NIH-funded team finds rapid-acting, non-addicting agent in mouse study.
A chemical byproduct, or metabolite, created as the body breaks down ketamine likely holds the secret to its rapid antidepressant action, National Institutes of Health (NIH) scientists and grantees have discovered. This metabolite singularly reversed depression-like behaviors in mice without triggering any of the anesthetic, dissociative, or addictive side effects associated with ketamine.
“This discovery fundamentally changes our understanding of how this rapid antidepressant mechanism works and holds promise for development of more robust and safer treatments,” said Carlos Zarate, M.D. of the NIH’s National Institute of Mental Health (NIMH), a study co-author and a pioneer of research using ketamine to treat depression. “By using a team approach, researchers were able to reverse-engineer ketamine’s workings from the clinic to the lab to pinpoint what makes it so unique.”
NIMH grantee Todd Gould, M.D., of the University of Maryland School of Medicine, in collaboration with Zarate and other colleagues, report on their findings May 4, 2016 in the journal Nature. The team also included researchers at the NIH’s National Center for Advancing Translational Sciences (NCATS) and National Institute on Aging (NIA), and the University of North Carolina.
“Now that we know that ketamine’s antidepressant actions in mice are due to a metabolite, not ketamine itself, the next steps are to confirm that it works similarly in humans, and determine if it can lead to improved therapeutics for patients,” explained Gould.
Clinical trials by Zarate and others have shown that ketamine can lift depression in hours, or even minutes – much faster than the most commonly used antidepressant medications now available, which often require weeks to take effect. Further, the antidepressant effects of a single dose can last for a week or longer. However, despite legitimate medical uses, ketamine also has dissociative, euphoric, and addictive properties, making it a potential drug of abuse and limiting its usefulness as a depression medication.
In hopes of finding leads to a more practical treatment, the research team sought to pinpoint the exact mechanism by which ketamine relieves depression. Ketamine belongs to a class of drugs that block cellular receptors for glutamate, the brain’s chief excitatory chemical messenger. Until now, the prevailing view was that ketamine produced its antidepressant effects by blocking N-methyl-D-aspartic acid (NMDA) glutamate receptors.
However, human trials of other NMDA-receptor blockers failed to produce ketamine’s robust and sustained antidepressant effects. So the team explored the effects of ketamine on antidepressant-responsive behaviors in mice. Ketamine harbors two chemical forms that are mirror images of each other, denoted (S)- and (R)-ketamine. The investigators found that while (S)-ketamine is more potent at blocking NMDA receptors, it is less effective in reducing depression-like behaviors than the (R) form.
The team then looked at the effects of the metabolites created as the body breaks down (S)- and (R)-ketamine. It was known that ketamine’s antidepressant effects are greater in female mice. NIA researchers Irving Wainer, Ph.D., and Ruin Moaddel, Ph.D. identified a key metabolite (2S,6S;2R,6R)-HNK (hydroxynorketamine) and showed that it is pharmacologically active. The team then discovered that levels of this metabolite were three times higher in female mice, hinting that it might be responsible for the sex difference in the antidepressant-like effect. To find out, the researchers chemically blocked the metabolism of ketamine. This prevented formation of the metabolite, which blocked the drug’s antidepressant-like effects.
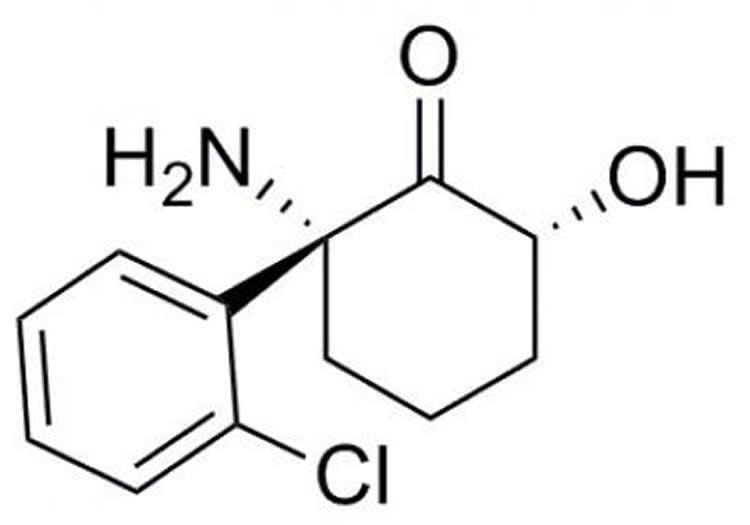
Like ketamine, this metabolite includes two forms that mirror each other. By testing both forms, they found that one – (2R,6R)-HNK – had antidepressant-like effects similar to ketamine, lasting for at least three days in mice. Notably, unlike ketamine, the compound does not inhibit NMDA receptors. It instead activates, possibly indirectly, another type of glutamate receptor, α-amino-3-hydroxy-5-methyl-4-isoxazole propionic acid (AMPA). Blocking AMPA receptors prevented the antidepressant-like effects of (2R,6R)-HNK in mice. The experiments confirmed that the rapid antidepressant-like effects require activation of AMPA receptors, not inhibition of NMDA receptors.
Ketamine also has effects in mice that mimic its dissociative, euphoric effects in humans and underlie its abuse and addictive potential; however, these effects were not observed with (2R,6R)-HNK. (2R,6R)-HNK did not cause the changes in physical activity, sensory processing, and coordination in mice that occur with ketamine. In an experimental situation where mice were able to self-administer medication, they did so with ketamine but not the (2R,6R)-HNK metabolite, indicating that (2R, 6R)-HNK is not addictive.
“Working in collaboration with NIH and academic researchers, NCATS chemists played a critical role in isolating the specific metabolite of ketamine responsible for fighting depression,” said Christopher P. Austin, M.D., NCATS director. “Overall, our collective efforts exemplify how a collaborative, team science approach can help advance the translational process in ways that help get more treatments to more patients more quickly.”
Carlos Zarate, M.D., speeds up treatment for major depression at the National Institutes of Health (NIH) Intramural Research Program (IRP). Dr. Zarate is Chief of the Experimental Therapeutics & Pathophysiology Branch and the Section on the Neurobiology and Treatment of Mood Disorders at the National Institute of Mental Health (NIMH).
“Unraveling the mechanism mediating ketamine’s antidepressant activity is an important step in the process of drug development,” said Richard J. Hodes, M.D., NIA director. “New approaches are critical for the treatment of depression, especially for older adults and for patients who do not respond to current medications.”
“Pending confirmation in humans, this line of studies exemplifies the power of mouse translational experiments for teasing out brain mechanisms that hold promise for future treatment breakthroughs,” added NIMH acting director Bruce Cuthbert, Ph.D.,.
The researchers are now following up on their discovery with safety and toxicity studies of the metabolite as part of a drug development plan in advance of a NIMH clinical trial in humans for the treatment of depression.
Other UT Southwestern researchers who contributed to this study were Dr. Laura Hewitson, Adjunct Associate Professor of Psychiatry at UTSW, and Director of Research at the Johnson Center for Child Health and Development in Austin, Texas; Dr. Umar Yazdani, research scientist; Dr. Bharathi Gadad, clinical research coordinator in Psychiatry; and Wenhao Li, research associate in Cell Biology. Researchers from the Johnson Center for Child Health and Development in Austin also assisted.
Funding: The study was supported by the National Institutes of Health.
Source: Jules Asher – NIH/NIMH
Image Source: The image is credited to NIH – National Center for Advancing Translational Sciences.
Video Source: The video is credited to NIH IRP.
Original Research: Abstract for “NMDAR inhibition-independent antidepressant actions of ketamine metabolites” by Panos Zanos, Ruin Moaddel, Patrick J. Morris, Polymnia Georgiou, Jonathan Fischell, Greg I. Elmer, Manickavasagom Alkondon, Peixiong Yuan, Heather J. Pribut, Nagendra S. Singh, Katina S. S. Dossou, Yuhong Fang, Xi-Ping Huang, Cheryl L. Mayo, Irving W. Wainer, Edson X. Albuquerque, Scott M. Thompson, Craig J. Thomas, Carlos A. Zarate Jr and Todd D. Gould in Nature. Published online May 4 2016 doi:10.1038/nature17998
Abstract
NMDAR inhibition-independent antidepressant actions of ketamine metabolites
Major depressive disorder affects around 16 per cent of the world population at some point in their lives. Despite the availability of numerous monoaminergic-based antidepressants, most patients require several weeks, if not months, to respond to these treatments, and many patients never attain sustained remission of their symptoms. The non-competitive, glutamatergic NMDAR (N-methyl-D-aspartate receptor) antagonist (R,S)-ketamine exerts rapid and sustained antidepressant effects after a single dose in patients with depression, but its use is associated with undesirable side effects. Here we show that the metabolism of (R,S)-ketamine to (2S,6S;2R,6R)-hydroxynorketamine (HNK) is essential for its antidepressant effects, and that the (2R,6R)-HNK enantiomer exerts behavioural, electroencephalographic, electrophysiological and cellular antidepressant-related actions in mice. These antidepressant actions are independent of NMDAR inhibition but involve early and sustained activation of AMPARs (α-amino-3-hydroxy-5-methyl-4-isoxazole propionic acid receptors). We also establish that (2R,6R)-HNK lacks ketamine-related side effects. Our data implicate a novel mechanism underlying the antidepressant properties of (R,S)-ketamine and have relevance for the development of next-generation, rapid-acting antidepressants.
“NMDAR inhibition-independent antidepressant actions of ketamine metabolites” by Panos Zanos, Ruin Moaddel, Patrick J. Morris, Polymnia Georgiou, Jonathan Fischell, Greg I. Elmer, Manickavasagom Alkondon, Peixiong Yuan, Heather J. Pribut, Nagendra S. Singh, Katina S. S. Dossou, Yuhong Fang, Xi-Ping Huang, Cheryl L. Mayo, Irving W. Wainer, Edson X. Albuquerque, Scott M. Thompson, Craig J. Thomas, Carlos A. Zarate Jr and Todd D. Gould in Nature. Published online May 4 2016 doi:10.1038/nature17998