Summary: Ketamine reduced alcohol intake in male rat models of alcohol use disorder but increased the desire for alcohol in low-consumption females.
Source: SfN
The drug ketamine decreases alcohol consumption in male, but not female, rats, according to new research published in eNeuro. The findings suggest that ketamine may be a viable treatment option for male patients with an alcohol use disorder.
Prior studies found that ketamine reduces alcohol use disorder symptoms in both rats and humans, but the drug was administered once, rather than over a more realistic treatment time period. Ketamine is itself an addictive drug, so it is critical to examine how it affects patients over extended use.
Strong et al. divided male and female rats into groups based on how much alcohol they were prone to consume. The rats were allowed unrestricted access to alcohol three times a week. Three weeks later, ketamine treatments began.
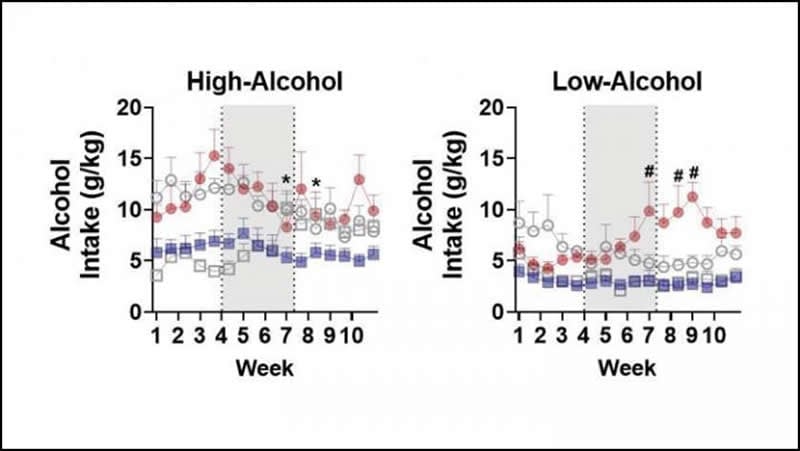
Ketamine administration reduced alcohol consumption in high-consumption male rats, and the effects lasted at least three weeks after the ketamine treatments ended. Ketamine did not affect the habits of high-consumption female rats and increased drinking in low-consumption females. The female rats also displayed a higher risk of abusing ketamine compared to the male rats.
Source:
SfN
Media Contacts:
Calli McMurray – SfN
Image Source:
The image is credited to Strong et al,/eNeuro 2019.
Original Research: Closed access
“Sex and Individual Differences in Alcohol Intake are Associated with Differences in Ketamine Self-Administration Behaviors and Nucleus Accumbens Dendritic Spine Density”. C. E. Strong, K. N. Wright and M. Kabbaj.
eNeuro doi:10.1523/ENEURO.0221-19.2019.
Abstract
Sex and Individual Differences in Alcohol Intake are Associated with Differences in Ketamine Self-Administration Behaviors and Nucleus Accumbens Dendritic Spine Density
Clinical and preclinical studies have shown that ketamine, an NMDA-receptor antagonist, has promising therapeutic value for the treatment of alcohol use disorder (AUD). However, maintenance of remission will ultimately require repeated infusions of ketamine which may lead to abuse potential and may hinder its therapeutic benefits. It is therefore crucial to assess the effects of repeated treatments with ketamine on alcohol intake. Accordingly, this study aimed to examine in both sexes how individual differences in alcohol intake alter ketamine self-administration and how ketamine self-administration will alter subsequent alcohol drinking behaviors. Male and female rats intermittently drank alcohol or water for 10-weeks and were divided into high- or low-alcohol intake groups prior to ketamine self-administration. Rats self-administered ketamine under fixed and progressive ratios schedules of reinforcement from weeks 4-7, and incubation of ketamine craving was examined from weeks 8-10. To investigate structural plasticity in a brain region involved in reward, nucleus accumbens (NAc) dendritic spine morphology was examined. Our results show that high-alcohol intake in male rats attenuated ketamine self-administration whereas in female rats, high-alcohol intake enhanced motivation to self-administer ketamine. Ketamine reduced alcohol intake in high-alcohol male rats but increased it in low-alcohol female rats. Incubation of ketamine craving developed in all groups except low-alcohol females. 3-weeks abstinence from ketamine was associated with increased mushroom spines in all groups except the high-alcohol male group. Overall, these data suggest that ketamine as a treatment for AUD may benefit male but not female subjects and warrants further investigation before use as a therapeutic agent.
Significance statement:
Alcohol use disorder (AUD) is one of the most prevalent forms of addiction yet effective treatment options are lacking. Preclinical and clinical data suggest that ketamine is a potential AUD treatment option. Since ketamine is also an addictive drug, we investigated here the relationship between alcohol and ketamine in both sexes and examined morphological changes in nucleus accumbens (NAc) medium spiny neurons, which are involved in mediating addiction related plasticity. We showed clear individual and sex differences in the interactions between alcohol and ketamine, which were reflected with structural plasticity alterations in the NAc of both sexes. Our data suggest that ketamine could be further investigated in humans as a viable treatment for AUD in male but not female subjects.






