Summary: Researchers hypothesize vitamin B1 (thiamine) deficiency may play a significant role in dementia associated with alcohol use disorder. It is known iron deposits in the brain contribute to neurodegenerative diseases. Those with AUD have elevated levels of both iron in their blood and thiamine deficiency. Thiamine is vital for maintaining the blood-brain barrier. Thiamine deficiency associated with AUD disrupts the integrity of the BBB, allowing for more iron deposits within the brain and leading to oxidative tissue damage.
Source: Medical University of Vienna
A common consequence of chronically high alcohol consumption is a decline in cognitive function, which can even progress to full-blown dementia. However, we do not yet fully understand how alcohol damages the brain. A research group led by Stephan Listabarth from MedUni Vienna’s Department of Psychiatry and Psychotherapy, Division of Social Psychiatry, has now developed a hypothesis whereby iron deposits in the brain – resulting from alcohol-induced vitamin B1 deficiency – can be regarded as key factors in cognitive decline. The work has now been published in the leading journal “Alzheimer’s and Dementia”.
In Austria, around 5% of the population are alcohol dependent from the age of 15 onwards. This means that approximately 365,000 people are affected by the dangerous health consequences associated with high alcohol consumption. One of these consequences is a decline in cognitive function, especially memory and abstraction. This is then referred to as alcohol-related dementia. However, we do not yet fully understand the exact pathomechanism, that is to say the way in which the brain is damaged by alcohol.
Researchers Stephan Listabarth, Daniel König and Benjamin Vyssoki from the Department of Psychiatry and Psychotherapy, Division of Social Psychiatry at MedUni Vienna and Simon Hametner from MedUni Vienna’s Department of Neurology, Division of Neuropathology and Neurochemistry, have now advanced a plausible hypothesis to explain alcohol-induced brain damage: the cognitive deterioration is caused by iron deposits in the brain but the administration of vitamin B1 could protect the brain from these deposits.
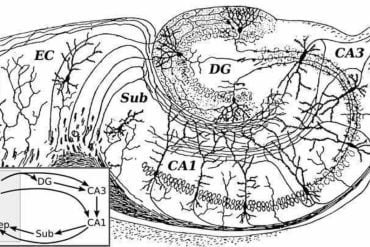
We know from various neurodegenerative diseases that iron deposits in the brain are responsible for nerve tissue damage. These deposits can also be detected in specific regions of the brain (including the basal ganglia) in people who drink a lot of alcohol.
The hypothesis advanced by the study authors now also offers an explanation as to why iron deposits are so prevalent in this patient group: high alcohol consumption results in elevated iron levels in the blood and also to vitamin B1 (thiamine) deficiency, which, among other things, is important for maintaining the blood-brain barrier.

If these two situations coincide, it will deposit more iron inside the brain, ultimately leading to oxidative tissue damage.
This newly described role of vitamin B1 in this process could represent a huge step forward in our understanding of the development of alcohol-related neurological damage and, in particular, could offer a new point of attack for preventive and therapeutic approaches. It would then be conceivable to give continuous vitamin B1 substitutionin future, as a preventive measure.
The researchers believe it would also be useful to evaluate the use of drugs to reduce iron levels (e.g. chelators), as is already done in other neurodegenerative diseases. The authors of the current work have already started planning a prospective clinical study to validate the above-mentioned relationship between alcohol dependency, vitamin B1 deficiency and cerebral iron deposits and to provide a basis for further research in the field of alcohol-related dementia in the future.
About this neuroscience research article
Source:
Medical University of Vienna
Contacts:
Thorsten Medwedeff – Medical University of Vienna
Image Source:
The image is in the public domain.
Original Research: Open access
“Does thiamine protect the brain from iron overload and alcohol-related dementia?” by Stephan Listabarth, Daniel König, Benjamin Vyssoki, Simon Hametner. Alzheimer’s and Dementia.
Abstract
Does thiamine protect the brain from iron overload and alcohol-related dementia?
Alcohol‐related dementia (ARD) is a common and severe co‐morbidity in alcohol use disorder (AUD). We propose brain iron overload (BIO) to be an important and previously neglected pathogenic process, accelerating cognitive decline in AUD. Furthermore, we suggest thiamine, which is frequently depleted in AUD, to be a key modulator in this process: Thiamine deficiency impairs the integrity of the blood‐brain barrier, thereby enabling iron to pass through and accumulate in the brain. This hypothesis is based on findings from animal, translational, and neuroimaging studies, discussed in this article. To validate this hypothesis, translational studies focusing on brain iron homeostasis in AUD, as well as prospective clinical studies investigating prevalence and clinical impact of BIO in AUD, should be conducted. If proven right, this would change the understanding of ARD and may lead to novel therapeutic interventions in prevention and treatment of ARD.