Breakthrough could help countless patients with neurological conditions that are currently hard to treat.
Researchers at Massachusetts Eye and Ear/Harvard Medical School and Boston University have successfully shown neuroprotection in a Parkinson’s mouse model using new techniques to deliver drugs across the naturally impenetrable blood-brain barrier. Their findings, published in Neurosurgery, lend hope to patients around the world with neurological conditions that are difficult to treat due to a barrier mechanism that prevents approximately 98 percent of drugs from reaching the brain and central nervous system.
“We are developing a platform that may eventually be used to deliver a variety of drugs to the brain,” said senior author Benjamin S. Bleier, M.D., of the department of otolaryngology at Mass. Eye and Ear/Harvard Medical School. “Although we are currently looking at neurodegenerative disease, there is potential for the technology to be expanded to psychiatric diseases, chronic pain, seizure disorders and many other conditions affecting the brain and nervous system down the road.”
Using nasal mucosal grafting, researchers delivered glial derived neurotrophic factor (GDNF), a therapeutic protein in testing for treating Parkinson’s disease, to the brains of mice. They showed through behavioral and histological data capture that their delivery method was equivalent to direct injection of GDNF – the current gold standard for delivering this drug in Parkinson’s disease despite its traumatic nature and high complication rates – in diffusing drugs to the brain.
The researchers chose to test their delivery method with GDNF because the therapy has been shown to delay and even reverse disease progression of Parkinson’s disease in pre-clinical models. The study was funded by The Michael J. Fox Foundation for Parkinson’s Research (MJFF).
“Brain diseases are notoriously difficult to treat due to the natural protections the body builds against intrusion,” said Jamie Eberling, PhD, senior associate director of MJFF research programs. “Dr. Bleier’s group has identified a potential avenue to pass that barrier, and we look forward to the next stage of research to further test its utility in people with Parkinson’s disease .”
Nasal mucosal grafting is a technique regularly used in the ENT field to reconstruct the barrier around the brain after surgery to the skull base. ENT surgeons commonly use endoscopic approaches to remove brain tumors through the nose by making a window through the blood-brain barrier to access the brain. Once they have finished the treatment, they use adjacent nasal lining to rebuild the hole in a permanent and safe way. The safety and efficacy of these methods have been well established through long-term clinical outcomes studies in the field, with the nasal lining protecting the brain from infection just as the blood brain barrier has done.
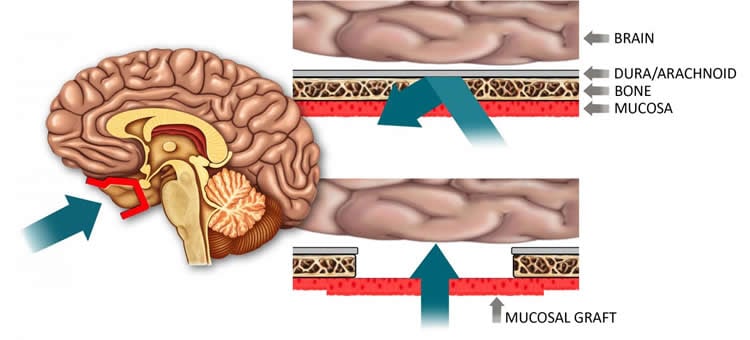
Dr. Bleier saw an opportunity to apply these techniques to the widespread clinical dilemma of delivering drugs across the barrier to the brain and central nervous system. By functionally replacing a section of the blood-brain barrier with nasal mucosa, which is more than 1,000 times more permeable than the native barrier, surgeons may create a “screen door” to allow for drug delivery to the brain and central nervous system.
The technique has the potential to benefit a large population of patients with neurodegenerative disorders, where there remains a specific unmet need for blood-brain penetrating therapeutic delivery strategies.
“We see this expanding beyond Parkinson’s disease, as there are multiple diseases of the brain that do not have good therapeutic options,” Dr. Bleier said. “It is a platform that opens doors for new discovery and could enable drug development for an underserved population.”
Funding: The study was supported by a grant from the Michael J. Fox Foundation for Parkinson’s Research and represents a collaborative effort between Mass. Eye and Ear and Dr. Xue Han of the Biomedical Engineering Department at Boston University. Other authors include Richie E. Kohman, Kevin Guerra, Angela Nocera, Shrestha Ramanlal, Armine H. Kocharyan and William T. Curry.
Source: Suzanne Day – Mass Eye and Ear
Image Credit: The image is credited to Garyfallia Pagonis and Benjamin S. Bleier, M.D.
Original Research: Abstract for “Heterotopic Mucosal Grafting Enables the Delivery of Therapeutic Neuropeptides Across the Blood Brain Barrier” by Bleier, Benjamin S. MD; Kohman, Richie E. PhD; Guerra, Kevin BS; Nocera, Angela L. MS; Ramanlal, Shreshtha BS; Kocharyan, Armine H. MD; Curry, William T. MD; Han, and Xue PhD in Neurosurgery. Published online September 8 2015 doi:10.1227/NEU.0000000000001016
Abstract
Heterotopic Mucosal Grafting Enables the Delivery of Therapeutic Neuropeptides Across the Blood Brain Barrier
BACKGROUND: The blood-brain barrier represents a fundamental limitation in treating neurological disease because it prevents all neuropeptides from reaching the central nervous system (CNS). Currently, there is no efficient method to permanently bypass the blood-brain barrier.
OBJECTIVE: To test the feasibility of using nasal mucosal graft reconstruction of arachnoid defects to deliver glial-derived neurotrophic factor (GDNF) for the treatment of Parkinson disease in a mouse model.
METHODS: The Institutional Animal Care and Use Committee approved this study in an established murine 6-hydroxydopamine Parkinson disease model. A parietal craniotomy and arachnoid defect was repaired with a heterotopic donor mucosal graft. The therapeutic efficacy of GDNF (2 [mu]g/mL) delivered through the mucosal graft was compared with direct intrastriatal GDNF injection (2 [mu]g/mL) and saline control through the use of 2 behavioral assays (rotarod and apomorphine rotation). An immunohistological analysis was further used to compare the relative preservation of substantia nigra cell bodies between treatment groups.
RESULTS: Transmucosal GDNF was equivalent to direct intrastriatal injection at preserving motor function at week 7 in both the rotarod and apomorphine rotation behavioral assays. Similarly, both transmucosal and intrastriatal GDNF demonstrated an equivalent ratio of preserved substantia nigra cell bodies (0.79 +/- 0.14 and 0.78 +/- 0.09, respectively, P = NS) compared with the contralateral control side, and both were significantly greater than saline control (0.53 +/- 0.21; P = .01 and P = .03, respectively).
CONCLUSION: Transmucosal delivery of GDNF is equivalent to direct intrastriatal injection at ameliorating the behavioral and immunohistological features of Parkinson disease in a murine model. Mucosal grafting of arachnoid defects is a technique commonly used for endoscopic skull base reconstruction and may represent a novel method to permanently bypass the blood-brain barrier.
“Heterotopic Mucosal Grafting Enables the Delivery of Therapeutic Neuropeptides Across the Blood Brain Barrier” by Bleier, Benjamin S. MD; Kohman, Richie E. PhD; Guerra, Kevin BS; Nocera, Angela L. MS; Ramanlal, Shreshtha BS; Kocharyan, Armine H. MD; Curry, William T. MD; Han, and Xue PhD in Neurosurgery. Published online September 8 2015 doi:10.1227/NEU.0000000000001016






