Summary: Researchers report a drug developed to target amyloid plaques in those with Alzheimer’s does not significantly slow cognitive decline.
Source: Columbia University Medical Center.
A paper published today in the New England Journal of Medicine reports that solanezumab, a monoclonal antibody-based treatment for Alzheimer’s disease developed by Eli Lilly that targets amyloid plaques, did not significantly slow cognitive decline.
Columbia University Irving Medical Center (CUIMC) led the multicenter study.
Researchers have proposed that Alzheimer’s disease is caused by the buildup of a sticky protein called beta-amyloid. According to this ‘amyloid hypothesis,’ the protein forms plaques in the brain that damage and eventually destroy brain cells. Solanezumab was designed to reduce the level of soluble amyloid molecules before they aggregate.
A total of 2,129 patients with mild dementia due to Alzheimer’s disease participated in the double-blind, placebo-controlled, phase 3 multicenter trial. This study was the first major Alzheimer’s clinical trial to require molecular evidence of amyloid deposition in the brain for enrollment. While the treatment did have some favorable effects, in the main measure of outcome–measured with a cognitive test called the Alzheimer’s Disease Assessment Scale-cognitive subscale–the researchers did not observe any statistically significant benefit compared with placebo.
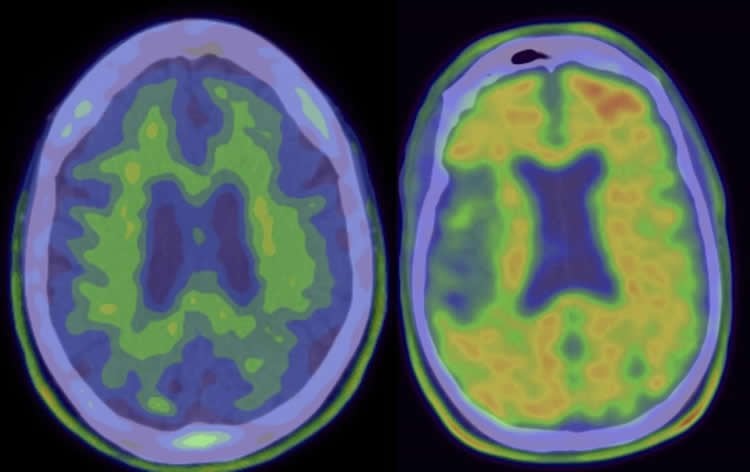
The authors suggest that while it is not certain that this particular strategy or drug could be effective, it is possible that either not enough drug was administered or that the drug needs to be administered earlier in the disease course.
In other studies ongoing at CUIMC, solanezumab is being evaluated in presymptomatic patients at risk of Alzheimer’s disease. Other Alzheimer’s drugs are also in development and being tested at higher doses.
“Although we are disappointed that this particular drug did not prove successful, the field is benefiting from each study,” says lead author Lawrence Honig, MD, PhD, professor of neurology at CUIMC. “There is hope that one of the newer ongoing studies may result in an effective treatment for slowing the course of Alzheimer’s disease.”
The results of this study were first released in late 2016 at the international Clinical Trials on Alzheimer’s Disease meeting in San Diego.
Additional authors are Bruno Vellas, M.D., Michael Woodward, M.D., Merc. Boada, M.D., Ph.D., Roger Bullock, M.D., Michael Borrie, M.B., Ch.B., Klaus Hager, M.D., Niels Andreasen, M.D., Ph.D., Elio Scarpini, M.D., Hong Liu Seifert, Ph.D., Michael Case, M.S., Robert A. Dean, M.D., Ph.D., Ann Hake, M.D., Karen Sundell, B.S., Vicki Poole Hoffmann, Pharm.D., Christopher Carlson, Ph.D., Rashna Khanna, M.D., Mark Mintun, M.D., Ronald DeMattos, Ph.D., Katherine J. Selzler, Ph.D., and Eric Siemers, M.D.
Funding: The study was designed and funded by Eli Lilly and Company.
Source: Lucky Tran – Columbia University Medical Center
Publisher: Organized by NeuroscienceNews.com.
Image Source: NeuroscienceNews.com image is credited to Columbia University Medical Center.
Original Research: Abstract in New England Journal of Medicine.
doi:10.1056/NEJMoa1705971
[cbtabs][cbtab title=”MLA”]Columbia University Medical Center “Alzheimer’s Drug Falls Short in Large Clinical Trial.” NeuroscienceNews. NeuroscienceNews, 25 January 2018.
<https://neurosciencenews.com/alzheimers-drug-trial-8367/>.[/cbtab][cbtab title=”APA”]Columbia University Medical Center (2018, January 25). Alzheimer’s Drug Falls Short in Large Clinical Trial. NeuroscienceNews. Retrieved January 25, 2018 from https://neurosciencenews.com/alzheimers-drug-trial-8367/[/cbtab][cbtab title=”Chicago”]Columbia University Medical Center “Alzheimer’s Drug Falls Short in Large Clinical Trial.” https://neurosciencenews.com/alzheimers-drug-trial-8367/ (accessed January 25, 2018).[/cbtab][/cbtabs]
Abstract
Trial of Solanezumab for Mild Dementia Due to Alzheimer’s Disease
BACKGROUND
Alzheimer’s disease is characterized by amyloid-beta (Aβ) plaques and neurofibrillary tangles. The humanized monoclonal antibody solanezumab was designed to increase the clearance from the brain of soluble Aβ, peptides that may lead to toxic effects in the synapses and precede the deposition of fibrillary amyloid.
METHODS
We conducted a double-blind, placebo-controlled, phase 3 trial involving patients with mild dementia due to Alzheimer’s disease, defined as a Mini–Mental State Examination (MMSE) score of 20 to 26 (on a scale from 0 to 30, with higher scores indicating better cognition) and with amyloid deposition shown by means of florbetapir positron-emission tomography or Aβ1-42 measurements in cerebrospinal fluid. Patients were randomly assigned to receive solanezumab at a dose of 400 mg or placebo intravenously every 4 weeks for 76 weeks. The primary outcome was the change from baseline to week 80 in the score on the 14-item cognitive subscale of the Alzheimer’s Disease Assessment Scale (ADAS-cog14; scores range from 0 to 90, with higher scores indicating greater cognitive impairment).
RESULTS
A total of 2129 patients were enrolled, of whom 1057 were assigned to receive solanezumab and 1072 to receive placebo. The mean change from baseline in the ADAS-cog14 score was 6.65 in the solanezumab group and 7.44 in the placebo group, with no significant between-group difference at week 80 (difference, −0.80; 95% confidence interval, −1.73 to 0.14; P=0.10). As a result of the failure to reach significance with regard to the primary outcome in the prespecified hierarchical analysis, the secondary outcomes were considered to be descriptive and are reported without significance testing. The change from baseline in the MMSE score was −3.17 in the solanezumab group and −3.66 in the placebo group. Adverse cerebral edema or effusion lesions that were observed on magnetic resonance imaging after randomization occurred in 1 patient in the solanezumab group and in 2 in the placebo group.
CONCLUSIONS
Solanezumab at a dose of 400 mg administered every 4 weeks in patients with mild Alzheimer’s disease did not significantly affect cognitive decline. (Funded by Eli Lilly; EXPEDITION3 ClinicalTrials.gov number, NCT01900665.)






