Summary: A new study reports babies born prematurely show better brain development when fed breast milk rather than formula.
Source: University of Edinburgh.
Babies born before their due date show better brain development when fed breast milk rather than formula, a study has found.
Experts say that helping mothers to provide breast milk in the weeks after giving birth could improve long-term outcomes for children born pre-term.
Premature birth has been linked to an increased possibility of problems with learning and thinking skills in later life, which are thought to be linked to alterations in brain development.
Studies have shown that pre-term birth is associated with changes in the part of the brain’s structure that helps brain cells to communicate with one another, known as white matter.
Researchers at the University of Edinburgh studied MRI brain scans from 47 babies from a study group known as the Theirworld Edinburgh Birth Cohort.
The babies had been born before 33 weeks gestation and scans took place when they reached term-equivalent age, an average of 40 weeks from conception.
The team also collected information about how the infants had been fed while in intensive care – either formula milk or breast milk from either the mother or a donor.
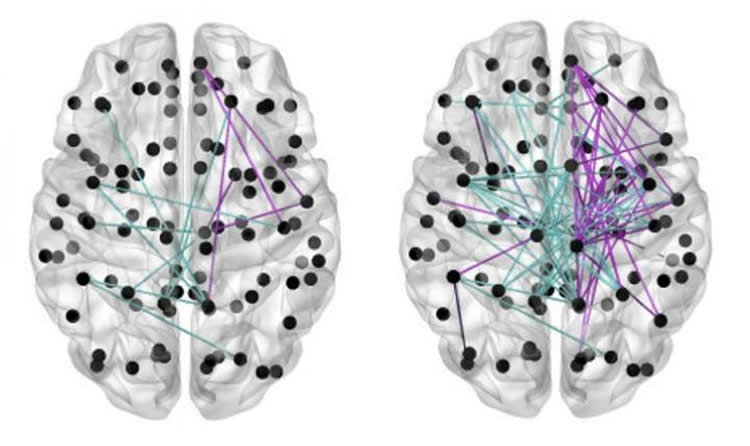
Babies who exclusively received breast milk for at least three-quarters of the days they spent in hospital showed improved brain connectivity compared with others.
The effects were greatest in babies who were fed breast milk for a greater proportion of their time spent in intensive care.
The study was funded by the charity Theirworld and was carried out in the Jennifer Brown Research Laboratory at the University’s Medical Research Council Centre for Reproductive Health. It is published in the journal NeuroImage.
Professor James Boardman, Director of the Jennifer Brown Research Laboratory at the University of Edinburgh, said: “Our findings suggest that brain development in the weeks after preterm birth is improved in babies who receive greater amounts of breast milk.
“This study highlights the need for more research to understand the role of early life nutrition for improving long-term outcomes for pre-term babies.
“Mothers of pre-term babies should be supported to provide breast milk while their baby is in neonatal care – if they are able to and if their baby is well enough to receive milk – because this may give their children the best chance of healthy brain development.”
Sarah Brown, President and Trustee of Theirworld, said: “I am so proud of the achievements of the Jennifer Brown Research Laboratory. This latest report delivers valuable evidence to support breast milk feeding for even the tiniest, most vulnerable premature babies, to give them the best start in life.
“An immense debt of gratitude is due to the families of the Theirworld Edinburgh Birth Cohort, who are dedicated to sharing information to support their own little ones, and benefit many other premature babies in the future.”
Source: Jen Middleton – University of Edinburgh
Publisher: Organized by NeuroscienceNews.com.
Image Source: NeuroscienceNews.com image is credited to Jennifer Brown Research Laboratory, the University of Edinburgh.
Original Research: Open access research for “Early breast milk exposure modifies brain connectivity in preterm infants” by Manuel Blesa, Gemma Sullivan, Devasuda Anblagan, Emma J. Telford, Alan J.Quigley, Sarah A. Sparrow, Ahmed Serag, Scott I. Semple, Mark E. Bastin, and James P. Boardman in NeuroImage. Published September 18 2018.
doi:10.1016/j.neuroimage.2018.09.045
[cbtabs][cbtab title=”MLA”]University of Edinburgh”Breast Milk May Be Best For Premature Babies’ Brain Development.” NeuroscienceNews. NeuroscienceNews, 21 September 2018.
<https://neurosciencenews.com/breast-milk-brain-development-9896/>.[/cbtab][cbtab title=”APA”]University of Edinburgh(2018, September 21). Breast Milk May Be Best For Premature Babies’ Brain Development. NeuroscienceNews. Retrieved September 21, 2018 from https://neurosciencenews.com/breast-milk-brain-development-9896/[/cbtab][cbtab title=”Chicago”]University of Edinburgh”Breast Milk May Be Best For Premature Babies’ Brain Development.” https://neurosciencenews.com/breast-milk-brain-development-9896/ (accessed September 21, 2018).[/cbtab][/cbtabs]
Abstract
Early breast milk exposure modifies brain connectivity in preterm infants
Preterm infants are at increased risk of alterations in brain structure and connectivity, and subsequent neurocognitive impairment. Breast milk may be more advantageous than formula feed for promoting brain development in infants born at term, but uncertainties remain about its effect on preterm brain development and the optimal nutritional regimen for preterm infants. We test the hypothesis that breast milk exposure is associated with improved markers of brain development and connectivity in preterm infants at term equivalent age.
We collected information about neonatal breast milk exposure and brain MRI at term equivalent age from 47 preterm infants (mean postmenstrual age [PMA] 29.43 weeks, range 23.28–33.0). Network-Based Statistics (NBS), Tract-based Spatial Statistics (TBSS) and volumetric analysis were used to investigate the effect of breast milk exposure on white matter water diffusion parameters, tissue volumes, and the structural connectome.
Twenty-seven infants received exclusive breast milk feeds for ≥75% of days of in-patient care and this was associated with higher connectivity in the fractional anisotropy (FA)-weighted connectome compared with the group who had < 75% of days receiving exclusive breast milk feeds (NBS, p = 0.04). Within the TBSS white matter skeleton, the group that received ≥75% exclusive breast milk days exhibited higher FA within the corpus callosum, cingulum cingulate gyri, centrum semiovale, corticospinal tracts, arcuate fasciculi and posterior limbs of the internal capsule compared with the low exposure group after adjustment for PMA at birth, PMA at image acquisition, bronchopulmonary dysplasia, and chorioamnionitis (p < 0.05). The effect on structural connectivity and tract water diffusion parameters was greater with ≥90% exposure, suggesting a dose effect. There were no significant groupwise differences in brain volumes.
Breast milk feeding in the weeks after preterm birth is associated with improved structural connectivity of developing networks and greater FA in major white matter fasciculi.






