Post-traumatic stress disorder (PTSD) doubles risk of future cardiac event and death.
One in eight people who suffer a heart attack or other acute coronary event experience clinically significant symptoms of post-traumatic stress disorder (PTSD), according to a meta-analysis of 24 studies led by Columbia University Medical Center researchers. The study also shows that heart patients who suffer PTSD face twice the risk of having another cardiac event or of dying within one to three years, compared with those without PTSD. The findings were published today in the online edition of PLoS ONE.
“While most people think of PTSD as a disorder of combat veterans and sexual assault survivors, it is also quite common among patients who have had a severe coronary event,” said lead author Donald Edmondson, PhD, assistant professor of behavioral medicine at CUMC. “Not only are such events life-threatening, but their psychological impact can be devastating and long lasting.”
PTSD is an anxiety disorder initiated by exposure to a traumatic event such as combat, disaster, or sexual assault. Common symptoms include nightmares, avoidance of reminders of the event, and elevated heart rate and blood pressure.
Each year, about 1.4 million people in the United States experience an acute coronary syndrome (ACS), a term used to describe any condition brought about by sudden reduced blood flow to the heart. Numerous small studies have suggested that ACS-induced PTSD is common and can have serious health consequences, but its prevalence is not known.
To get a better idea of the scope of the problem, Dr. Edmondson and his colleagues performed the first combined review, or meta-analysis, of clinical studies of ACS-induced PTSD. The 24 studies in the meta-analysis included a total of 2,383 ACS patients from around the globe.
The study found that overall 12 percent, or one in eight, of the patients developed clinically significant PTSD symptoms, with four percent meeting full diagnostic criteria for the disorder.
“Given that some 1.4 million ACS patients are discharged from U.S. hospitals each year, our results suggest that 168,000 patients will develop clinically significant PTSD symptoms. That is quite substantial. However, there is abundant evidence that psychological disorders in heart patients are underrecognized and undertreated. In fact, underdiagnosis may be even more pronounced in cardiac practices than in other types of medical practices,” said Dr. Edmondson.
“This is a serious problem for individual patients, as well as for the healthcare system as a whole,” he said. “PTSD appears to double a heart patient’s risk for a second cardiac event and for death, which adds hundreds of millions of dollars to annual health expenditures.”
“Fortunately, there are good treatments for people with PTSD,” Dr. Edmondson said. “But first, physicians and patients have to be aware that this is a problem. Family members can also help. We know that social support is a good protective factor against PTSD due to any type of traumatic event.”
“The next step is further research to assess whether treatment can reduce ACS-induced PTSD symptoms and reduce the associated risk for ACS recurrence and mortality,” said Dr. Edmondson.
Dr. Edmondson’s paper is titled, “Posttraumatic stress disorder induced by acute coronary syndrome: A meta-analytic review of prevalence and associated clinical outcomes.” The other contributors are Safiya Richardson (CUMC), Louise Falzon (CUMC), Karina W. Davidson (CUMC), Mary Alice Mills (VA Boston Healthcare System), and Yuval Neria (CUMC).
This research was supported by National Institutes of Health (NIH) grants HL-088117 and CA-156709. It was supported in part by Columbia University’s Clinical and Translational Science Awards (CTSA) grant No. UL1RR024156 from the National Center for Advancing Translational Sciences – National Center for Research Resources/NIH. Dr. Edmondson is supported by NIH grant KM1CA156709.
The authors declare no financial or other conflicts of interest.
Contact: Elizabeth Streich – Columbia University Medical Center
Source: Columbia University Medical Center press release
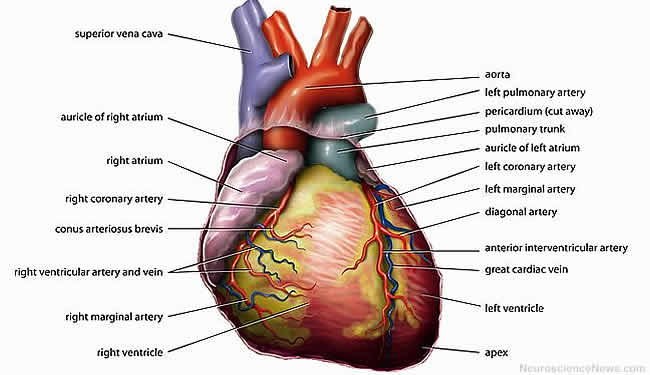
Image Source: Neuroscience News image adapted from public domain image. Feel free to use.
Original Research: Full open access research paper for “Posttraumatic Stress Disorder Prevalence and Risk of Recurrence in Acute Coronary Syndrome Patients: A Meta-analytic Review” by Donald Edmondson, Safiya Richardson, Louise Falzon, Karina W. Davidson, Mary Alice Mills and Yuval Neria in PLoS ONE 2012 7(6): e38915. doi:10.1371/journal.pone.0038915







