Summary: Researchers discover higher infection rates in Purkinje cells with the herpesvirus HHV-6 in patients with bipolar disorder.
Source: University of Würzburg.
Purkinje cells are a central part of the human cerebellum, the part of the brain that plays an important role in motor learning, fine motor control of the muscle, equilibrium and posture but also influences emotions, perception, memory and language.
Scientists from the Institute for Virology and Immunobiology of the University of Würzburg and their US colleagues have now made a surprising discovery in these nerve cells. They found a high infection rate of Purkinje neurons with the human herpesvirus HHV-6 for the first time in patients with bipolar disorder and/or severe depression. The study was led by Dr. Bhupesh Prusty, group leader at the Department of Microbiology. The scientists have now published the results of their study in the journal Frontiers in Microbiology.
Virus-related inflammation in the brain
“Inherited factors have long been known to increase the risk of developing several types of psychiatric disorders including bipolar disorder, major depressive disorder and schizophrenia,” Bhupesh Prusty explains. But there is also strong evidence that environmental factors, particularly those that lead to neuroinflammation early in life, might play an important etiologic role in the pathogenesis of these disorders as well. Viruses are such an environmental factor.
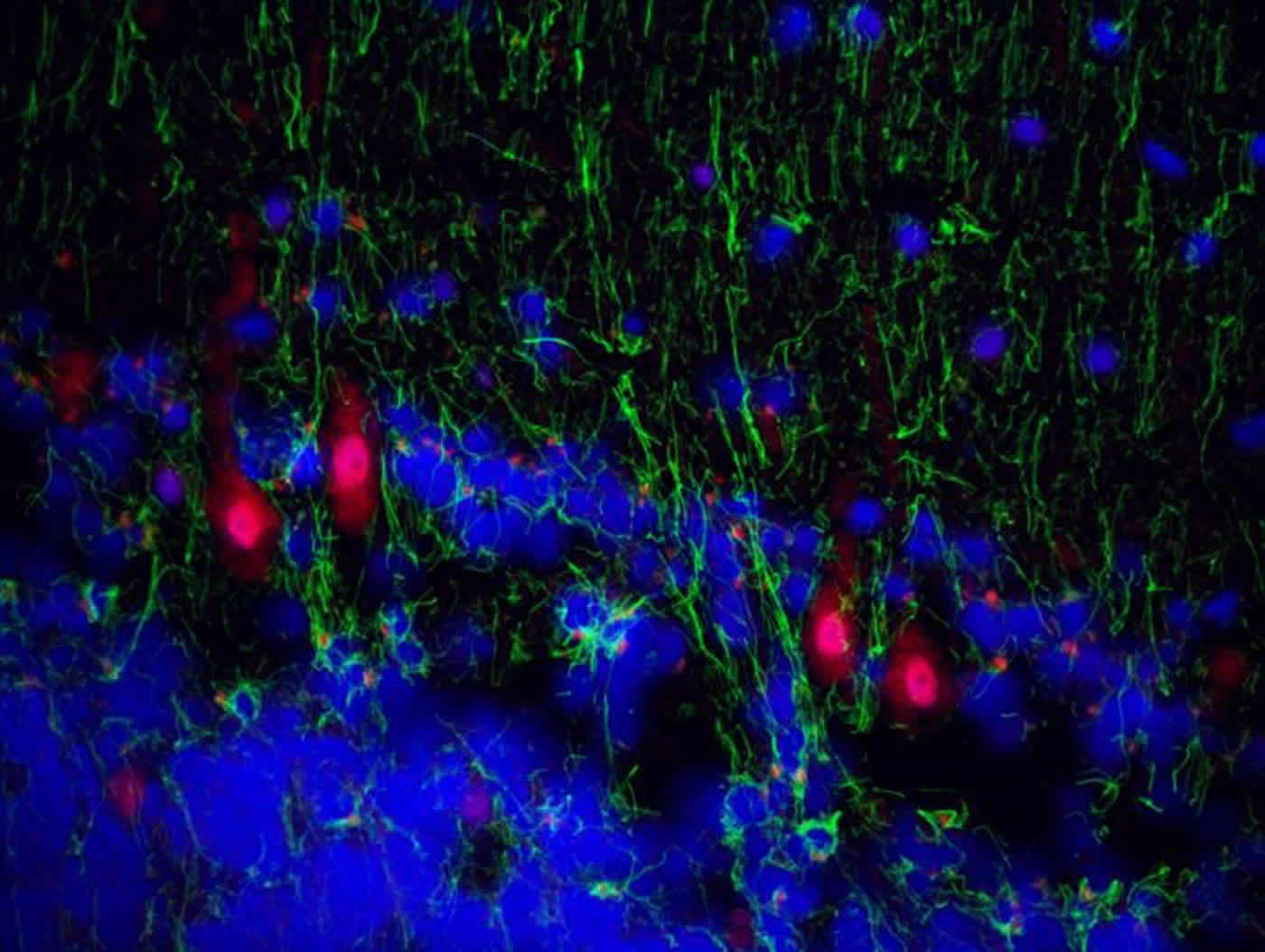
“Pathogens may disrupt neurodevelopment and cross talk with the immune system at key developmental stages,” Prusty explains. Children that are infected at a young age usually recover without any late complications. However, the viruses lie dormant (latent) in various organs and tissues including the central nervous system and the salivary glands and can be reactivated under certain circumstances, even after years.
Increased infection rate in two psychiatric disorders
Prusty and his team suspected the human herpesviruses HHV-6A and HHV-6B to play a key role in the genesis of psychiatric disorders. So they studied two of the largest human brain biopsy cohorts from Stanley Medical Research Institute (USA) and what they found confirmed their assumption: “We were able to find active infection of HHV-6 predominantly within Purkinje cells of human cerebellum in bipolar and major depressive disorder patients,” Prusty sums up the central result of their study. The results show for the first time that type HHV-6 viruses are capable of infecting neurons and possibly causing cognitive disturbances leading to mood disorder.
According to the scientists, the study disproves the belief that viruses which lie “dormant” and hidden in organs and tissues never cause any disease. “Studies like ours prove this thinking as wrong,” Prusty says and he cites another study which shows that Alzheimer’s disease can also be caused by human herpesvirus 6A.
In the next step, the Würzburg researchers want to figure out the molecular mechanisms behind HHV-6A mediated cellular damage to Purkinje neurons.
Funding: Funding provided by HHV-6 Foundation ,VolkswagenStiftung.
Source: Dr. Bhupesh Prusty – University of Würzburg
Publisher: Organized by NeuroscienceNews.com.
Image Source: NeuroscienceNews.com image is credited to Prusty et al.
Original Research: Abstract for “Active HHV-6 infection of cerebellar Purkinje cells in mood disorders” by Bhupesh K. Prusty, Nitish Gulve, Sheila Govind, Gerhard R. Krueger, Julia Feichtinger, Lee Larcombe, Richard Aspinall, DHARAM V. ABLASHI and Carla T. Toro in Frontiers in Microbiology. Published August 2 2018.
doi:10.3389/fmicb.2018.01955
[cbtabs][cbtab title=”MLA”]University of Würzburg”Surprise Finding in Neurons.” NeuroscienceNews. NeuroscienceNews, 10 August 2018.
<https://neurosciencenews.com/purkinje-cell-emotion-9682/>.[/cbtab][cbtab title=”APA”]University of Würzburg(2018, August 10). Surprise Finding in Neurons. NeuroscienceNews. Retrieved August 10, 2018 from https://neurosciencenews.com/purkinje-cell-emotion-9682/[/cbtab][cbtab title=”Chicago”]University of Würzburg”Surprise Finding in Neurons.” https://neurosciencenews.com/purkinje-cell-emotion-9682/ (accessed August 10, 2018).[/cbtab][/cbtabs]
Abstract
Active HHV-6 infection of cerebellar Purkinje cells in mood disorders
Early-life infections and associated neuroinflammation is incriminated in the pathogenesis of various mood disorders. Infection with human roseoloviruses, HHV-6A and HHV-6B, allows viral latency in the central nervous system and other tissues, which can later be activated causing cognitive and behavioral disturbances. Hence this study was designed to evaluate possible association of HHV-6A and HHV-6B activation with three different groups of psychiatric patients. DNA qPCR, immunofluorescence and FISH studies were carried out in post mortem posterior cerebellum from 50 cases each of bipolar disorder, schizophrenia, 15 major depressive disorder and 50 appropriate control samples obtained from two well-known brain collections (Stanley Medical Research Institute). HHV-6A and HHV-6B late proteins (indicating active infection) and viral DNA were detected more frequently (p < 0.001 for each virus) in human cerebellum in major depressive disorder and bipolar disorder relative to controls. These roseolovirus proteins and DNA were found less frequently in schizophrenia cases. Active HHV-6A and HHV-6B infection in cerebellar Purkinje cells were detected frequently in bipolar disorder and major depressive disorder cases. Furthermore, we found a significant association of HHV-6A infection with reduced Purkinje cell size, suggesting virus-mediated abnormal Purkinje cell function in these disorders. Finally, gene expression analysis of cerebellar tissue revealed changes in pathways reflecting an inflammatory response to HHV-6A infection. Our results provide molecular evidence to support a role for active HHV-6A and HHV-6B infection in bipolar disorder and major depressive disorder.