In what may be the largest study of sleep problems among individuals with multiple sclerosis (MS), researchers at UC Davis have found that widely undiagnosed sleep disorders may be at the root of the most common and disabling symptom of the disease: fatigue.
Conducted in over 2,300 individuals in Northern California with multiple sclerosis, the large, population-based study found that, overall, more than 70 percent of participants screened positive for one or more sleep disorders.
The research highlights the importance of diagnosing the root causes of fatigue among individuals with MS, as sleep disorders may affect the course of the disease as well as the overall health and well-being of sufferers, the authors said.
The study “The Underdiagnosis of Sleep Disorders in Patients with Multiple Sclerosis,” is published online today in the Journal of Clinical Sleep Medicine.
“A large percentage of MS subjects in our study are sleep deprived and screened positive for one or more sleep disorders,” said Steven Brass, associate clinical professor and director of the Neurology Sleep Clinical Program and co-medical director of the UC Davis Sleep Medicine Laboratory.
“The vast majority of these sleep disorders are potentially undiagnosed and untreated,” he said. “This work suggests that patients with MS may have sleep disorders requiring independent diagnosis and management.”
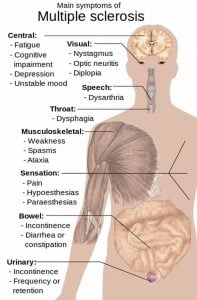
Fatigue is the hallmark of multiple sclerosis, an inflammatory disease affecting the white matter and spinal cord of sufferers. MS symptoms include loss of vision, vertigo, weakness and numbness. Patients also may experience psychiatric symptoms. Disease onset generally is between the ages of 20 and 50 years. The cause of MS is not known, although it is believed to be an autoimmune condition.
Sleep disorders are known to occur more frequently among patients with MS. To gauge the extent of sleep disorders, such as obstructive sleep apnea and insomnia, Brass and his colleagues surveyed members of the Northern California Chapter of the National MS Society. Subjects were recruited in 2011.
More than 11,000 surveys were mailed to prospective participants. Of those, 2,375 met criteria and were included in the study. Consistent with the reported epidemiology of multiple sclerosis, the majority (81 percent) were female and Caucasian (88 percent). The mean age of the participants was 54.
Participants were asked to complete a 10-page survey, which included a detailed sleep history and questions assessing obstructive sleep apnea, daytime sleepiness, insomnia and restless legs syndrome.
Most of the participants – nearly 52 percent – said it took them more than one half hour to fall asleep at night, and nearly 11 percent reported taking a medication to fall asleep. Close to 38 percent of participants screened positive for obstructive sleep apnea. Nearly 32 percent had moderate to severe insomnia and nearly 37 percent had restless legs syndrome.
However, most of the participants had not been diagnosed with a sleep disorder by a physician. While nearly 38 percent reported having obstructive sleep apnea, only a little more than 4 percent reported being diagnosed by a physician with the condition. Similar statistics were seen for other sleep disorders.
“This study shows that sleep disorder frequency, sleep patterns and complaints of excessive daytime sleepiness suggest that sleep problems may be a hidden epidemic in the MS population, separate from MS fatigue,” Brass said.
Other study authors include Chin-Shang Li of UC Davis and Sanford Auerbach of Boston University.
The study was funded by a grant from the National Center for Advancing Translational Sciences and the National Institutes of Health through grant UL1 TR000002.
Contact: Phyllis Brown – UC Davis
Source: UC Davis press release
Image Source: The image is credited to Mikael Häggström and is in the public domain
Original Research: Abstract for “The Underdiagnosis of Sleep Disorders in Patients with Multiple Sclerosis” by Steven D. Brass, M.D., M.P.H., M.B.A.; Chin-Shang Li, Ph.D.; and Sanford Auerbach, M.D., F.A.A.S.M. in Journal of Clinical Sleep Medicine. Published online September 2014 doi:10.5664/jcsm.4044