Summary: Neuroimaging study ties the degradation of circuitry in one area of the brain to reduced efficiency of executive function in older adults.
Source: UT Dallas
As the human brain ages, the neural circuits that allow its different parts to communicate with each other gradually wear down, even in healthy adults.
Scientists at The University of Texas at Dallas are using imaging techniques to investigate this process to understand better how it relates to cognitive decline in healthy individuals across the lifespan.
“We’re trying to figure out what’s breaking down in the brain that yields this cognitive decline as we get older, even if we’re healthy,” said Dr. Kristen Kennedy, associate professor of psychology in the School of Behavioral and Brain Sciences and in UT Dallas’ Center for Vital Longevity. “Everything we do in our lab is adding pieces to that puzzle.”
In a study published online June 7 and in the October issue of Neurobiology of Aging, principal investigator Kennedy and her colleagues describe how they used a pair of imaging techniques to tie the degradation of circuitry in one region of the brain to reduced efficiency in executive functions. The study included 169 healthy human subjects between the ages of 20 and 94.
On a basic level, the brain consists of regions of gray matter that are interconnected by white matter. Composed primarily of neuronal cell bodies, gray matter is the center of activity, from higher learning and memory to sensory reception and muscular responses. White matter consists mainly of myelinated axons, the part of neurons that relay signals to and from gray matter regions.
Dr. Christina Webb, lead author of the study and a research associate in Kennedy’s lab, said that the evolving research on white matter shows that its ability to propagate signals strongly affects cognition and higher-order processing.
“More and more, research shows us that the structure of the brain affects its function, especially in terms of aging and white matter,” she said. “In earlier work, we’ve shown this effect more broadly across white matter networks. Here, we’re tying it more specifically to the frontostriatal white matter networks, which we know are linked to higher-order executive function.”
Kennedy said that when the brain is confronted with a challenging task, it has to “ramp up” its activity, and that the amount needed changes across the lifespan.
“This research shows that you don’t ramp up the output of your gray matter regions as well when you’re older,” she said. “One reason is that the white matter connections have degraded. The electrical transmission between neurons is not as intact.”
The research team used two different imaging techniques to examine how white matter connections lose integrity, as well as how this affects cognition in people of different ages.
One of the techniques, diffusion tensor imaging, measures the directionality of water diffusion in the brain. Webb compared the ideal performance to water moving through a straw.
“If the water is constrained on this path, this represents faster information processing,” she said. “If water is very diffuse, flowing freely, that can slow down communication efficiency between neurons. So we’re measuring the effectiveness of structural connectivity.”
The scientists combined this insight with functional MRI (fMRI), which Kennedy described as “a dynamic, moment-to-moment look at what the brain is doing in real time.”
“While the other scans are structural, the fMRI scans — taken while subjects are performing a task — allow us to see what resources the brain is using by tracking blood-oxygen levels,” she said.
With these two sets of metrics, the researchers could predict cognitive performance and then compare expectations to how the subjects actually performed.
“While this doesn’t examine causality, this technique can be used to test hypotheses, which are based on our knowledge of how we think the brain works,” Kennedy said. “Our theory is that age directly degrades the white matter, and this in turn results in a failure of the gray matter to fully ramp up. The result is a detrimental effect on cognition.”
Kennedy’s work is part of a trend toward studying healthy neurological aging as much as pathological conditions, which were much more thoroughly studied through the end of the 20th century.
“There’s been an increasing feeling that it can only help us so much to understand these handful of diseases versus understanding how people ideally age,” she said. “That baseline is needed to better understand, by comparison, any disease.”
The researchers have continued to collect new data from the study’s cohort since the original measurements were obtained four years ago. They plan to address some larger questions of aging via a forthcoming longitudinal study, which will compare data from the same people at two different points in time.
“Maybe we can capitalize on seeing what’s happening very early, when everyone’s healthy and normal, and determine when that changes, or to help define a path toward pathology,” Webb said. “We see differences early in the lifespan with this group. Seeing what’s happening early in the lifespan, and with the longitudinal data coming in, will hopefully help us determine if these people are already on different paths.”
Additional contributors to the study included Dr. Karen Rodrigue, associate professor of psychology, and cognition and neuroscience doctoral student David Hoagey.
Funding:This work was supported in part by National Institute on Aging grants 5R00AG036848-05, 5R00AG036818 and 5R01AG056535-04.
About this brain plasticity research article
Source:
Garvan Institute of Medical Research
Contacts:
Press Office – UT Dallas
Image Source:
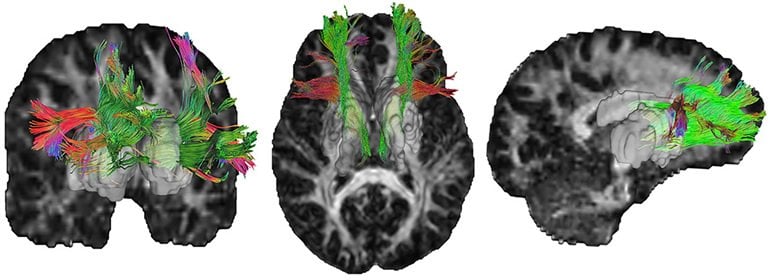
The image is credited to the researchers.
Original Research: Closed access
“Frontostriatal white matter connectivity: age differences and associations with cognition and BOLD modulation” by Kristen Kennedy et al. Neurobiology of Aging.
Abstract
Frontostriatal white matter connectivity: age differences and associations with cognition and BOLD modulation
Despite the importance of cortico-striatal circuits to cognition, investigation of age effects on the structural circuitry connecting these regions is limited. The current study examined age effects on frontostriatal white matter connectivity, and identified associations with both executive function performance and dynamic modulation of blood-oxygen-level-dependent (BOLD) activation to task difficulty in a lifespan sample of 169 healthy humans aged 20–94 years. Greater frontostriatal diffusivity was associated with poorer executive function and this negative association strengthened with increasing age. Whole-brain functional magnetic resonance imaging (fMRI) analyses additionally indicated an association between frontostriatal mean diffusivity and BOLD modulation to difficulty selectively in the striatum across 2 independent fMRI tasks. This association was moderated by age, such that younger- and middle-aged individuals showed reduced dynamic range of difficulty modulation as a function of increasing frontostriatal diffusivity. Together these results demonstrate the importance of age-related degradation of frontostriatal circuitry on executive functioning across the lifespan, and highlight the need to capture brain changes occurring in early-to middle-adulthood.







