Summary: Smoking causes white matter scarring in the brain, and the effects do more harm than previously believed.
Source: NTNU
It’s quite possible that you are one of those people with white spots on the brain. Healthy people aren’t spared them, but sick individuals may be more vulnerable. If you smoke, the risk increases even more..
You probably don’t notice them too much unless your doctor has you get into an MRI machine.
Then you can see them. White spots on the brain. These are the scars in your white matter.
A bit unpleasant to think about, but is there really a problem if they’re so common?
“Both yes and no,” says Asta Håberg, a neuroscience professor at NTNU.
“White spots are the most common age-related finding, but they’re not good for the brain, because it makes it more vulnerable,” says Håberg.
She has just discovered something new.
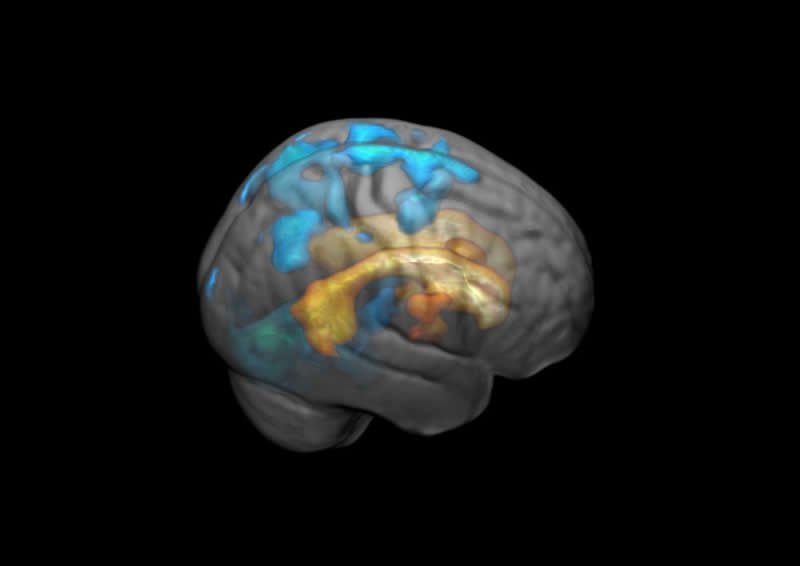
If you have scarring in the white matter in the brain, it not surprisingly affects the area where the scar is. What Håberg and her colleagues found was that completely different parts of the brain are also affected by the scarring.
Including areas far removed from the scarred tissue.
As with many other things in life, the scars start deep and spread out.
“The effects of the white spots spread across the surface of the brain and increase in volume,” says Håberg.
This finding makes things a little more worrisome. It doesn’t help that scientists don’t really know why the white spots appear at all. Ever since they were discovered, they have been a mystery.
But a few pieces of the puzzle are in place.
“Smoking and high blood pressure increase the risk,” says Håberg.
Fortunately, there’s been a shift in this habit. Fewer young people now take up smoking. Among individuals who started when they were young, some are obviously still caught in tobacco’s grip. Statistics Norway data shows that twelve percent of Norway’s population smoked in 2018.
Smoking is more prevalent among people in the 65-74 age group than among those who are 49 years old or younger.
The risk of numerous different brain diseases — such as dementia or stroke — increases with age.
“Keeping your brain as healthy as possible can reduce the negative effects of other brain diseases. Regular health advice regarding high blood pressure and not smoking are both good for the body and the brain,” says Håberg.
Source:
NTNU
Media Contacts:
Asta Håberg – NTNU
Image Source:
The image is credited to NTNU.
Original Research: Open access
“The effect of white matter hyperintensities on regional brain volumes and white matter microstructure, a population-based study in HUNT”. Torgil Riise Vangberg, Live Eikenes, Asta K. Håberg.
NeuroImage doi:10.1016/j.neuroimage.2019.116158.
Abstract
The effect of white matter hyperintensities on regional brain volumes and white matter microstructure, a population-based study in HUNT
Even though age-related white matter hyperintensities (WMH) begin to emerge in middle age, their effect on brain micro- and macrostructure in this age group is not fully elucidated. We have examined how presence of WMH and load of WMH affect regional brain volumes and microstructure in a validated, representative general population sample of 873 individuals between 50 and 66 years. Presence of WMH was determined as Fazakas grade ≥1. WMH load was WMH volume from manual tracing of WMHs divided on intracranial volume. The impact of age appropriate WMH (Fazakas grade 1) on the brain was also investigated. Major novel findings were that even the age appropriate WMH group had widespread macro- and microstructural changes in gray and white matter, showing that the mere presence of WMH, not just WMH load is an important clinical indicator of brain health. With increasing WMH load, structural changes spread centrifugally. Further, we found three major patterns of FA and MD changes related to increasing WMH load, demonstrating a heterogeneous effect on white matter microstructure, where distinct patterns were found in the proximity of the lesions, in deep white matter and in white matter near the cortex. This study also raises several questions about the onset of WMH related pathology, in particular, whether some of the aberrant brain structural and microstructural findings are present before the emergence of WMH. We also found, similar to other studies, that WMH risk factors had low explanatory power for WMH, making it unclear which factors lead to WMH.







