Summary: According to researchers, a reorganization of wiring in the brain could be an underlying cause of phantom limb pain experienced by amputees.
Source: University of Cambridge.
Researchers have identified the cause of chronic, and currently untreatable, pain in those with amputations and severe nerve damage, as well as a potential treatment which relies on engineering instead of drugs.
Researchers have discovered that a ‘reorganisation’ of the wiring of the brain is the underlying cause of phantom limb pain, which occurs in the vast majority of individuals who have had limbs amputated, and a potential method of treating it which uses artificial intelligence techniques.
The researchers, led by a group from Osaka University in Japan in collaboration with the University of Cambridge, used a brain-machine interface to train a group of ten individuals to control a robotic arm with their brains. They found that if a patient tried to control the prosthetic by associating the movement with their missing arm, it increased their pain, but training them to associate the movement of the prosthetic with the unaffected hand decreased their pain.
Their results, reported in the journal Nature Communications, demonstrate that in patients with chronic pain associated with amputation or nerve injury, there are ‘crossed wires’ in the part of the brain associated with sensation and movement, and that by mending that disruption, the pain can be treated. The findings could also be applied to those with other forms of chronic pain, including pain due to arthritis.
Approximately 5,000 amputations are carried out in the UK every year, and those with type 1 or type 2 diabetes are at particular risk of needing an amputation. In most cases, individuals who have had a hand or arm amputated, or who have had severe nerve injuries which result in a loss of sensation in their hand, continue to feel the existence of the affected hand as if it were still there. Between 50 and 80 percent of these patients suffer with chronic pain in the ‘phantom’ hand, known as phantom limb pain.
“Even though the hand is gone, people with phantom limb pain still feel like there’s a hand there – it basically feels painful, like a burning or hypersensitive type of pain, and conventional painkillers are ineffective in treating it,” said study co-author Dr Ben Seymour, a neuroscientist based in Cambridge’s Department of Engineering. “We wanted to see if we could come up with an engineering-based treatment as opposed to a drug-based treatment.”
A popular theory of the cause of phantom limb pain is faulty ‘wiring’ of the sensorimotor cortex, the part of the brain that is responsible for processing sensory inputs and executing movements. In other words, there is a mismatch between a movement and the perception of that movement.
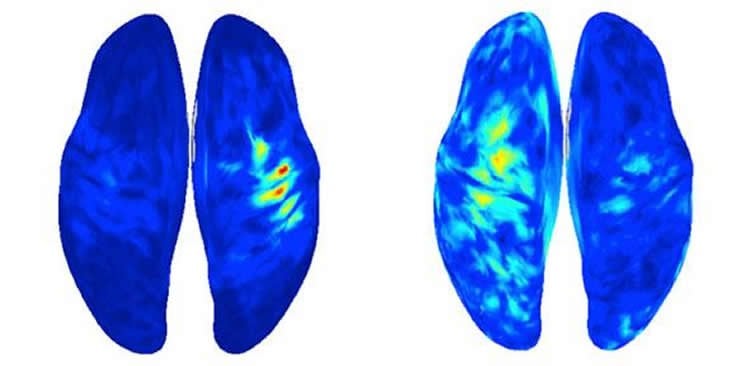
In the study, Seymour and his colleagues, led by Takufumi Yanagisawa from Osaka University, used a brain-machine interface to decode the neural activity of the mental action needed for a patient to move their ‘phantom’ hand, and then converted the decoded phantom hand movement into that of a robotic neuroprosthetic using artificial intelligence techniques.
“We found that the better their affected side of the brain got at using the robotic arm, the worse their pain got,” said Yanagisawa. “The movement part of the brain is working fine, but they are not getting sensory feedback – there’s a discrepancy there.”
The researchers then altered their technique to train the ‘wrong’ side of the brain: for example, a patient who was missing their left arm was trained to move the prosthetic arm by decoding movements associated with their right arm, or vice versa. When they were trained in this counter-intuitive technique, the patients found that their pain significantly decreased. As they learned to control the arm in this way, it takes advantage of the plasticity – the ability of the brain to restructure and learn new things – of the sensorimotor cortex, showing a clear link between plasticity and pain.
Although the results are promising, Seymour warns that the effects are temporary, and require a large, expensive piece of medical equipment to be effective. However, he believes that a treatment based on their technique could be available within five to ten years. “Ideally, we’d like to see something that people could have at home, or that they could incorporate with physio treatments,” he said. “But the results demonstrate that combining AI techniques with new technologies is a promising avenue for treating pain, and an important area for future UK-Japan research collaboration.”
Source: Sarah Collins – University of Cambridge
Image Source: NeuroscienceNews.com image is credited to Osaka University.
Original Research: Full open access research for “Induced sensorimotor brain plasticity controls pain in phantom limb patients” by Takufumi Yanagisawa, Ryohei Fukuma, Ben Seymour, Koichi Hosomi, Haruhiko Kishima, Takeshi Shimizu, Hiroshi Yokoi, Masayuki Hirata, Toshiki Yoshimine, Yukiyasu Kamitani and Youichi Saitoh in Nature Communications. Published online October 27 2016 doi:10.1038/ncomms13209
[cbtabs][cbtab title=”MLA”]University of Cambridge “Cause of Phantom Limb Pain in Amputees Identified.” NeuroscienceNews. NeuroscienceNews, 27 October 2016.
<https://neurosciencenews.com/amputee-phantom-limb-pain-5366/>.[/cbtab][cbtab title=”APA”]University of Cambridge (2016, October 27). Cause of Phantom Limb Pain in Amputees Identified. NeuroscienceNew. Retrieved October 27, 2016 from https://neurosciencenews.com/amputee-phantom-limb-pain-5366/[/cbtab][cbtab title=”Chicago”]University of Cambridge “Cause of Phantom Limb Pain in Amputees Identified.” https://neurosciencenews.com/amputee-phantom-limb-pain-5366/ (accessed October 27, 2016).[/cbtab][/cbtabs]
Abstract
Induced sensorimotor brain plasticity controls pain in phantom limb patients
The cause of pain in a phantom limb after partial or complete deafferentation is an important problem. A popular but increasingly controversial theory is that it results from maladaptive reorganization of the sensorimotor cortex, suggesting that experimental induction of further reorganization should affect the pain, especially if it results in functional restoration. Here we use a brain–machine interface (BMI) based on real-time magnetoencephalography signals to reconstruct affected hand movements with a robotic hand. BMI training induces significant plasticity in the sensorimotor cortex, manifested as improved discriminability of movement information and enhanced prosthetic control. Contrary to our expectation that functional restoration would reduce pain, the BMI training with the phantom hand intensifies the pain. In contrast, BMI training designed to dissociate the prosthetic and phantom hands actually reduces pain. These results reveal a functional relevance between sensorimotor cortical plasticity and pain, and may provide a novel treatment with BMI neurofeedback.
“Induced sensorimotor brain plasticity controls pain in phantom limb patients” by Takufumi Yanagisawa, Ryohei Fukuma, Ben Seymour, Koichi Hosomi, Haruhiko Kishima, Takeshi Shimizu, Hiroshi Yokoi, Masayuki Hirata, Toshiki Yoshimine, Yukiyasu Kamitani and Youichi Saitoh in Nature Communications. Published online October 27 2016 doi:10.1038/ncomms13209






