Summary: Researchers document the effects of ketamine overdose in a 10 month old infant.
Source: Journal of Neurosurgery Publishing Group.
Perhaps the saddest drug abuse stories are about unsuspecting children who inadvertently ingest dangerous substances in the home. Fortunately, the case described in this report has a happy ending due to fast action on the part of the response team and pediatric emergency physicians and neurosurgeons. Detailed information on the case can be found in the article, “Severe bilateral cerebellar edema from ingestion of ketamine: case report,” by Nicolas Villelli, MD, and colleagues, published today in the Journal of Neurosurgery: Pediatrics.
Ketamine is a medical drug administered to humans (including children) and animals to induce sedation and anesthesia. Its euphoric and dissociative side effects have made it attractive to people seeking recreational drug highs. A ketamine overdose can have serious consequences, and the drug has been implicated in deaths–some due to physiological responses to the drug alone and some caused by risky behaviors brought on by the drugged state.
The authors recount the case of a 10-month-old baby girl who was found in an unresponsive state along with her brother and grandmother. Initially, carbon monoxide poisoning was believed to be responsible. Not until later did the police determine that all victims had eaten from dishes previously used to soak tobacco leaves in ketamine for use as a recreational drug known as “Kommon.”
The child vomited after eating eggs from her dish and went to sleep. She was later found unresponsive by a family member who called for emergency services. At the hospital, it was necessary to use emergency intubation and ventilation for the child’s poor breathing. She was minimally responsive and displayed abnormally high muscle tone.
Imaging studies revealed severe swelling in the cerebellar hemispheres. This was blocking the normal flow of cerebrospinal fluid, causing a situation that could be rapidly fatal. The upper part of the brain seemed spared from damage. This set of findings was unusual, because most of the time the upper part of the brain is damaged from lack of oxygen and the cerebellum is spared. This reversal of the expected findings suggested a specific association with the drug that was ingested.
The patient received emergency placement of a drain to divert the spinal fluid, followed by surgical decompression to allow more room for the swelling and to reduce the pressure on the brain.
The patient’s neurological condition slowly improved, and artificial ventilation was removed six days postoperatively. At two weeks postoperatively, the infant was able to participate in rehabilitation exercises and the external ventricular drain was replaced with a cerebrospinal fluid shunt. Six months after the injury, although imaging studies showed permanent damage to the cerebellum, the child’s clinical recovery was remarkable. Her muscle coordination was normal and, other than a slight speech delay, she was meeting all appropriate developmental milestones.
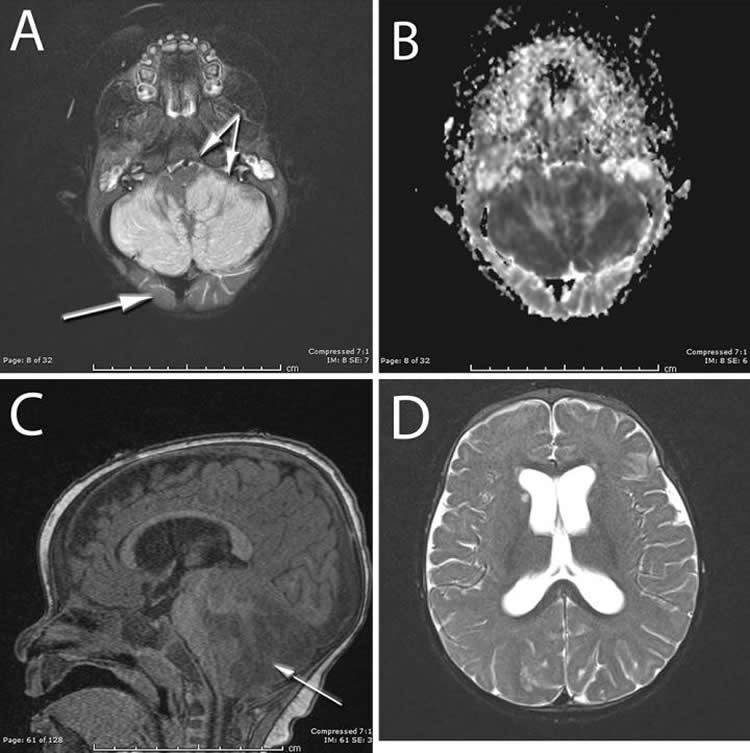
Prior to this case report not much was known about the pediatric brain’s reaction to a ketamine overdose. The importance of this paper lies in the detailed description of the patient’s clinical features and the unexpected imaging findings.
In discussing the findings of this study, the corresponding author, Dr. Daniel H. Fulkerson, MD, provided the following comment:
“We are very excited that the child has recovered well following this life-threatening event. Unfortunately, we fear that cases like this will continue to occur, as we have seen a dangerous rise in drug use in our state and in the nation. Innocent kids are often affected. We hope this case shines some light on this particular exposure and helps other medical facilities recognize these unique findings.”
The authors report no conflict of interest concerning the materials or methods used in this study or the findings specified in this paper.
Source: Jo Ann M. Eliason – Journal of Neurosurgery Publishing Group
Image Source: NeuroscienceNews.com image is credited to AANS.
Original Research: Full open access research for “Severe bilateral cerebellar edema from ingestion of ketamine: case report” by Nicolas Villelli, MD, Natalie Hauser, NP, Thomas Gianaris, MD, Blake A. Froberg, MD, and Daniel H. Fulkerson, MD in Journal of Neurosurgery. Published online August 15 2017 doi:10.3171/2017.5.PEDS16695
[cbtabs][cbtab title=”MLA”]Journal of Neurosurgery Publishing Group”Clinical Appearance and Unusual Imaging Findings of Pediatric Ketamine Overdose.” NeuroscienceNews. NeuroscienceNews, 15 August 2017.
<https://neurosciencenews.com/neuroimaging-ketamine-overdose-7312/>.[/cbtab][cbtab title=”APA”]Journal of Neurosurgery Publishing Group(2017, August 15). Clinical Appearance and Unusual Imaging Findings of Pediatric Ketamine Overdose. NeuroscienceNew. Retrieved August 15, 2017 from https://neurosciencenews.com/neuroimaging-ketamine-overdose-7312/[/cbtab][cbtab title=”Chicago”]Journal of Neurosurgery Publishing Group”Clinical Appearance and Unusual Imaging Findings of Pediatric Ketamine Overdose.” https://neurosciencenews.com/neuroimaging-ketamine-overdose-7312/ (accessed August 15, 2017).[/cbtab][/cbtabs]
Abstract
Severe bilateral cerebellar edema from ingestion of ketamine: case report
The use of ketamine as a drug of abuse has increased and so too has the risk of accidental overdose. Here, the authors report the case of a 10-month-old infant who inadvertently ingested ketamine. The child demonstrated severe cerebellar swelling that required emergency surgical intervention. The authors describe the clinical course of this child and present the radiographic characteristics of the brain. The imaging characteristics were not consistent with purely anoxic injury, thus suggesting a specific effect of this drug. To the authors’ knowledge, similar imaging characteristics in this context have not been described.
“Severe bilateral cerebellar edema from ingestion of ketamine: case report” by Nicolas Villelli, MD, Natalie Hauser, NP, Thomas Gianaris, MD, Blake A. Froberg, MD, and Daniel H. Fulkerson, MD in Journal of Neurosurgery. Published online August 15 2017 doi:10.3171/2017.5.PEDS16695






