Summary: Researchers have identified a neurological reasons why people with eating disorders are able to override the urge to eat.
Source: University of Colorado Anschutz Medical Campus.
CU Anschutz researchers find their neuropathways travel in opposite direction.
Scientists at the University of Colorado Anschutz Medical Campus have discovered the neurological reasons why those with anorexia and bulimia nervosa are able to override the urge to eat.
In a study published last week in the journal Translational Psychiatry, the researchers showed that normal patterns of appetite stimulation in the brain are effectively reversed in those with eating disorders.
Rather than the hypothalamus, a brain region that regulates appetite, driving motivation to eat, signals from other parts of the brain can override the hypothalamus in eating disorders.
“In the clinical world we call this `mind over matter,”’ said Guido Frank, MD, lead author of the study and associate professor of psychiatry and neuroscience at the University of Colorado School of Medicine. “Now we have physiological evidence to back up that idea.”
Dr. Frank, an expert on eating disorders, set out to discover the hierarchies of the brain that govern appetite and food intake. He wanted to understand the neurological reasons behind why some people eat when they were hungry and others don’t.
Using brain scans, the researchers examined how 26 healthy women and 26 women with anorexia or bulimia nervosa reacted to tasting a sugary solution.
They discovered that those with eating disorders had widespread alterations in the structure of brain pathways governing taste-reward and appetite regulation. The alterations were found in the white matter, which coordinates communication between different parts of the brain.
There were also major differences in the role the hypothalamus played in each group.
Among those without an eating disorder, brain regions that drive eating took their cues from the hypothalamus.
In the groups with an eating disorder, the pathways to the hypothalamus were significantly weaker and the direction of information went in the opposite direction.
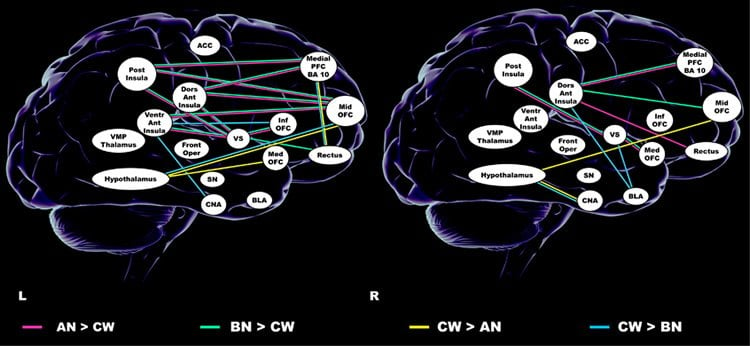
As a result, their brain may be able to override the hypothalamus and fend off the signals to eat.
“The appetite region of the brain should drive you off your chair to get something to eat,” said Frank. “But in patients with anorexia or bulimia nervosa that is not the case.” According to the study, humans are programmed at birth to like sweet tastes. But those with eating disorders begin to avoid eating sweets for fear of gaining weight.
“One could see such avoidance as a form of learned behavior and more specifically operant conditioning, with weight gain as the feared `punishment,”’ the study said. This behavior could eventually alter the brain circuits governing appetite and food intake. Researchers now suggest that being afraid to eat certain foods could impact the taste-reward processing mechanisms in the brain which could then reduce the influence of the hypothalamus.
“We now understand better on the biological level how those with an eating disorder may be able to override the drive to eat,” said Frank. “Next we need to begin looking at children to see when all of this starts to come into play.”
Frank is the author of a new book entitled “What Causes Eating Disorders – And What Do They Cause?”.
Source: David Ruth – University of Colorado Anschutz Medical Campus
Image Source: This NeuroscienceNews.com image is credited to Jeff Fitlow/University of Colorado Anschutz Medical Campus.
Original Research: Full open access research for “Altered structural and effective connectivity in anorexia and bulimia nervosa in circuits that regulate energy and reward homeostasis” by G K W Frank, M E Shott, J Riederer and T L Pryor in Translational Psychiatry. Published online November 1 2016 doi:10.1038/tp.2016.199
[cbtabs][cbtab title=”MLA”]University of Colorado Anschutz Medical Campus. “New Theory Debunks Idea That Math Abilities Are Inate.” NeuroscienceNews. NeuroscienceNews, 7 November 2016.
<https://neurosciencenews.com/neuropathways-eating-disorders-5446/>.[/cbtab][cbtab title=”APA”]University of Colorado Anschutz Medical Campus. (2016, November 7). New Theory Debunks Idea That Math Abilities Are Inate. NeuroscienceNews. Retrieved November 7, 2016 from https://neurosciencenews.com/neuropathways-eating-disorders-5446/[/cbtab][cbtab title=”Chicago”]University of Colorado Anschutz Medical Campus. “New Theory Debunks Idea That Math Abilities Are Inate.” https://neurosciencenews.com/neuropathways-eating-disorders-5446/ (accessed November 7, 2016).[/cbtab][/cbtabs]
Abstract
Altered structural and effective connectivity in anorexia and bulimia nervosa in circuits that regulate energy and reward homeostasis
Anorexia and bulimia nervosa are severe eating disorders that share many behaviors. Structural and functional brain circuits could provide biological links that those disorders have in common. We recruited 77 young adult women, 26 healthy controls, 26 women with anorexia and 25 women with bulimia nervosa. Probabilistic tractography was used to map white matter connectivity strength across taste and food intake regulating brain circuits. An independent multisample greedy equivalence search algorithm tested effective connectivity between those regions during sucrose tasting. Anorexia and bulimia nervosa had greater structural connectivity in pathways between insula, orbitofrontal cortex and ventral striatum, but lower connectivity from orbitofrontal cortex and amygdala to the hypothalamus (P<0.05, corrected for comorbidity, medication and multiple comparisons). Functionally, in controls the hypothalamus drove ventral striatal activity, but in anorexia and bulimia nervosa effective connectivity was directed from anterior cingulate via ventral striatum to the hypothalamus. Across all groups, sweetness perception was predicted by connectivity strength in pathways connecting to the middle orbitofrontal cortex. This study provides evidence that white matter structural as well as effective connectivity within the energy-homeostasis and food reward-regulating circuitry is fundamentally different in anorexia and bulimia nervosa compared with that in controls. In eating disorders, anterior cingulate cognitive–emotional top down control could affect food reward and eating drive, override hypothalamic inputs to the ventral striatum and enable prolonged food restriction.
“Altered structural and effective connectivity in anorexia and bulimia nervosa in circuits that regulate energy and reward homeostasis” by G K W Frank, M E Shott, J Riederer and T L Pryor in Translational Psychiatry. Published online November 1 2016 doi:10.1038/tp.2016.199