Summary: According to researchers, a simple MRI brain scan could help diagnose people with a common cognitive disorder.
Source: RSNA.
Brain MRI could help improve the diagnosis of people with a common type of cognitive disorder, according to a new study published online in the journal Radiology.
Vascular cognitive disorder is caused by disease of the vessels supplying blood to the brain. Strokes and transient ischemic attacks, or ministrokes, are risk factors. The resulting loss of healthy brain tissue adversely affects concentration and decision making and leads to problems with planning and organizing. Prevalence of vascular cognitive disorder is increasing in the elderly, and it can be challenging to diagnose and differentiate from other forms of dementia like Alzheimer’s disease.
“If vascular cognitive disorder follows a major stroke, the cognitive impairment typically develops suddenly, and can thus be well recognized,” said study co-author Dewen Meng, M.Sc., from the University of Nottingham in Nottingham, England. “In the majority of cases such a clear association is lacking, explaining why the detection of vascular cognitive disorder remains challenging.”

A biomarker that could predict and track vascular cognitive disorder on imaging exams has yet to be found, although MRI measurements of the brain’s signal-carrying white matter are a promising area of research. Damage to the white matter can be assessed with diffusion tensor imaging, an MRI technique that provides two important measures of microscopic brain damage: mean diffusivity and fractional anisotropy. Increased mean diffusivity, which measures the movement of water through tissue, is particularly sensitive to the breakdown of nerve fibers in the brain and the protective coating around them.
For the new study, researchers assessed brain MRI and cognitive examination results from 108 patients with symptomatic carotid artery disease, a risk factor for vascular cognitive disorder. Of the 108 patients, 53 were cognitively impaired. Further analysis showed a clear correlation between cognitive performance and the presence of chronic vascular disease-related lesions within certain white matter tracts of the brain. White matter tract skeleton mean diffusivity showed the closest correlation with impaired cognitive performance, making it a promising tool for improved diagnostic accuracy of vascular cognitive disorder.
“Using standard clinical brain MRI, we found that microscopic damage of main white matter tracts allowed us to distinguish patients with symptomatic carotid artery disease and cognitive impairment from those who were cognitively intact,” said the study’s senior author, Dorothee P. Auer, Ph.D., from the University of Nottingham. “Our findings mean that a simple MRI test might improve the diagnostic work-up of people with suspected vascular cognitive disorder, and holds further promise to track progression of the disorder.”
The results suggest that a key mechanism of vascular cognitive disorder is subcortical disconnection, a kind of breakdown of communication within the large-scale cognitive neural networks.
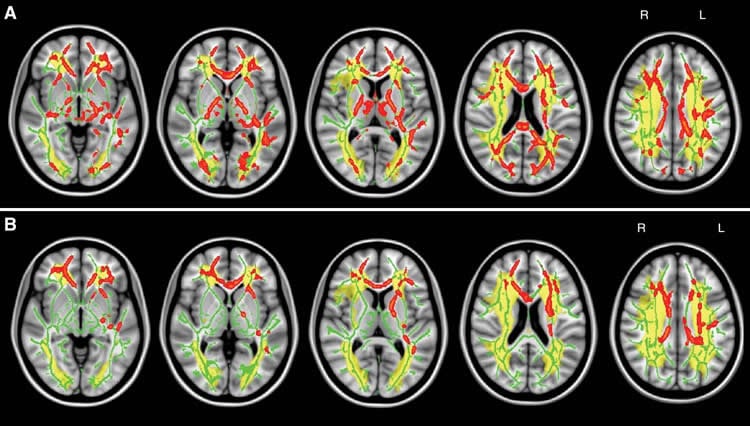
Dr. Auer explained that the brain is functionally organized into networks that require efficient communication across specific brain regions. This communication depends on the information flow between the network nodes, not unlike the flow of passenger traffic through an extensive urban subway system. Subcortical disconnection suggests a disruption in connections between such cognitive nodes, impairing information flow and thus network coordination.
“The analogy would be a construction site at one of the main subway lines causing traffic disruptions,” Dr. Auer said.
The researchers plan to expand their studies and look at changes in patients over time to see if they can track the progression of subcortical disconnection.
“This will be a critical step in the quest for prevention of vascular dementia, by helping to identify those at risk, and by enabling imaging studies to evaluate the effectiveness of interventions,” Meng said.
Funding: This work was supported by theNational Institute for Health Research.
Source: Linda Brooks – RSNA
Image Source: NeuroscienceNews.com images are credited to RSNA.
Original Research: Full open access research for “Lesion Topography and Microscopic White Matter Tract Damage Contribute to Cognitive Impairment in Symptomatic Carotid Artery Disease” by Dewen Meng, Akram A. Hosseini, Richard J. Simpson, Quratulain Shaikh, Christopher R. Tench, Robert A. Dineen, and Dorothee P. Auer in Radiology. Published online September 6 2016 doi:10.1148/radiol.2016152685
[cbtabs][cbtab title=”MLA”]RSNA “‘Traffic Jam’ in Brain Linked to Common Cognitive Disorder.” NeuroscienceNews. NeuroscienceNews, 6 September 2016.
<https://neurosciencenews.com/neurology-vascular-cognitive-disorder-4970/>.[/cbtab][cbtab title=”APA”]RSNA (2016, September 6). ‘Traffic Jam’ in Brain Linked to Common Cognitive Disorder. NeuroscienceNew. Retrieved September 6, 2016 from https://neurosciencenews.com/neurology-vascular-cognitive-disorder-4970/[/cbtab][cbtab title=”Chicago”]RSNA “‘Traffic Jam’ in Brain Linked to Common Cognitive Disorder.” https://neurosciencenews.com/neurology-vascular-cognitive-disorder-4970/ (accessed September 6, 2016).[/cbtab][/cbtabs]
Abstract
Lesion Topography and Microscopic White Matter Tract Damage Contribute to Cognitive Impairment in Symptomatic Carotid Artery Disease
Purpose
To investigate associations between neuroimaging markers of cerebrovascular disease, including lesion topography and extent and severity of strategic and global cerebral tissue injury, and cognition in carotid artery disease (CAD).
Materials and Methods
All participants gave written informed consent to undergo brain magnetic resonance imaging and the Addenbrooke’s Cognitive Examination–Revised. One hundred eight patients with symptomatic CAD but no dementia were included, and a score less than 82 represented cognitive impairment. Group comparison and interrelations between global cognitive and fluency performance, lesion topography, and ultrastructural damage were assessed with voxel-based statistics. Associations between cognition, medial temporal lobe atrophy (MTA), lesion volumes, and global white matter ultrastructural damage indexed as increased mean diffusivity were tested with regression analysis by controlling for age. Diagnostic accuracy of imaging markers selected from a multivariate prediction model was tested with receiver operating characteristic analysis.
Results
Cognitively impaired patients (n = 53 [49.1%], classified as having probable vascular cognitive disorder) were older than nonimpaired patients (P = .027) and had more frequent MTA (P < .001), more cortical infarctions (P = .016), and larger volumes of acute (P = .028) and chronic (P = .009) subcortical ischemic lesions. Lesion volumes did not correlate with global cognitive performance (lacunar infarctions, P = .060; acute lesions, P = .088; chronic subcortical ischemic lesions, P = .085). In contrast, cognitive performance correlated with presence of chronic ischemic lesions within the interhemispheric tracts and thalamic radiation (P < .05, false discovery rate corrected). Skeleton mean diffusivity showed the closest correlation with cognition (R2 = 0.311, P < .001) and promising diagnostic accuracy for vascular cognitive disorder (area under the curve, 0.82 [95% confidence interval: 0.75, 0.90]). Findings were confirmed in subjects with a low risk of preclinical Alzheimer disease indexed by the absence of MTA (n = 85).
Conclusion
Subcortical white matter ischemic lesion locations and severity of ultrastructural tract damage contribute to cognitive impairment in symptomatic CAD, which suggests that subcortical disconnection within large-scale cognitive neural networks is a key mechanism of vascular cognitive disorder.
“Lesion Topography and Microscopic White Matter Tract Damage Contribute to Cognitive Impairment in Symptomatic Carotid Artery Disease” by Dewen Meng, Akram A. Hosseini, Richard J. Simpson, Quratulain Shaikh, Christopher R. Tench, Robert A. Dineen, and Dorothee P. Auer in Radiology. Published online September 6 2016 doi:10.1148/radiol.2016152685






