Summary: Cannabidiol (CBD) increases cerebral blood flow to areas of the brain associated with memory processing, specifically the hippocampus. The findings identify a potential mechanism for the use of CBD to treat disorders associated with altered memory processing, including Alzheimer’s disease, PTSD, and schizophrenia.
Source: UCL
A single dose of cannabidiol (CBD) helped increase blood flow to the hippocampus, an important area of the brain associated with memory and emotion, finds a new study led by UCL researchers.
Researchers say the findings could be an important discovery for conditions which affect memory, such as Alzheimer’s disease and post-traumatic stress disorder (PTSD), and could help better target therapies.
In the study, published in the Journal of Psychopharmacology, researchers set out to investigate how CBD influences cerebral blood flow in different regions on the brain involved in memory processing.
Lead author, Dr Michael Bloomfield (UCL Psychiatry) said: “Cannabidiol is one of the main constituents of cannabis and is gaining interest for its therapeutic potential.
“There is evidence that CBD may help reduce symptoms of psychosis and anxiety. There is some evidence to suggest that CBD may improve memory function.
“Additionally, CBD changes how the brain processes emotional memories, which could help to explain its reputed therapeutic effects in PTSD and other psychiatric disorders. However, the precise mechanisms underlying the effects of CBD on memory are unclear.”
For the randomised controlled study, 15 healthy young adult participants, with little or no history of cannabis use were selected.
On different occasions, separated by at least a week, each participant was given a 600mg of oral CBD or a placebo. The doses came in identical capsules, so participants didn’t know which one they were taking on which occasion.
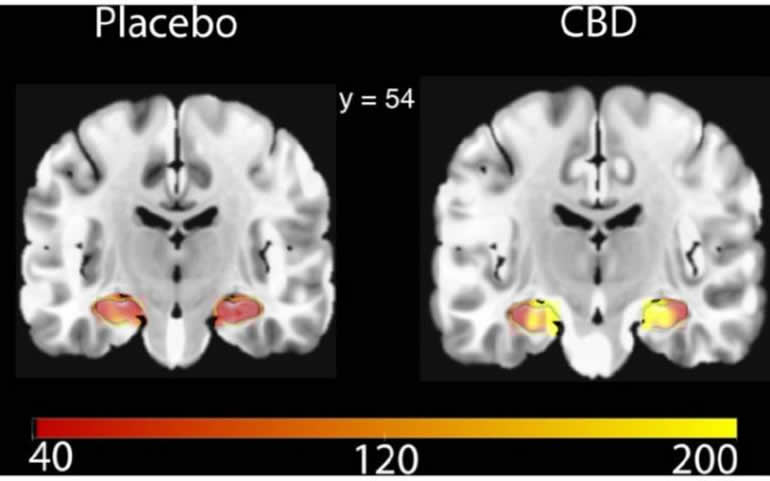
Researchers measured blood flow to the hippocampus using ‘arterial spin labelling’ – a magnetic resonance imaging (MRI) brain scanning technique which measures changes in the blood oxygen levels.
Findings
CBD significantly increased blood flow in the hippocampus, however CBD did not cause significant differences in blood flow in other regions of the medial temporal lobe (MTL), of which the hippocampus is a significant component.
In the prefrontal cortex, the area of the brain used for planning and decision making, CBD caused a significant increase in blood flow in the orbitofrontal cortex.
Dr Bloomfield added: “To our knowledge, this is the first study to find that CBD increases blood flow to key regions involved in memory processing, particularly the hippocampus.”
“This supports the view that CBD has region-specific blood flow effects in the human brain, which has previously been disputed.
“If replicated, these results could lead to further research across a range of conditions characterised by changes in how the brain processes memories, including Alzheimer’s disease, where there are defects in the control of blood control flow, along with schizophrenia and post-traumatic stress disorder.”
Study limitations
This study used a single dose of CBD in healthy volunteers, which may not translate to the effects of repeated CBD dosing.
Funding: This research was funded by British Medical Association award.
About this neurology research article
Source:
UCL
Contacts:
Henry Killworth – UCL
Image Source:
The image is credited to the researchers.
Original Research: Open access
“The effects of acute cannabidiol on cerebral blood flow and its relationship to memory: An arterial spin labelling magnetic resonance imaging study” by Michael Bloomfield et al. Journal of Psychopharmacology.
Abstract
The effects of acute cannabidiol on cerebral blood flow and its relationship to memory: An arterial spin labelling magnetic resonance imaging study
Background:
Cannabidiol (CBD) is being investigated as a potential treatment for several medical indications, many of which are characterised by altered memory processing. However, the mechanisms underlying these effects are unclear.
Aims:
Our primary aim was to investigate how CBD influences cerebral blood flow (CBF) in regions involved in memory processing. Our secondary aim was to determine if the effects of CBD on CBF were associated with differences in working and episodic memory task performance.
Methods:
We used a randomised, crossover, double-blind design in which 15 healthy participants were administered 600 mg oral CBD or placebo on separate days. We measured regional CBF at rest using arterial spin labelling 3 h after drug ingestion. We assessed working memory with the digit span (forward, backward) and n-back (0-back, 1-back, 2-back) tasks, and we used a prose recall task (immediate and delayed) to assess episodic memory.
Results:
CBD increased CBF in the hippocampus (mean (95% confidence intervals) = 15.00 (5.78–24.21) mL/100 g/min, t14 = 3.489, Cohen’s d = 0.75, p = 0.004). There were no differences in memory task performance, but there was a significant correlation whereby greater CBD-induced increases in orbitofrontal CBF were associated with reduced reaction time on the 2-back working memory task ( r= −0.73, p = 0.005).
Conclusions:
These findings suggest that CBD increases CBF to key regions involved in memory processing, particularly the hippocampus. These results identify potential mechanisms of CBD for a range of conditions associated with altered memory processing, including Alzheimer’s disease, schizophrenia, post-traumatic stress disorder and cannabis-use disorders.







