Summary: Age-related macular degeneration and lupus share a common contributor to inflammation. The findings could help researchers develop new treatments for those conditions, and other conditions associated with inflammation.
Source: University of Virginia
Researchers at the University of Virginia School of Medicine have made a discovery linking lupus, a potentially debilitating autoimmune disorder, and macular degeneration, a leading cause of blindness.
The two diseases share a common contributor to harmful inflammation, the scientists found. The insights could let researchers develop new treatments for those diseases and other conditions driven by the newly discovered inflammation source.
“We were quite surprised at the common link between lupus and macular degeneration,” said Jayakrishna Ambati, MD, of UVA’s Department of Ophthalmology and the founding director of UVA’s Center for Advanced Vision Science. “It appears that the new inflammatory pathway we identified could be therapeutically targeted for many chronic diseases.”
Macular Degeneration and Lupus
Ambati and his collaborators have discovered an unknown role for an inflammasome—an agent of the immune system—called NLRC4-NLRP3. Inflammasomes play an important role in marshaling the body’s defenses to protect it from invaders such as viruses and bacteria.
In lupus and atrophic macular degeneration, however, it appears that NLRC4-NLRP3 contributes to harmful inflammation, the UVA researchers found. In lupus, it helps drive the hyperactive immune response that leads to symptoms such as joint pain, rash, fever and more. In macular degeneration, meanwhile, NRC4-NLRP3 appears to contribute to inflammation that destroys the vital light-sensing cells in the eye’s retina.
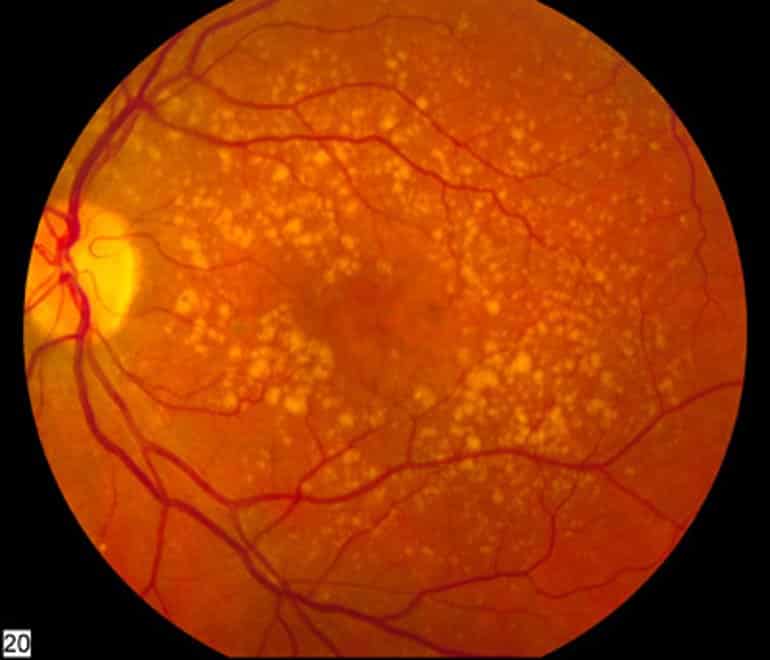
Ambati’s new work helps explain why. The inflammasome, he found, is sent into action by a special class of genetic material called “short interspersed nuclear element RNAs,” or SINE RNAs. This type of RNA makes up more than 10% of our genomes, and it activates in response to cell stresses such as infection, genetic damage and aging. The resulting inflammation caused by SINE RNAs can be harmful in many chronic diseases.
SINE RNAs are elevated in both macular degeneration and lupus, Ambati found. In addition to discovering the role of SINE RNA in the two diseases, Ambati and his colleagues identified an unknown receptor for the SINE RNAs called DDX17. Scientists have been looking for this receptor for decades, and the new discovery helps them better understand the process that leads to the harmful inflammation.
“These findings indicate that blocking a single inflammasome might not be enough, and that targeting both the NLRC4 and NLRP3 inflammasomes would be a superior strategy,” Ambati said.
Using this new information, scientists may be able to target the source of harmful inflammation in lupus, macular degeneration and other diseases driven by SINE RNAs. That could lead to new treatments to benefit patients, the UVA researchers say.
“We’re excited to have developed drugs called Kamuvudines that block this dual inflammasome, which we anticipate will be in clinical trials next year,” Ambati said.
The researchers have published their findings in the scientific journal Science Immunology.
About this inflammation research news
Author: Press Office
Source: University of Virginia
Contact: Press Office – University of Virginia
Image: The image is credited to National Eye Institute, National Institutes of Health
Original Research: Open access.
“DDX17 is an essential mediator of sterile NLRC4 inflammasome activation by retrotransposon RNAs” by Shao-bin Wang et al. Science Immunology
Abstract
DDX17 is an essential mediator of sterile NLRC4 inflammasome activation by retrotransposon RNAs
Detection of microbial products by multiprotein complexes known as inflammasomes is pivotal to host defense against pathogens. Nucleotide-binding domain leucine-rich repeat (NLR) CARD domain containing 4 (NLRC4) forms an inflammasome in response to bacterial products; this requires their detection by NLR family apoptosis inhibitory proteins (NAIPs), with which NLRC4 physically associates. However, the mechanisms underlying sterile NLRC4 inflammasome activation, which is implicated in chronic noninfectious diseases, remain unknown.
Here, we report that endogenous short interspersed nuclear element (SINE) RNAs, which promote atrophic macular degeneration (AMD) and systemic lupus erythematosus (SLE), induce NLRC4 inflammasome activation independent of NAIPs. We identify DDX17, a DExD/H box RNA helicase, as the sensor of SINE RNAs that licenses assembly of an inflammasome comprising NLRC4, NLR pyrin domain–containing protein 3, and apoptosis-associated speck-like protein–containing CARD and induces caspase-1 activation and cytokine release.
Inhibiting DDX17-mediated NLRC4 inflammasome activation decreased interleukin-18 release in peripheral blood mononuclear cells of patients with SLE and prevented retinal degeneration in an animal model of AMD. Our findings uncover a previously unrecognized noncanonical NLRC4 inflammasome activated by endogenous retrotransposons and provide potential therapeutic targets for SINE RNA–driven diseases.







