Summary: People with schizophrenia have lower levels of S1P, a type of fatty molecule found in white matter. Evaluating post mortem tissue of those who died from a range of psychiatric disorders, researchers found the decreased levels of S1P in the brain were only attributed to those with schizophrenia. The findings could lead to new targeted treatments for the mental health disorder.
Source: RIKEN
Researchers at the RIKEN Center for Brian Science (CBS) in Japan have discovered a deficiency in the brains of people with schizophrenia that could lead to the development of new drug therapies. A postmortem comparison published in Schizophrenia Bulletin revealed that schizophrenia was associated with lower than normal levels of S1P, a type of fatty molecule found in the white matter of the brain. Preventing S1P degradation might therefore be a new direction for drug development in treating schizophrenia.
In recent years, drug therapy for schizophrenia has come to a stand-still. Most of the drugs available for schizophrenia are based on dopamine, but they are ineffective in about one out of every three patients. “Because we don’t have another angle on what causes schizophrenia, many pharmaceutical companies are pulling out of schizophrenia-related drug development,” says Takeo Yoshikawa, team leader at RIKEN CBS. “Hopefully, our findings can provide the new angle with a new target for drug development.”
Although schizophrenia is a well-known mental disorder that affects the brain, how it does so remains somewhat of a mystery. Scientists have known for some time that the brains of people with schizophrenia have less white matter than normal brains. White matter in the brain is made from oligodendrocytes, special cells that wrap around the parts of neurons that carry outgoing signals, which helps them communicate with each other. Characteristic symptoms of schizophrenia include hallucinations and the inability to distinguish reality from fantasy, which might originate in white matter abnormalities that cause irregular communication between neurons.
Led by Takeo Yoshikawa, the team at RIKEN CBS investigated sphingolipids, a group of lipids known to have many functions, some related to white matter. Postmortem analysis of the large white matter tract that connects the left and right sides of the brain showed a severe deficiency in S1P, a sphingolipid necessary for oligodendrocyte production. Further tests showed that although normal amounts of S1P had been produced, it was metabolized and degraded when it should not have been. “Drugs that prevent S1P degradation could be particularly effective in treating schizophrenia,” says first author and postdoctoral research scientist, Kayoko Esaki.
Although the experiment sounds simple, measuring S1P levels in postmortem brains was a big challenge and required interdisciplinary expertise in chemistry–specifically mass spectrometry–that was brought to the team by Esaki. “This was the first psychiatric study of the postmortem brain to use mass spectroscopic analysis, and our discovery would not have been possible without our newly established comprehensive technique for screening sphingolipids,” says Yoshikawa.
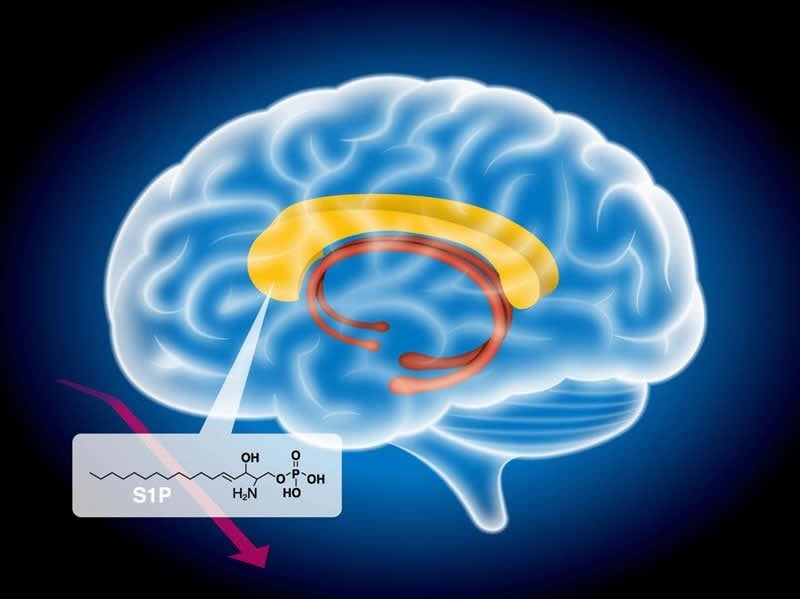
After finding S1P sphingolipid deficiency in schizophrenia, the researchers examined postmortem brains of people with bipolar disorder or major depressive disorder. They found that S1P levels did not differ from what they found in normal brains, indicating that the problem is specific for schizophrenia, and not a common feature of mental disorders.
Before schizophrenia specific clinical trials can begin, studies in animals will be necessary. “The next important step,” says Yoshikawa, “is to determine precisely which S1P receptor-acting drugs are effective in experimental animals. Although the new blockbuster drug fingolimod works at the S1P receptor and is effective at treating multiple sclerosis, we do not yet know how effective it would be for schizophrenia.”
About this neuroscience research article
Source:
RIKEN
Media Contacts:
Adam Phillips – RIKEN
Image Source:
The image is credited to RIKEN.
Original Research: Open access
“Evidence for altered metabolism of sphingosine-1-phosphate in the corpus callosum of patients with schizophrenia”. by Esaki et al..
Schizophrenia Bulletin doi:10.1093/schbul/sbaa052
Abstract
Evidence for altered metabolism of sphingosine-1-phosphate in the corpus callosum of patients with schizophrenia
The disturbed integrity of myelin and white matter, along with dysregulation of the lipid metabolism, may be involved in schizophrenia pathophysiology. Considering the crucial role of sphingolipids in neurodevelopment, particularly in oligodendrocyte differentiation and myelination, we examined the role of sphingolipid dynamics in the pathophysiology of schizophrenia. We performed targeted mass spectrometry-based analysis of sphingolipids from the cortical area and corpus callosum of postmortem brain samples from patients with schizophrenia and controls. We observed lower sphingosine-1-phosphate (S1P) levels, specifically in the corpus callosum of patients with schizophrenia, but not in major depressive disorder or bipolar disorder, when compared with the controls. Patient data and animal studies showed that antipsychotic intake did not contribute to the lowered S1P levels. We also found that lowered S1P levels in the corpus callosum of patients with schizophrenia may stem from the upregulation of genes for S1P-degrading enzymes; higher expression of genes for S1P receptors suggested a potential compensatory mechanism for the lowered S1P levels. A higher ratio of the sum of sphingosine and ceramide to S1P, which can induce apoptosis and cell-cycle arrest, was also observed in the samples of patients with schizophrenia than in controls. These results suggest that an altered S1P metabolism may underlie the deficits in oligodendrocyte differentiation and myelin formation, leading to the structural and molecular abnormalities of white matter reported in schizophrenia. Our findings may pave the way toward a novel therapeutic strategy.
Feel Free To Share This Neuroscience News.