Summary: A new study reports on how Zika directly affects the fetal brain during development and also evades detection by the immune system.
Source: UT Southwestern Medical Center.
The mosquito-borne Zika virus linked to microcephaly and other neurological problems in newborns of affected mothers directly infects the brain progenitor cells destined to become neurons, UT Southwestern Medical Center researchers report in a study published online today in Cell Reports.
The team of researchers used a strain of Zika currently impacting the Americas, and found that the virus infects about 20 percent of cells on average, evades immune system detection, and continues to replicate for weeks.
“The cellular system we studied mirrors what pathologists are finding in the brain tissue of affected infants and will be valuable for further understanding how Zika causes severe brain-related problems. The system may also serve as a platform for testing new therapies targeting the virus,” said Dr. John Schoggins, Assistant Professor of Microbiology at UT Southwestern and senior author of the study.
Zika can be spread by infected mosquitos or through sexual intercourse. In adults, the symptoms are generally mild and include fever, rash, joint pain, and red eyes. However, Zika virus can cause a serious birth defect called microcephaly, and other severe neurological effects such as eye problems, hearing loss, and impaired growth in infants born to women who contracted the virus when pregnant, according to the Centers for Disease Control and Prevention (CDC).
The CDC’s website lists a series of unanswered questions about the virus that the World Health Organization (WHO) has declared a public health emergency of international concern. The unanswered questions include when during pregnancy the infection may harm the fetus and how the virus affects individual pregnancies.
“There was a suggestion that the detrimental effects of the virus might be linked to its ability to infect brain cells, specifically the progenitor cells that give rise to neurons,” said Dr. Schoggins, a Nancy Cain and Jeffrey A. Marcus Scholar in Medical Research, in Honor of Dr. Bill S. Vowell.
“We showed that neural progenitors can be infected by a strain of Zika virus that is currently infecting people in the Americas,” Dr. Schoggins said. “We found that the virus kills some neural progenitor cells, but not all. Other cells survive the infection, and surprisingly, continue to replicate the virus for many weeks. In addition, it appears that Zika virus does not stimulate much of an immune response.”
Dr. Schoggins collaborated on the study with Dr. Genevieve Konopka, Assistant Professor of Neuroscience and a Jon Heighten Scholar in Autism Research, whose expertise includes working with neural progenitor cells, cells similar to stem cells that tend to differentiate into neurons. Other UT Southwestern co-authors included: lead author Dr. Natasha Hanners, a pediatric infectious diseases fellow training in Dr. Schoggins’ lab; Jennifer Eitson, a research assistant in Microbiology; Dr. Noriyoshi Usui, a postdoctoral researcher in Neuroscience; and Microbiology graduate student R. Blake Richardson. A researcher from UCLA also participated.
Funding: This project received support from the National Institutes of Health and the Rita Allen Foundation.
Source: Deborah Wormser – UT Southwestern Medical Center
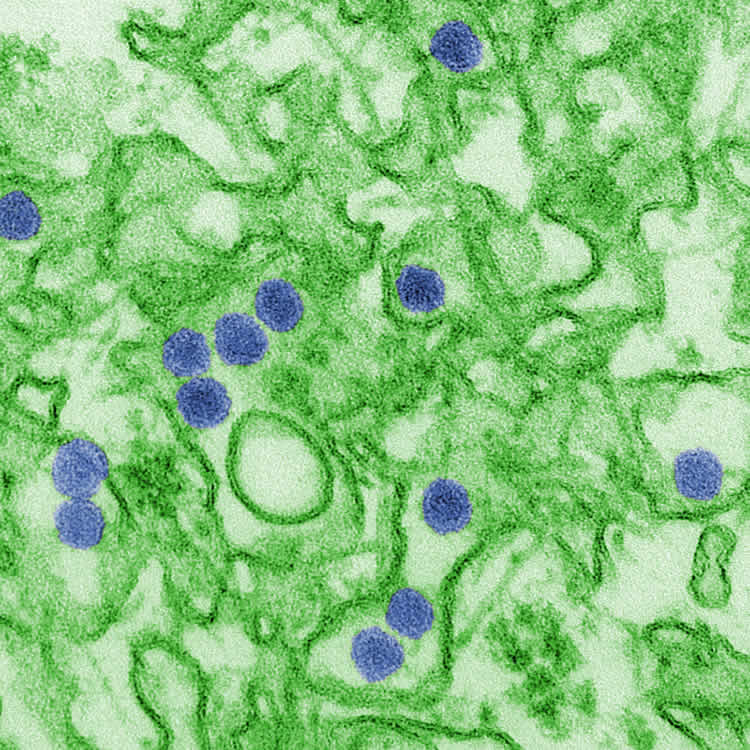
Image Source: This NeuroscienceNews.com image is credited to Wen-Jie Zhao/MDC.
Original Research: Full open access research for “Western Zika Virus in Human Fetal Neural Progenitors Persists Long Term with Partial Cytopathic and Limited Immunogenic Effects” by Natasha W. Hanners, Jennifer L. Eitson, Noriyoshi Usui, R. Blake Richardson, Eric M. Wexler, Genevieve Konopka, and John W. Schoggins in Cell Reports. Published online June 3 3016 doi:10.1016/j.celrep.2016.05.075
[cbtabs][cbtab title=”MLA”]UT Southwestern Medical Center. “Zika Virus Infects Brain Cells and Evades Immune System Detection.” NeuroscienceNews. NeuroscienceNews, 3 June 2016.
<https://neurosciencenews.com/zika-immune-system-4368/>.[/cbtab][cbtab title=”APA”]UT Southwestern Medical Center. (2016, June 3). Zika Virus Infects Brain Cells and Evades Immune System Detection. NeuroscienceNews. Retrieved June 3, 2016 from https://neurosciencenews.com/zika-immune-system-4368/[/cbtab][cbtab title=”Chicago”]UT Southwestern Medical Center. “Zika Virus Infects Brain Cells and Evades Immune System Detection.” https://neurosciencenews.com/zika-immune-system-4368/ (accessed June 3, 2016).[/cbtab][/cbtabs]
Abstract
Western Zika Virus in Human Fetal Neural Progenitors Persists Long Term with Partial Cytopathic and Limited Immunogenic Effects
Highlights
•A 2015 ZIKV isolate replicates in human fetal neural progenitors
•ZIKV in fetal neural progenitors is partially cytopathic and persists for weeks
•ZIKV has limited immunogenic effects in fetal neural progenitors
Summary
The recent Zika virus (ZIKV) outbreak in the Western hemisphere is associated with severe pathology in newborns, including microcephaly and brain damage. The mechanisms underlying these outcomes are under intense investigation. Here, we show that a 2015 ZIKV isolate replicates in multiple cell types, including primary human fetal neural progenitors (hNPs). In immortalized cells, ZIKV is cytopathic and grossly rearranges endoplasmic reticulum membranes similar to other flaviviruses. In hNPs, ZIKV infection has a partial cytopathic phase characterized by cell rounding, pyknosis, and activation of caspase 3. Despite notable cell death, ZIKV did not activate a cytokine response in hNPs. This lack of cell intrinsic immunity to ZIKV is consistent with our observation that virus replication persists in hNPs for at least 28 days. These findings, supported by published fetal neuropathology, establish a proof-of-concept that neural progenitors in the developing human fetus can be direct targets of detrimental ZIKV-induced pathology.
“Western Zika Virus in Human Fetal Neural Progenitors Persists Long Term with Partial Cytopathic and Limited Immunogenic Effects” by Natasha W. Hanners, Jennifer L. Eitson, Noriyoshi Usui, R. Blake Richardson, Eric M. Wexler, Genevieve Konopka, and John W. Schoggins in Cell Reports. Published online June 3 3016 doi:10.1016/j.celrep.2016.05.075






