Low levels of the naturally occurring protein progranulin exacerbate cellular and cognitive dysfunction, while raising levels can prevent abnormalities in an Alzheimer model.
Researchers at the Gladstone Institutes have shown that low levels of the protein progranulin in the brain can increase the formation of amyloid-beta plaques (a hallmark of Alzheimer’s disease), cause neuroinflammation, and worsen memory deficits in a mouse model of this condition. Conversely, by using a gene therapy approach to elevate progranulin levels, scientists were able to prevent these abnormalities and block cell death in this model.
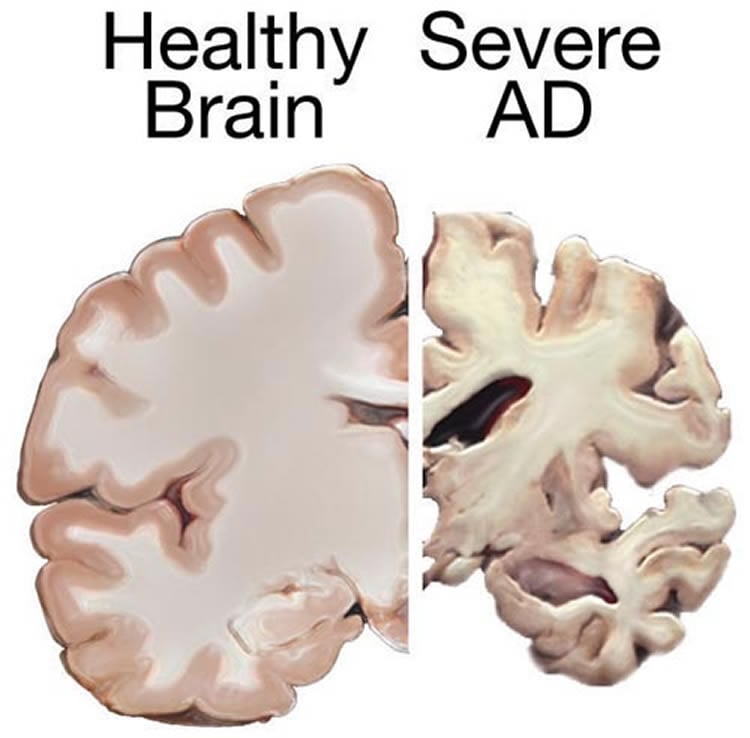
Progranulin deficiency is known to cause another neurodegenerative disorder, frontotemporal dementia (FTD), but its role in Alzheimer’s disease was previously unclear. Although the two conditions are similar, FTD is associated with greater injury to cells in the frontal cortex, causing behavioral and personality changes, whereas Alzheimer’s disease predominantly affects memory centers in the hippocampus and temporal cortex.
Earlier research showed that progranulin levels were elevated near plaques in the brains of patients with Alzheimer’s disease, but it was unknown whether this effect counteracted or exacerbated neurodegeneration. The new evidence, published today in Nature Medicine, shows that a reduction of the protein can severely aggravate symptoms, while increases in progranulin may be the brain’s attempt at fighting the inflammation associated with the disease.
According to first author S. Sakura Minami, PhD, a postdoctoral fellow at the Gladstone Institutes, “This is the first study providing evidence for a protective role of progranulin in Alzheimer’s disease. Prior research had shown a link between Alzheimer’s and progranulin, but the nature of the association was unclear. Our study demonstrates that progranulin deficiency may promote Alzheimer’s disease, with decreased levels rendering the brain vulnerable to amyloid-beta toxicity.”
In the study, the researchers manipulated several different mouse models of Alzheimer’s disease, genetically raising or lowering their progranulin levels. Reducing progranulin markedly increased amyloid-beta plaque deposits in the brain as well as memory impairments. Progranulin deficiency also triggered an over-active immune response in the brain, which can contribute to neurological disorders. In contrast, increasing progranulin levels via gene therapy effectively lowered amyloid beta levels, protecting against cell toxicity and reversing the cognitive deficits typically seen in these Alzheimer’s models.
These effects appear to be linked to progranulin’s involvement in phagocytosis, a type of cellular house-keeping whereby cells “eat” other dead cells, debris, and large molecules. Low levels of progranulin can impair this process, leading to increased amyloid beta deposition. Conversely, increasing progranulin levels enhanced phagocytosis, decreasing the plaque load and preventing neuron death.
“The profound protective effects of progranulin against both amyloid-beta deposits and cell toxicity have important therapeutic implications,” said senior author Li Gan, PhD, an associate investigator at Gladstone and associate professor of neurology at the University of California, San Francisco. “The next step will be to develop progranulin-enhancing approaches that can be used as potential novel treatments, not only for frontotemporal dementia, but also for Alzheimer’s disease.”
Other authors on the study include Sang-Won Min, Grietje Krabbe, Chao Wang, Yungui Zhou, Rustam Asgarov, Yaqiao Li, Lauren Martens, Lisa Elia, Michael Ward, Lennart Mucke, and Robert Farese. Funding for the research was provided by the Consortium for Frontotemporal Dementia, National Institutes of Health, and the S. D. Bechtel, Jr. Foundation.
Contact: Dana Smith – Gladstone Institute
Source: Gladstone Institute press release
Image Source: The image is credited to the NIH and is in the public domain
Original Research: Abstract for “Progranulin protects against amyloid β deposition and toxicity in Alzheimer’s disease mouse models” by S Sakura Minami, Sang-Won Min, Grietje Krabbe, Chao Wang, Yungui Zhou, Rustam Asgarov, Yaqiao Li, Lauren H Martens, Lisa P Elia, Michael E Ward, Lennart Mucke, Robert V Farese Jr and Li Gan in Nature Medicine. Published online September 28 2014 doi:10.1038/nm.3672






