Summary: Anosmia, the loss of the sense of smell which is a common symptom of COVID-19, may be a secondary consequence of immune system inflammation rather than a direct action of the virus.
Source: Johns Hopkins Medicine
Anosmia, the loss of smell, is a frequent and often long-term symptom associated with COVID-19 that can severely burden a person’s quality of life, making it extremely difficult to taste foods, detect airborne hazards in the environment and carry out other functions dependent on the sense.
While the devastating impacts of COVID-mediated anosmia are well known, the biological mechanisms underlying the condition remain somewhat of a mystery.
In a study published today in JAMA Neurology, a Johns Hopkins Medicine-led team shows that loss of smell is most likely a secondary consequence of inflammation occurring when the body’s immune system responds to SARS-CoV-2 infection rather than a direct action of the virus.
“As a neuropathologist, I wondered why smell loss is a very common symptom with COVID-19 but not with other respiratory diseases,” says study lead author Cheng-Ying Ho, M.D., Ph.D., associate professor of pathology at the Johns Hopkins University School of Medicine.
“So, we decided to dig deeply into the mechanics of smell to see what actually occurs at the cellular level when SARS-CoV-2 invades the body.”
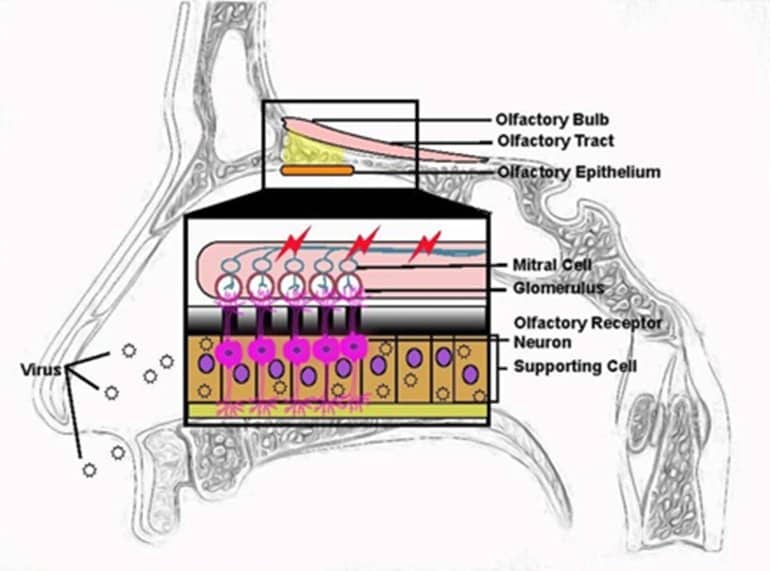
To conduct their investigation, Ho and her colleagues collected tissues from the olfactory bulb at the base of the brain—a region that transmits nerve impulses carrying information about odors—of 23 persons who died from COVID-19 and a control group of 14 who died from other causes and who had no detectable SARS-CoV-2 at the time of their deaths.
All of the tissues were evaluated for any detectable SARS-CoV-2 particles; the structure and characteristics of the cells, blood vessels and neurons (nerve cells) within them, using both light and electron microscopy; and the number of axons (the portions of neurons that transmit electrical impulses) present. Information about sense of smell and taste was obtained from clinical records for three patients and from family interviews for the rest.
Three of the 23 patients with COVID-19 were determined to have lost their sense of smell, four had diminished ability to smell and two had loss of both smell and taste. None of the 14 patients in the control group were identified as having lost either smell or taste.
The researchers wanted to learn three things from their study of the two groups: the levels of degeneration (damage) to the neurons in the olfactory system, the amount of olfactory axons lost and the severity of microvasculopathy (disease of the small blood vessels). What they found, Ho says, was not unexpected.
“When we compared the tissues from patients without COVID-19 with those from persons who had been infected with SARS-CoV-2—especially the ones with diminished or complete loss of smell—we found that the group with COVID showed more severe vascular injury and far fewer axons in the olfactory bulb,” says Ho.
“And that didn’t change when we statistically controlled for the impact of age, strongly suggesting that these effects aren’t age-related and therefore, are linked to SARS-CoV-2 infection.”
However, Ho says the researchers were surprised by the study’s other major finding—that despite nerve and vascular damage, SARS-CoV-2 particles were not detected in the olfactory bulb in the majority of patients with COVID-19.
“Previous investigations that only relied on routine pathological examinations of tissue—and not the in-depth and ultrafine analyses we conducted—surmised that viral infection of the olfactory neurons and olfactory bulb might play a role in loss of smell associated with COVID-19,” she explains.
“But our findings suggest that SARS-CoV-2 infection of the olfactory epithelium leads to inflammation, which in turn, damages the neurons, reduces the numbers of axons available to send signals to the brain and results in the olfactory bulb becoming dysfunctional.”
The researchers next plan to do a follow-up study on tissues taken from patients who died of the SARS-CoV-2 Delta and Omicron variants.
“We want to compare any axon damage and bulb dysfunction found in those tissues with what we observed in patients who had the original virus strain,” says Ho. “That way, we’ll be able to better predict if Delta and Omicron are more or less likely to cause loss of smell.”
About this inflammation and COVID-19 research news
Author: Press Office
Source: Johns Hopkins Medicine
Contact: Press Office – Johns Hopkins Medicine
Image: The image is credited to Cheng-Ying Ho, Johns Hopkins Medicine
Original Research: Open access.
“Postmortem Assessment of Olfactory Tissue Degeneration and Microvasculopathy in Patients With COVID-19” by Cheng-Ying Ho et al. JAMA Neurology
Abstract
Postmortem Assessment of Olfactory Tissue Degeneration and Microvasculopathy in Patients With COVID-19
Importance
Loss of smell is an early and common presentation of COVID-19 infection. Although it has been speculated that viral infection of olfactory neurons may be the culprit, it is unclear whether viral infection causes injuries in the olfactory bulb region.
Objective
To characterize the olfactory pathology associated with COVID-19 infection in a postmortem study.
Design, Setting, and Participants
This multicenter postmortem cohort study was conducted from April 7, 2020, to September 11, 2021. Deceased patients with COVID-19 and control individuals were included in the cohort. One infant with congenital anomalies was excluded. Olfactory bulb and tract tissue was collected from deceased patients with COVID-19 and appropriate controls. Histopathology, electron microscopy, droplet digital polymerase chain reaction, and immunofluorescence/immunohistochemistry studies were performed. Data analysis was conducted from February 7 to October 19, 2021.
Main Outcomes and Measures
(1) Severity of degeneration, (2) losses of olfactory axons, and (3) severity of microvasculopathy in olfactory tissue.
Results
Olfactory tissue from 23 deceased patients with COVID-19 (median [IQR] age, 62 [49-69] years; 14 men [60.9%]) and 14 control individuals (median [IQR] age, 53.5 [33.25-65] years; 7 men [50%]) was included in the analysis.
The mean (SD) axon pathology score (range, 1-3) was 1.921 (0.569) in patients with COVID-19 and 1.198 (0.208) in controls (P < .001), whereas axon density was 2.973 (0.963) × 104/mm2 in patients with COVID-19 and 3.867 (0.670) × 104/mm2 in controls (P = .002). Concomitant endothelial injury of the microvasculature was also noted in olfactory tissue. The mean (SD) microvasculopathy score (range, 1-3) was 1.907 (0.490) in patients with COVID-19 and 1.405 (0.233) in control individuals (P < .001).
Both the axon and microvascular pathology was worse in patients with COVID-19 with smell alterations than those with intact smell (mean [SD] axon pathology score, 2.260 [0.457] vs 1.63 [0.426]; P = .002; mean [SD] microvasculopathy score, 2.154 [0.528] vs 1.694 [0.329]; P = .02) but was not associated with clinical severity, timing of infection, or presence of virus.
Conclusions and Relevance
This study found that COVID-19 infection is associated with axon injuries and microvasculopathy in olfactory tissue. The striking axonal pathology in some cases indicates that olfactory dysfunction in COVID-19 infection may be severe and permanent.







