In a cutting-edge treatment for Alzheimer’s disease, EPFL scientists have developed an implantable capsule that can turn the patient’s immune system against the disease.
One of the hypothesized causes of Alzheimer’s is the over-accumulation of the protein amyloid beta (Abeta) in different areas of the brain. This results in the deposition of aggregated protein plaques, which are toxic to neurons. One of the most promising ways to fight the plaques is to “tag” the Abeta proteins with antibodies that signal the patient’s own immune system to attack and clear them. To be most effective, this treatment has to be given as early as possible, before the first signs of cognitive decline. But this requires repeated vaccine injections, which can cause side effects. EPFL scientists have now solved the problem with an implant that can deliver a steady and safe flow of antibodies to the patient’s brain to clear Abeta proteins. The work is published in the journal Brain.
The lab of Patrick Aebischer at EPFL has developed a bioactive capsule containing cells that have been genetically engineered to produce antibodies against Abeta. The capsule is implanted in the tissue under the skin, and over time the cells produce and release a steady flow of antibodies into the bloodstream, from where they cross over into the brain to target the Abeta plaques.
The capsule itself is based on a design from Aebischer’s lab published in 2014. It is referred to as a “macroencapsulation device” and it is made of two permeable membranes sealed together with a polypropylene frame. The completed device is 27-mm long, 12-mm wide and 1.2-mm thick, and contains a hydrogel that facilitates cell growth. All the materials used are biocompatible, and the lab specifically used a method that is easily reproducible for large-scale manufacturing.
The cells inside the capsule are important. Not only must they be able to produce antibodies, but they also have to be compatible with the patient, so as to not trigger the immune system against them, like a transplant can. This is where the capsule’s membranes come into play, shielding the cells from being identified and attacked by the immune system. This protection also means that cells from a single donor can be used on multiple patients.
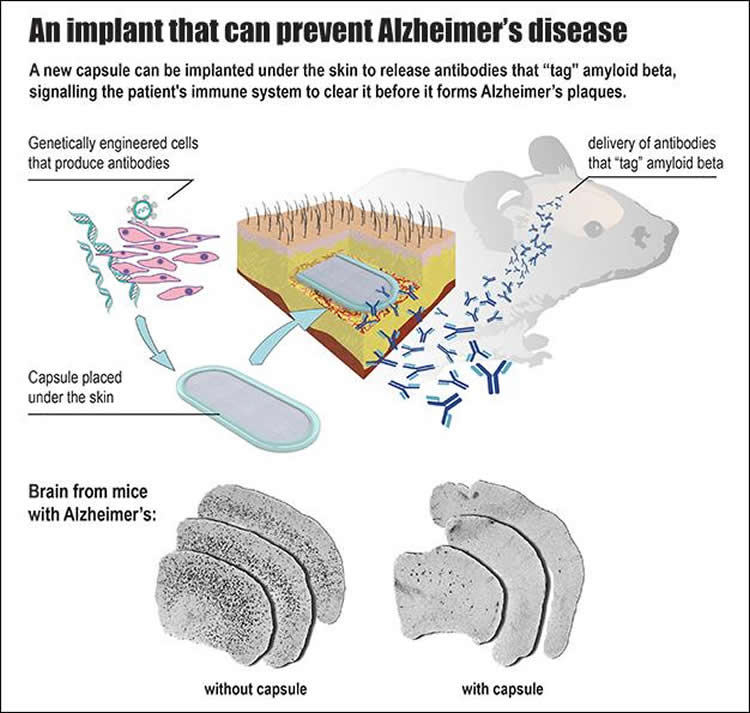
Before going into capsule, the cells are first genetically engineered to produce antibodies that specifically recognize and target Abeta. The cells of choice are taken from muscle tissue, and the permeable membranes let them interact with the surrounding tissue to get all the nutrients and molecules they need.
The researchers tested the device on mice with great success. The mice – a genetic line that is commonly used to simulate Alzheimer’s disease – showed dramatic reduction of Abeta plaque load. Indeed, the constant flow of antibodies produced by the capsule over a course of 39 weeks prevented the formation of Abeta plaques in the brain. The treatment also reduced the phosphorylation of the protein tau, another sign of Alzheimer’s observed in these mice.
The proof-of-concept work is a landmark. It demonstrates clearly that encapsulated cell implants can be used successfully and safely to deliver antibodies to treat Alzheimer’s disease and other neurodegenerative disorders that feature defective proteins.
Funding: This work involved a collaboration between EPFL’s Neurodegenerative Studies Laboratory (Brain Mind Institute), the Swiss Light Source (Paul Scherrer Institute) and F. Hoffmann-La Roche. It was funded by the Swiss Commission for Technology and Innovation and F. Hoffmann-La Roche Ltd.
Source: Nik Papageorgiou – EPFL
Image Source: The image is credited to Patrick Aebischer (EPFL).
Original Research: Abstract for “A subcutaneous cellular implant for passive immunization against amyloid-β reduces brain amyloid and tau pathologies” by Aurélien Lathuilière, Vanessa Laversenne, Alberto Astolfo, Erhard Kopetzki, Helmut Jacobsen, Marco Stampanoni, Bernd Bohrmann, Bernard L. Schneider, and Patrick Aebischer in Brain. Published online March 8 2016 doi:10.1093/brain/aww036
Abstract
A subcutaneous cellular implant for passive immunization against amyloid-β reduces brain amyloid and tau pathologies
Passive immunization against misfolded toxic proteins is a promising approach to treat neurodegenerative disorders. For effective immunotherapy against Alzheimer’s disease, recent clinical data indicate that monoclonal antibodies directed against the amyloid-β peptide should be administered before the onset of symptoms associated with irreversible brain damage. It is therefore critical to develop technologies for continuous antibody delivery applicable to disease prevention. Here, we addressed this question using a bioactive cellular implant to deliver recombinant anti-amyloid-β antibodies in the subcutaneous tissue. An encapsulating device permeable to macromolecules supports the long-term survival of myogenic cells over more than 10 months in immunocompetent allogeneic recipients. The encapsulated cells are genetically engineered to secrete high levels of anti-amyloid-β antibodies. Peripheral implantation leads to continuous antibody delivery to reach plasma levels that exceed 50 µg/ml. In a proof-of-concept study, we show that the recombinant antibodies produced by this system penetrate the brain and bind amyloid plaques in two mouse models of the Alzheimer’s pathology. When encapsulated cells are implanted before the onset of amyloid plaque deposition in TauPS2APP mice, chronic exposure to anti-amyloid-β antibodies dramatically reduces amyloid-β40 and amyloid-β42 levels in the brain, decreases amyloid plaque burden, and most notably, prevents phospho-tau pathology in the hippocampus. These results support the use of encapsulated cell implants for passive immunotherapy against the misfolded proteins, which accumulate in Alzheimer’s disease and other neurodegenerative disorders.
“A subcutaneous cellular implant for passive immunization against amyloid-β reduces brain amyloid and tau pathologies” by Aurélien Lathuilière, Vanessa Laversenne, Alberto Astolfo, Erhard Kopetzki, Helmut Jacobsen, Marco Stampanoni, Bernd Bohrmann, Bernard L. Schneider, and Patrick Aebischer in Brain. Published online March 8 2016 doi:10.1093/brain/aww036