Summary: Separating vascular cell data based on sex helps researchers make new discoveries about why males and females are affected by neurodegenerative diseases differently. Findings point to differences in the blood-brain barrier between males and females.
Source: American Institute of Physics
Men and women are impacted differently by brain diseases, like Alzheimer’s disease and Parkinson’s disease. Researchers are urging their colleagues to remember those differences when researching treatments and cures.
In APL Bioengineering, by AIP Publishing, University of Maryland scientists highlight a growing body of research suggesting sex differences play roles in how patients respond to brain diseases, as well as multiple sclerosis, motor neuron disease, and other brain ailments.
That is progress from just a few years ago, said Alisa Morss Clyne, director of the university’s Vascular Kinetics Laboratory.
“I have worked with vascular cells for 20 years and, up until maybe about five years ago, if you asked if the sex of my cells mattered at all, I would have said no,” Clyne said. Then, she worked on a difficult study in which data appeared “all over the place.”
“We separated the cell data by sex, and it all made sense,” Clyne said. “It was an awakening for me that we should be studying this.”
As of 2020, an estimated 5.8 million Americans were diagnosed with Alzheimer’s disease, another 1 million with Parkinson’s disease, 914,000 with multiple sclerosis, and 63,000 with motor neuron disease. These diseases happen when nerve cells in the brain and nervous system quit working and, ultimately, die.
The changes are associated with the breakdown of what is called the blood-brain barrier — a border of cells that keeps the wrong kind of molecules in the bloodstream from entering the brain and damaging it.
Published research has shown differences in the blood-brain barriers of men and women. Some of the research suggests the barrier can be stronger in women than men, and the barriers in men and women are built and behave differently.
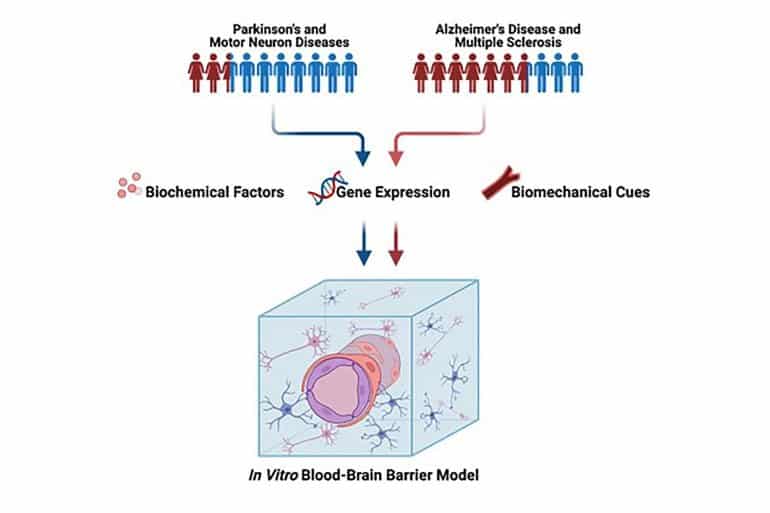
That could factor into known differences in the sexes, such as Alzheimer’s disease being more prevalent in older women than men, while Parkinson’s impacts men more frequently and tends to do so more severely.
The authors said they hope their article will serve as a reminder to researchers not just in their own field, but across the sciences, that accounting for sex differences leads to better results.
“I think there is an awakening in the past 10 years or so that you cannot ignore sex differences,” Clyne said. “My goal is to inspire people to include sex differences in their research, no matter what research they are doing.”
About this neurology research news
Source: American Institute of Physics
Contact: Larry Frum – American Institute of Physics
Image: The image is credited to Callie Weber
Original Research: Open access.
“Sex differences in the blood–brain barrier and neurodegenerative diseases” by Callie M. Weber and Alisa Morss Clynea. APL Bioengineering
Abstract
Sex differences in the blood–brain barrier and neurodegenerative diseases
The number of people diagnosed with neurodegenerative diseases is on the rise. Many of these diseases, including Alzheimer’s disease, Parkinson’s disease, multiple sclerosis, and motor neuron disease, demonstrate clear sexual dimorphisms. While sex as a biological variable must now be included in animal studies, sex is rarely included in in vitro models of human neurodegenerative disease.
In this Review, we describe these sex-related differences in neurodegenerative diseases and the blood–brain barrier (BBB), whose dysfunction is linked to neurodegenerative disease development and progression. We explain potential mechanisms by which sex and sex hormones affect BBB integrity.
Finally, we summarize current in vitro BBB bioengineered models and highlight their potential to study sex differences in BBB integrity and neurodegenerative disease.