Summary: PET study finds early accumulation of the tau protein in the brain is a better predictor of Alzheimer’s associated memory decline than amyloid plaque accumulation or cerebrospinal fluid biomarkers.
Source: Karolinska Institute
Researchers at Karolinska Institutet in Sweden have compared how well different Alzheimer’s biomarkers predict the progression of the disease and its effect on the memory. They found that early accumulation of tau proteins in the brain as measured by PET scanner was more effective at predicting memory impairment than biomarkers in the cerebrospinal fluid or amyloid plaque in the brain.
The results are published in the journal Molecular Psychiatry.
Over 50 million people around the world suffer from dementia. Alzheimer’s disease is the most common form of dementia and is characterised by an accumulation of the proteins beta-amyloid (Ab) and tau in the brain, followed by a continuous progression in memory decline. The pathological progression can take different forms and it is difficult to predict how quickly the symptoms will develop in any particular individual.
Moreover, the presence of Ab in a person’s brain – known as amyloid plaque – does not necessarily mean that the he or she will develop Alzheimer’s dementia.
“There’s been a rapid development of different Alzheimer’s biomarkers in recent years, enabling us to measure and detect early signs of the disease in patients,” says the study’s first author Marco Bucci, researcher at the Center for Alzheimer Research, part of the Department of Neurobiology, Care Sciences and Society, Karolinska Institutet. “But we still need to find tests that can predict the development of the disease with greater specificity, so that we can improve not only its diagnosis but also its prognosis and treatment.”
Some biomarkers identify accumulations of Aβ or tau, while others are used to measure the loss of nerve function (neurodegeneration). Protein accumulation and neurodegeneration can be measured in the cerebrospinal fluid (CSF) and plasma, or through brain imaging using positron emission tomography (PET) and magnetic resonance imaging (MRI).
Current guidelines for the early detection of Alzheimer’s disease with biomarkers endorse the interchangeability of brain imaging methods and analyses of CSF biomarkers (pTau and Ab), but this has been mooted. There is also a lack of longitudinal studies showing how the biomarkers are linked to gradual cognitive impairment.
“Our study shows that the presence of amyloid plaque in the brain and changes in concentrations of Ab and pTau in the CSF can be detected early during the course of the disease, but they do not seem to have any correlation with later memory loss,” says Dr Bucci.
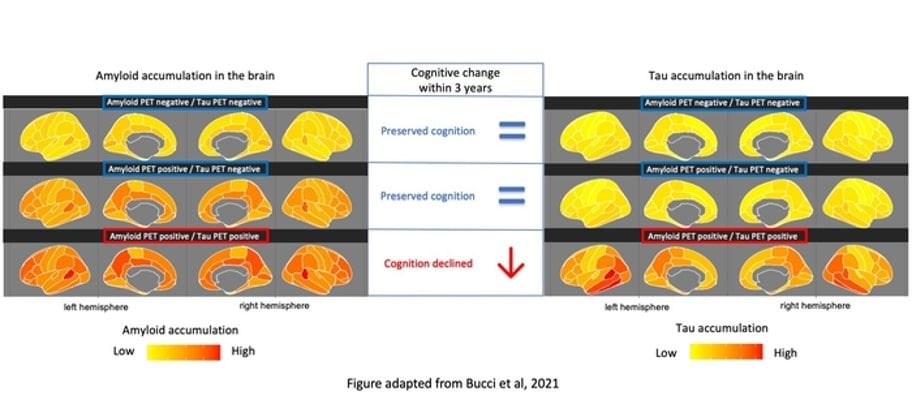
“However, our results show that the presence of tau in the brain measured by a PET scanner is linked to a rapid decline, especially of the episodic memory, which is often affected at an early stage of the disease. Our observation suggests that tau PET should be recommended for the clinical prognostic assessment of cognitive decline in Alzheimer’s patients.”
The results are based on brain imaging (PET and MRI) and CSF analyses in a group of 282 participants comprising people with mild cognitive impairment, people with Alzheimer’s dementia and healthy controls. 213 of the participants were also monitored for three years with tests of episodic memory (i.e. short term memory related to daily events).
“Our findings show that the concentration of tau in the brain in Alzheimer’s disease plays an important part in its pathological progression and may become a key target for future drug treatments,” says principal investigator Agneta Nordberg, professor at the Center for Alzheimer Research, Karolinska Institutet.
Funding: The study was financed by the Swedish Foundation for Strategic Research, the Swedish Research Council, Region Stockholm, the Swedish Brain Fund, the Swedish Alzheimer’s Foundation, the Centre for Innovative Medicine and the Swedish Society for Medical Research. There are no reported conflicts of interest.
About this Alzheimer’s disease research news
Author: Press Office
Source: Karolinska Institute
Contact: Press Office – Karolinska Institute
Image: The image is credited to Marco Bucci
Original Research: Open access.
“Alzheimer’s disease profiled by fluid and imaging markers: Tau PET best predicts cognitive decline” by Marco Bucci, Konstantinos Chiotis & Agneta Nordberg for the Alzheimer’s Disease Neuroimaging Initiative. Molecular Psychiatry
Abstract
Alzheimer’s disease profiled by fluid and imaging markers: Tau PET best predicts cognitive decline
For early detection of Alzheimer’s disease, it is important to find biomarkers with predictive value for disease progression and clinical manifestations, such as cognitive decline. Individuals can now be profiled based on their biomarker status for Aβ42 (A) or tau (T) deposition and neurodegeneration (N).
The aim of this study was to compare the cerebrospinal fluid (CSF) and imaging (PET/MR) biomarkers in each ATN category and to assess their ability to predict longitudinal cognitive decline. A subset of 282 patients, who had had at the same time PET investigations with amyloid-β and tau tracers, CSF sampling, and structural MRI (18% within 13 months), was selected from the ADNI dataset.
The participants were grouped by clinical diagnosis at that time: cognitively normal, subjective memory concern, early or late mild cognitive impairment, or AD. Agreement between CSF (amyloid-β-1-42(A), phosphorylated-Tau181(T), total-Tau(N)), and imaging (amyloid-β PET (florbetaben and florbetapir)(A), tau PET (flortaucipir)(T), hippocampal volume (MRI)(N)) positivity in ATN was assessed with Cohen’s Kappa. Linear mixed-effects models were used to predict decline in the episodic memory.
There was moderate agreement between PET and CSF for A biomarkers (Kappa = 0.39–0.71), while only fair agreement for T biomarkers (Kappa ≤ 0.40, except AD) and discordance for N biomarkers across all groups (Kappa ≤ 0.14) was found. Baseline PET tau predicted longitudinal decline in episodic memory irrespective of CSF p-Tau181 positivity (p ≤ 0.02). Baseline PET tau and amyloid-β predicted decline in episodic memory (p ≤ 0.0001), but isolated PET amyloid-β did not. Isolated PET Tau positivity was only observed in 2 participants (0.71% of the sample).
While results for amyloid-β were similar using CSF or imaging, CSF and imaging results for tau and neurodegeneration were not interchangeable. PET tau positivity was superior to CSF p-Tau181 and PET amyloid-β in predicting cognitive decline in the AD continuum within 3 years of follow-up.






