Summary: Researchers report vitamin D levels affect perineuronal nets in the hippocampus. The study found vitamin D deficiency resulted in a significant decline in memory and learning in mouse models.
Source: University of Queensland.
University of Queensland research may explain why vitamin D is vital for brain health, and how deficiency leads to disorders including depression and schizophrenia.
Associate Professor Thomas Burne at UQ’s Queensland Brain Institute led the studies, which provide the groundwork for research into better prevention and treatments.
“Over a billion people worldwide are affected by vitamin D deficiency, and there is a well-established link between vitamin D deficiency and impaired cognition,” Dr Burne said.
“Unfortunately, exactly how vitamin D influences brain structure and function is not well understood, so it has remained unclear why deficiency causes problems.”
Dr Burne’s team found that vitamin D levels affect a type of ‘scaffolding’ in the brain, called perineuronal nets.
“These nets form a strong, supportive mesh around certain neurons, and in doing so they stabilise the contacts these cells make with other neurons,” he said.
Researchers removed vitamin D from the diet of a group of healthy adult mice, and after 20 weeks found a significant decline in their ability to remember and learn compared to a control group.
Dr Burne said the vitamin D deficient group had a pronounced reduction in perineuronal nets in the hippocampus, the brain region crucial to memory formation.
“There was also a stark reduction in both the number and strength of connections between neurons in that region.”
Dr Burne’s team propose that vitamin D plays an important role in keeping perineuronal nets stable, and that when vitamin D levels drop, this ‘scaffolding’ is more easily degraded by enzymes.
“As neurons in the hippocampus lose their supportive perineuronal nets, they have trouble maintaining connections, and this ultimately leads to a loss of cognitive function.”
Associate Professor Burne said the hippocampus may be most strongly affected by vitamin D deficiency because it is much more active than other brain regions.
“It’s like the canary in the coalmine–it might fail first because its high energy requirement makes it more sensitive to the depletion of essential nutrients like vitamin D.
“Intriguingly, the right side of the hippocampus was more affected by vitamin D deficiency than the left side.”
Associate Professor Burne said loss of function in this area could be an important contributor to the hallmarks of schizophrenia, including severe memory deficits and a distorted perception of reality.
“The next step is to test this new hypothesis on the link between vitamin D deficiency, perineuronal nets and cognition,” he said.
“We are also particularly excited to have discovered these nets can change in adult mice.
“I’m hoping that because they’re dynamic there is a chance that we can rebuild them, and that could set the stage for new treatments.”
Source: Thomas Burne – University of Queensland
Publisher: Organized by NeuroscienceNews.com.
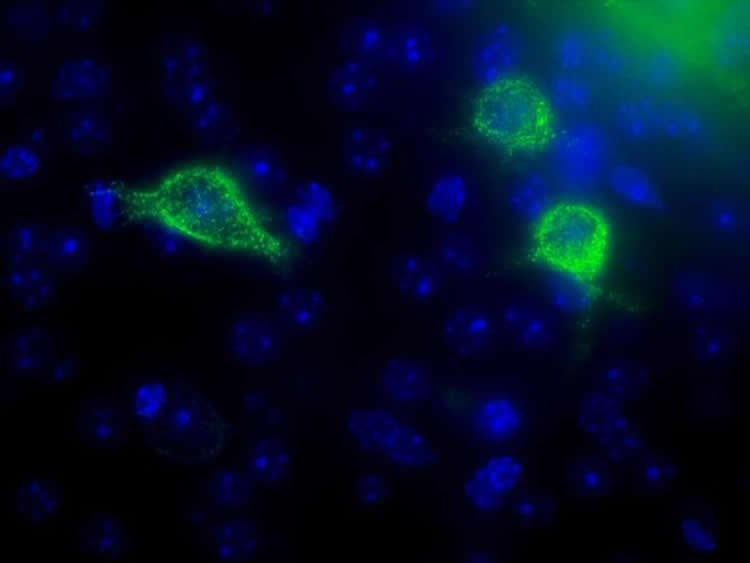
Image Source: NeuroscienceNews.com image is credited to Phoebe Mayne, The University of Queensland.
Original Research: Abstract for “Vitamin D in Synaptic Plasticity, Cognitive Function, and Neuropsychiatric Illness” by Phoebe E. Mayne, and Thomas H.J. Burne in Trends in Neurosciences. Published February 18 2019.
doi:10.1016/j.tins.2019.01.003
[cbtabs][cbtab title=”MLA”]University of Queensland”Potential Link Between Vitamin D Deficiency and Loss of Brain Plasticity.” NeuroscienceNews. NeuroscienceNews, 19 February 2019.
<https://neurosciencenews.com/vitamin-d-brain-plasticity-10777/>.[/cbtab][cbtab title=”APA”]University of Queensland(2019, February 19). Potential Link Between Vitamin D Deficiency and Loss of Brain Plasticity. NeuroscienceNews. Retrieved February 19, 2019 from https://neurosciencenews.com/vitamin-d-brain-plasticity-10777/[/cbtab][cbtab title=”Chicago”]University of Queensland”Potential Link Between Vitamin D Deficiency and Loss of Brain Plasticity.” https://neurosciencenews.com/vitamin-d-brain-plasticity-10777/ (accessed February 19, 2019).[/cbtab][/cbtabs]
Abstract
Vitamin D in Synaptic Plasticity, Cognitive Function, and Neuropsychiatric Illness
Vitamin D plays various roles in normal brain physiology, including modulating synaptic plasticity.
Converging evidence suggests that vitamin D deficiency affects multiple brain processes, including cognitive functioning, in both healthy people and those afflicted with neuropsychiatric illness. The underlying mechanisms, however, are poorly understood.
Evidence suggests that vitamin D deficiency impacts synaptic plasticity through a plethora of avenues, including l-type voltage-gated calcium channels and regulation of various neurotransmitters, including NO.
An emerging concept is that vitamin D deficiency may weaken the integrity of PNNs, aggregates of the ECM, through modulation of MMPs.
PNNs have been reported to play essential roles in cognitive processes such as learning and memory. As such, dysregulation of PNNs is likely to disturb neural-circuit function and impair cognitive functioning.
Assessing the molecular mechanisms that underpin the roles of vitamin D in cognition is pertinent to informing preventive and intervention strategies for persons with cognitive disturbances, including patients with schizophrenia.
Over a billion people worldwide are affected by vitamin D deficiency. Although vitamin D deficiency is associated with impaired cognition, the mechanisms mediating this link are poorly understood. The extracellular matrix (ECM) has now emerged as an important participant of synaptic plasticity and a new hypothesis is that vitamin D may interact with aggregates of the ECM, perineuronal nets (PNNs), to regulate brain plasticity. Dysregulation of PNNs caused by vitamin D deficiency may contribute to the presentation of cognitive deficits. Understanding the molecular mechanisms underpinning the role of vitamin D in brain plasticity and cognition could help identify ways to treat cognitive symptoms in schizophrenia and other neuropsychiatric conditions.







