab title=”Chicago”]University of Missouri Columbia “Diet Not Connected to GI Problems in Autistic Children.” https://neurosciencenews.com/gi-diet-autism-7070/ (accessed July 12, 2017).[/cbtab][/cbtabs]
Abstract
Meta-analysis of time perception and temporal processing in schizophrenia: Differential effects on precision and accuracy
Numerous studies have reported that time perception and temporal processing are impaired in schizophrenia. In a meta-analytical review, we differentiate between time perception (judgments of time intervals) and basic temporal processing (e.g., judgments of temporal order) as well as between effects on accuracy (deviation of estimates from the veridical value) and precision (variability of judgments). In a meta-regression approach, we also included the specific tasks and the different time interval ranges as covariates. We considered 68 publications of the past 65 years, and meta-analyzed data from 957 patients with schizophrenia and 1060 healthy control participants. Independent of tasks and interval durations, our results demonstrate that time perception and basic temporal processing are less precise (more variable) in patients (Hedges’ g > 1.00), whereas effects of schizophrenia on accuracy of time perception are rather small and task-dependent. Our review also shows that several aspects, e.g., potential influences of medication, have not yet been investigated in sufficient detail. In conclusion, the results are in accordance with theoretical assumptions and the notion of a more variable internal clock in patients with schizophrenia, but not with a strong effect of schizophrenia on clock speed. The impairment of temporal precision, however, may also be clock-unspecific as part of a general cognitive deficiency in schizophrenia.
“Meta-analysis of time perception and temporal processing in schizophrenia: Differential effects on precision and accuracy” by Sven Thoenesa and Daniel Oberfelda in Clinical Psychology Review. Published online March 29 2017 doi:10.1016/j.cpr.2017.03.007