Summary: A new study reveals the molecular switch that helps control the function of satiety neurons and body weight.
Source: Helmholtz Zentrum München.
Obesity – as research in the past decade has shown – is first and foremost a brain disease. Researchers at Helmholtz Zentrum München, partners in the German Center for Diabetes Research, have now discovered a molecular switch that controls the function of satiety neurons and therefore body weight. The findings were published in the journal Nature Metabolism.
The worldwide epidemic of obesity has reached record levels, and what was once a problem only of industrialized countries is now also affecting the developing world. Consequently, scientists are working with great commitment to identify the mechanisms underlying the disease in order to find new treatments. Researchers at the Institute of Diabetes and Obesity (IDO) of Helmholtz Zentrum München have recently taken a further step in this direction.
Yin and yang of energy metabolism
“Whether we’re hungry or feel full is largely determined in the brain – specifically in the hypothalamus,” explains IDO scientist Dr. Alexandre Fisette, together with Dr. Carmelo Quarta lead co-authors of the aforementioned paper. “Two groups of neurons in the hypothalamus control body weight and energy balance via various molecular messengers. Like yin and yang, they help strike a good balance.” While neurons known as Agrp increase appetite, their counterparts, Pomc neurons, produce a sensation of satiety. However, if the interplay between the two is disturbed, the result can be obesity or type 2 diabetes.
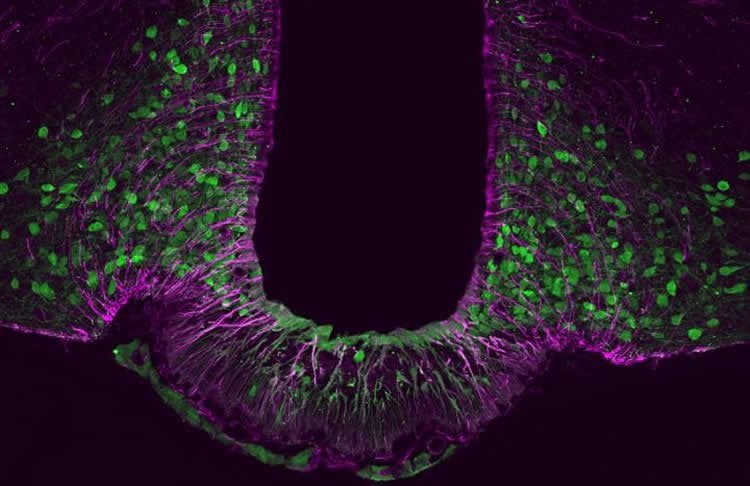
“In our recent study we discovered that a transcription factor* called Tbx3 plays a key role in this mechanism,” says Carmelo Quarta, describing the new findings. “Specifically, in the absence of Tbx3, the neurons responsible for producing a feeling of satiety are no longer able to synthesize the expected molecular messengers.” Applying a broad range of techniques, the scientists were then able to show that Tbx3 plays a pivotal role in maintaining energy and sugar metabolism.
Lack of Tbx3 leads to an identity crisis
“Both in a preclinical model and in fruit flies, the absence of Tbx3 leads to a kind of identity crisis of satiety neurons, resulting in obesity,” says Alexandre Fisette. The same signaling pathways also appear to be present in humans: “In preliminary experiments with human neurons, we were able to show that they are no longer able to carry out their function in the absence of Tbx3,” Carmelo Quarta adds.
“Humans with genetic defects in the Tbx3 gene have long been reported to suffer from obesity,” explains study director Prof. Dr. Dr. h.c. Matthias H. Tschöp, CEO of Helmholtz Zentrum München and holder of the Chair for Metabolic Diseases at the Technical University of Munich.** “Our study explains for the first time the underlying mechanisms and once again focuses attention on the central role of the brain in regulating energy metabolism. We hope that Tbx3 may come into consideration one day as a target for drug therapies.”
Funding: Tikun Olam Ltd funded this study.
Source: Alexandre Fisette – Helmholtz Zentrum München
Publisher: Organized by NeuroscienceNews.com.
Image Source: NeuroscienceNews.com image is credited to Quarta, C. & Fisette, A. et al. (Nature Metabolism).
Original Research: Abstract for “Functional identity of hypothalamic melanocortin neurons depends on Tbx3” by Carmelo Quarta, Alexandre Fisette, Yanjun Xu, Gustav Colldén, Beata Legutko, Yu-Ting Tseng, Alexander Reim, Michael Wierer, Maria Caterina De Rosa, Valentina Klaus, Rick Rausch, Vidhu V. Thaker, Elisabeth Graf, Tim M. Strom, Anne-Laure Poher, Tim Gruber, Ophélia Le Thuc, Alberto Cebrian-Serrano, Dhiraj Kabra, Luigi Bellocchio, Stephen C. Woods, Gert O. Pflugfelder, Rubén Nogueiras, Lori Zeltser, Ilona C. Grunwald Kadow, Anne Moon, Cristina García-Cáceres, Matthias Mann, Mathias Treier, Claudia A. Doege & Matthias H. Tschöp in Nature Metabolism. Published January 17 2019.
doi:10.1038/s42255-018-0028-1
[cbtabs][cbtab title=”MLA”]Helmholtz Zentrum München”Identity Crisis of Satiety Neurons Leads to Obesity.” NeuroscienceNews. NeuroscienceNews, 31 January 2019.
<https://neurosciencenews.com/obesity-neurons-10672/>.[/cbtab][cbtab title=”APA”]Helmholtz Zentrum München(2019, January 31). Identity Crisis of Satiety Neurons Leads to Obesity. NeuroscienceNews. Retrieved January 31, 2019 from https://neurosciencenews.com/obesity-neurons-10672/[/cbtab][cbtab title=”Chicago”]Helmholtz Zentrum München”Identity Crisis of Satiety Neurons Leads to Obesity.” https://neurosciencenews.com/obesity-neurons-10672/ (accessed January 31, 2019).[/cbtab][/cbtabs]
Abstract
Functional identity of hypothalamic melanocortin neurons depends on Tbx3
There has been a dramatic increase in the number of children diagnosed with autism spectrum disorders (ASD) worldwide. Recently anecdotal evidence of possible therapeutic effects of cannabis products has emerged. The aim of this study is to characterize the epidemiology of ASD patients receiving medical cannabis treatment and to describe its safety and efficacy. We analysed the data prospectively collected as part of the treatment program of 188 ASD patients treated with medical cannabis between 2015 and 2017. The treatment in majority of the patients was based on cannabis oil containing 30% CBD and 1.5% THC. Symptoms inventory, patient global assessment and side effects at 6 months were primary outcomes of interest and were assessed by structured questionnaires. After six months of treatment 82.4% of patients (155) were in active treatment and 60.0% (93) have been assessed; 28 patients (30.1%) reported a significant improvement, 50 (53.7%) moderate, 6 (6.4%) slight and 8 (8.6%) had no change in their condition. Twenty-three patients (25.2%) experienced at least one side effect; the most common was restlessness (6.6%). Cannabis in ASD patients appears to be well tolerated, safe and effective option to relieve symptoms associated with ASD.






