Summary: Researchers find significant differences in the brains of teens with bipolar disorder that attempt to take their lives over those with the disorder who have never attempted suicide.
Source: Yale.
A new Yale-led study of adolescents and young adults at high risk of taking their own lives — those suffering from bipolar disorder — implicates specific differences in the brains of those who attempt suicide and those who do not, researchers report Jan. 31 in the American Journal of Psychiatry.
“Suicide is a leading cause of death of adolescents and young adults, and we can’t move on this issue fast enough,” said Hilary Blumberg, the John and Hope Furth Professor of Psychiatric Neuroscience, professor in psychiatry, radiology, and biomedical imaging and in the Yale Child Study Center, and senior author of the study. “The identification of brain circuits involved in risk for suicide can lead to new ways to identify who is most at risk and hopefully, prevent suicides.”
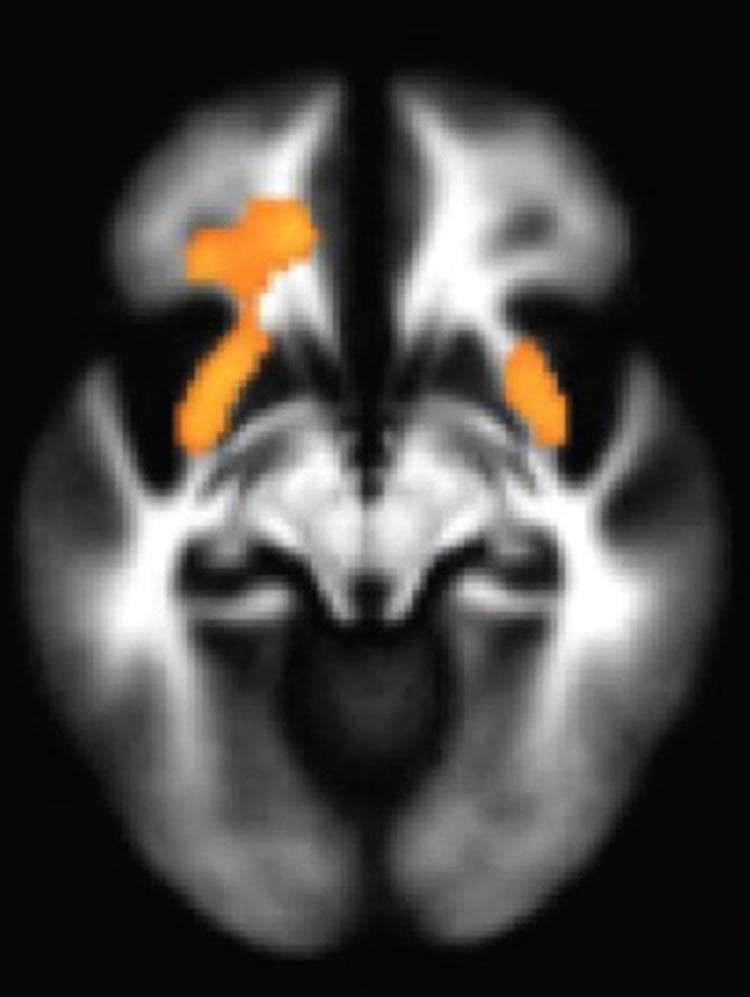
About half of individuals with bipolar disorder, which is marked by extreme mood swings, attempt suicide in their lifetimes, and as many as one in five people with the disorder may die by suicide. In studies of adults who made suicide attempts, evidence implicates problems in the frontal-limbic system, where emotions and impulses arise, and the frontal cortex, which helps regulate emotions and impulses.
Blumberg and her colleagues studied adolescents and young adults. Since their frontal-limbic system is still under development, explain the researchers, studying them could provide windows onto how suicidal thoughts and behaviors arise. Blumberg and her team took specialized magnetic resonance imaging (MRI) scans of those who had attempted suicide and those who had not and found several telltale differences. Those who had attempted suicide had subtle decreases in the volume and activity in areas of the brain ciruitry that regulate emotion and impulses, and in the white matter, the wiring that provides connections between those brain areas.
“The findings suggest that the frontal cortex is not working as well as it should to regulate the circuitry,” Blumberg said. “That can lead to more extreme emotional pain, difficulties in generating alternate solutions to suicide and greater likelihood of acting on suicidal impulses.”
Blumberg said further research into brain circuitry developmental processes that lead to suicide can help identify individuals at risk of suicide. The findings may help clinicians develop new strategies to minimize risk factors and therapies designed to strengthen the vulnerable brain circuits.
Jennifer A.Y. Johnston is the lead author of the study.
Funding: Funding for the research came from the National Institutes of Health, American Foundation for Suicide Prevention, International Bipolar Disorder Foundation, Brain and Behavior Research Foundation, Women’s Health Research at Yale, and The John and Hope Furth Endowment.
Source: Bill Hathaway – Yale
Image Source: NeuroscienceNews.com image is adapted from the Yale press release.
Original Research: Abstract for “Multimodal Neuroimaging of Frontolimbic Structure and Function Associated With Suicide Attempts in Adolescents and Young Adults With Bipolar Disorder” by Jennifer A.Y. Johnston, M.A., Fei Wang, M.D., Ph.D., Jie Liu, Ph.D., Benjamin N. Blond, M.D., Amanda Wallace, M.D., Jiacheng Liu, M.D., Ph.D., Linda Spencer, B.S., Elizabeth T. Cox Lippard, Ph.D., Kirstin L. Purves, B.Sc., Angeli Landeros-Weisenberger, M.D., Eric Hermes, M.D., Brian Pittman, M.S., Sheng Zhang, Ph.D., Robert King, M.D., Andrés Martin, M.D., M.P.H., Maria A. Oquendo, M.D., and Hilary P. Blumberg, M.D. in American Journal of Psychiatry. Published online February 2016 doi:10.1176/appi.ajp.2016.15050652
[cbtabs][cbtab title=”MLA”]Yale “Brain Circuits May Reveal Which Young People Are Likely to Commit Suicide.” NeuroscienceNews. NeuroscienceNews, 2 February 2017.
<https://neurosciencenews.com/teen-suicide-neural-network-6043/>.[/cbtab][cbtab title=”APA”]Yale (2017, February 2). Brain Circuits May Reveal Which Young People Are Likely to Commit Suicide. NeuroscienceNew. Retrieved February 2, 2017 from https://neurosciencenews.com/teen-suicide-neural-network-6043/[/cbtab][cbtab title=”Chicago”]Yale “Brain Circuits May Reveal Which Young People Are Likely to Commit Suicide.” https://neurosciencenews.com/teen-suicide-neural-network-6043/ (accessed February 2, 2017).[/cbtab][/cbtabs]
Abstract
Multimodal Neuroimaging of Frontolimbic Structure and Function Associated With Suicide Attempts in Adolescents and Young Adults With Bipolar Disorder
Objective:
Bipolar disorder is associated with high risk for suicidal behavior that often develops in adolescence and young adulthood. Elucidation of involved neural systems is critical for prevention. This study of adolescents and young adults with bipolar disorder with and without a history of suicide attempts combines structural, diffusion tensor, and functional MR imaging methods to investigate implicated abnormalities in the morphology and structural and functional connectivity within frontolimbic systems.
Method:
The study had 26 participants with bipolar disorder who had a prior suicide attempt (the attempter group) and 42 participants with bipolar disorder without a suicide attempt (the nonattempter group). Regional gray matter volume, white matter integrity, and functional connectivity during processing of emotional stimuli were compared between groups, and differences were explored for relationships between imaging modalities and associations with suicide-related symptoms and behaviors.
Results:
Compared with the nonattempter group, the attempter group showed significant reductions in gray matter volume in the orbitofrontal cortex, hippocampus, and cerebellum; white matter integrity in the uncinate fasciculus, ventral frontal, and right cerebellum regions; and amygdala functional connectivity to the left ventral and right rostral prefrontal cortex. In exploratory analyses, among attempters, there was a significant negative correlation between right rostral prefrontal connectivity and suicidal ideation and between left ventral prefrontal connectivity and attempt lethality.
Conclusions:
Adolescent and young adult suicide attempters with bipolar disorder demonstrate less gray matter volume and decreased structural and functional connectivity in a ventral frontolimbic neural system subserving emotion regulation. Among attempters, reductions in amygdala–prefrontal functional connectivity may be associated with severity of suicidal ideation and attempt lethality.
“Multimodal Neuroimaging of Frontolimbic Structure and Function Associated With Suicide Attempts in Adolescents and Young Adults With Bipolar Disorder” by Jennifer A.Y. Johnston, M.A., Fei Wang, M.D., Ph.D., Jie Liu, Ph.D., Benjamin N. Blond, M.D., Amanda Wallace, M.D., Jiacheng Liu, M.D., Ph.D., Linda Spencer, B.S., Elizabeth T. Cox Lippard, Ph.D., Kirstin L. Purves, B.Sc., Angeli Landeros-Weisenberger, M.D., Eric Hermes, M.D., Brian Pittman, M.S., Sheng Zhang, Ph.D., Robert King, M.D., Andrés Martin, M.D., M.P.H., Maria A. Oquendo, M.D., and Hilary P. Blumberg, M.D. in American Journal of Psychiatry. Published online February 2016 doi:10.1176/appi.ajp.2016.15050652






