Using a sophisticated MRI technique, researchers have found abnormalities in the brain’s white matter tracts in patients with insomnia. Results of the study were published online in the journal Radiology.
Primary insomnia, in which individuals have difficulty falling or staying asleep for a month or longer, is associated with daytime fatigue, mood disruption and cognitive impairment. Insomnia can also lead to depression and anxiety disorders.
“Insomnia is a remarkably prevalent disorder,” said researcher Shumei Li, M.S., from the Department of Medical Imaging, Guangdong No. 2 Provincial People’s Hospital, Guangzhou, China. “However, its causes and consequences remain elusive.”
For the study, Li, along with colleagues lead by investigator Guihua Jiang, M.D., set out to analyze the white matter tracts in insomnia patients and the relationship between abnormal white matter integrity and the duration and features of insomnia.
“White matter tracts are bundles of axons–or long fibers of nerve cells–that connect one part of the brain to another,” Li said. “If white matter tracts are impaired, communication between brain regions is disrupted.”
The study included 23 patients with primary insomnia and 30 healthy control volunteers. To evaluate mental status and sleep patterns, all participants completed questionnaires including the Pittsburgh Sleep Quality Index, the Insomnia Severity Index, the Self-Rating Anxiety Scale and the Self-Rating Depression Scale.
Each participant also underwent brain MRI with a specialized technique called diffusion tensor imaging (DTI). DTI allows researchers to analyze the pattern of water movement along white matter tracts to identify a loss of tract integrity.
“We used a new method called Tract-Based Spatial Statistics that is highly sensitive to the microstructure of the white matter tract and provides multiple diffusion measures,” Li said.
Results of the analysis showed that compared to the healthy controls, the insomnia patients had significantly reduced white matter integrity in several right-brain regions, and the thalamus which regulates consciousness, sleep and alertness.
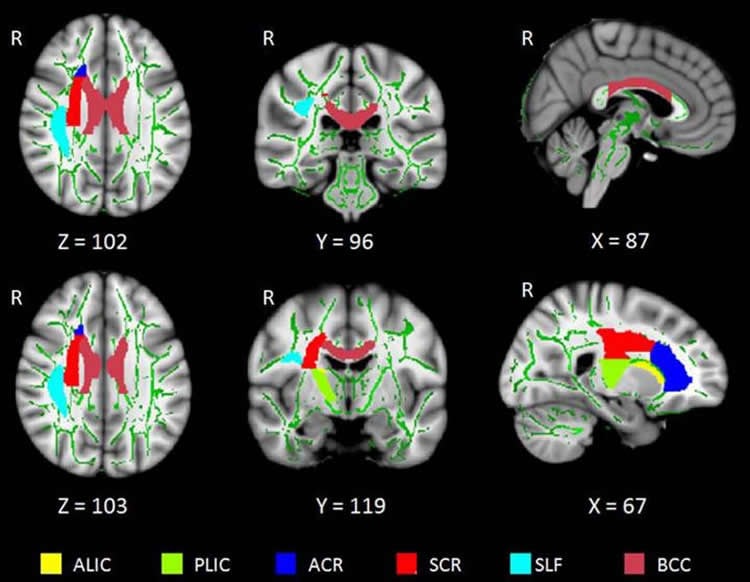
“These impaired white matter tracts are mainly involved in the regulation of sleep and wakefulness, cognitive function and sensorimotor function,” Li said.
In addition, abnormalities in the thalamus and body corpus callosum–the largest white matter structure in the brain–were associated with the duration of patients’ insomnia and score on self-rating depression scale.
“The involvement of the thalamus in the pathology of insomnia is particularly critical, since the thalamus houses important constituents of the body’s biological clock,” she added.
The study also found that underlying cause of white matter integrity abnormalities in insomnia patients may be loss of myelin, the protective coating around nerve fibers.
The researchers caution that further study needs to be done on a larger sample to clarify the relationship between altered white matter integrity and insomnia.
Source: Linda Brooks – Radiological Society of North America
Image Credit: The image is credited to Radiological Society of North America.
Original Research: Abstract for “Reduced Integrity of Right Lateralized White Matter in Patients with Primary Insomnia: A Diffusion-Tensor Imaging Study” by Shumei Li, Junzhang Tian, Andreas Bauer, Ruiwang Huang, Hua Wen, Meng Li, Tianyue Wang, Likun Xia, and Guihua Jiang in Radiology. Published online April 5 2016 doi:10.1148/radiol.2016152038
Abstract
Reduced Integrity of Right Lateralized White Matter in Patients with Primary Insomnia: A Diffusion-Tensor Imaging Study
Purpose
To analyze the integrity of white matter (WM) tracts in primary insomnia patients and provide better characterization of abnormal WM integrity and its relationship with disease duration and clinical features of primary insomnia.
Materials and Methods
This prospective study was approved by the ethics committee of the Guangdong No. 2 Provincial People’s Hospital. Tract-based spatial statistics were used to compare changes in diffusion parameters of WM tracts from 23 primary insomnia patients and 30 healthy control (HC) participants, and the accuracy of these changes in distinguishing insomnia patients from HC participants was evaluated. Voxel-wise statistics across subjects was performed by using a 5000-permutation set with family-wise error correction (family-wise error, P < .05). Multiple regressions were used to analyze the associations between the abnormal fractional anisotropy (FA) in WM with disease duration, Pittsburgh Sleep Quality Index, insomnia severity index, self-rating anxiety scale, and the self-rating depression scale in primary insomnia. Characteristics for abnormal WM were also investigated in tract-level analyses.
Results
Primary insomnia patients had lower FA values mainly in the right anterior limb of the internal capsule, right posterior limb of the internal capsule, right anterior corona radiata, right superior corona radiata, right superior longitudinal fasciculus, body of the corpus callosum, and right thalamus (P < .05, family-wise error correction). The receiver operating characteristic areas for the seven regions were acceptable (range, 0.60–0.74; 60%–74%). Multiple regression models showed abnormal FA values in the thalamus and body corpus callosum were associated with the disease duration, self-rating depression scale, and Pittsburgh Sleep Quality Index scores. Tract-level analysis suggested that the reduced FA values might be related to greater radial diffusivity.
Conclusion
This study showed that WM tracts related to regulation of sleep and wakefulness, and limbic cognitive and sensorimotor regions, are disrupted in the right brain in patients with primary insomnia. The reduced integrity of these WM tracts may be because of loss of myelination.
“Reduced Integrity of Right Lateralized White Matter in Patients with Primary Insomnia: A Diffusion-Tensor Imaging Study” by Shumei Li, Junzhang Tian, Andreas Bauer, Ruiwang Huang, Hua Wen, Meng Li, Tianyue Wang, Likun Xia, and Guihua Jiang in Radiology. Published online April 5 2016 doi:10.1148/radiol.2016152038