Genetic findings support observational evidence that lower vitamin D levels are associated with increased risk of multiple sclerosis, according to a new research article by Brent Richards, from McGill University, Canada, and colleagues published this week in PLOS Medicine.
Multiple sclerosis is a debilitating autoimmune disease that affects the nerves in the brain and spinal cord. There is no known cure for multiple sclerosis and it usually presents between the ages of 20 and 40 years. While some observational evidence suggests there may be a link between lower vitamin D levels and multiple sclerosis risk, it is difficult to infer a causal relationship because individuals who develop multiple sclerosis in these studies might share another unknown characteristic that increases their risk of multiple sclerosis (this is known as confounding).
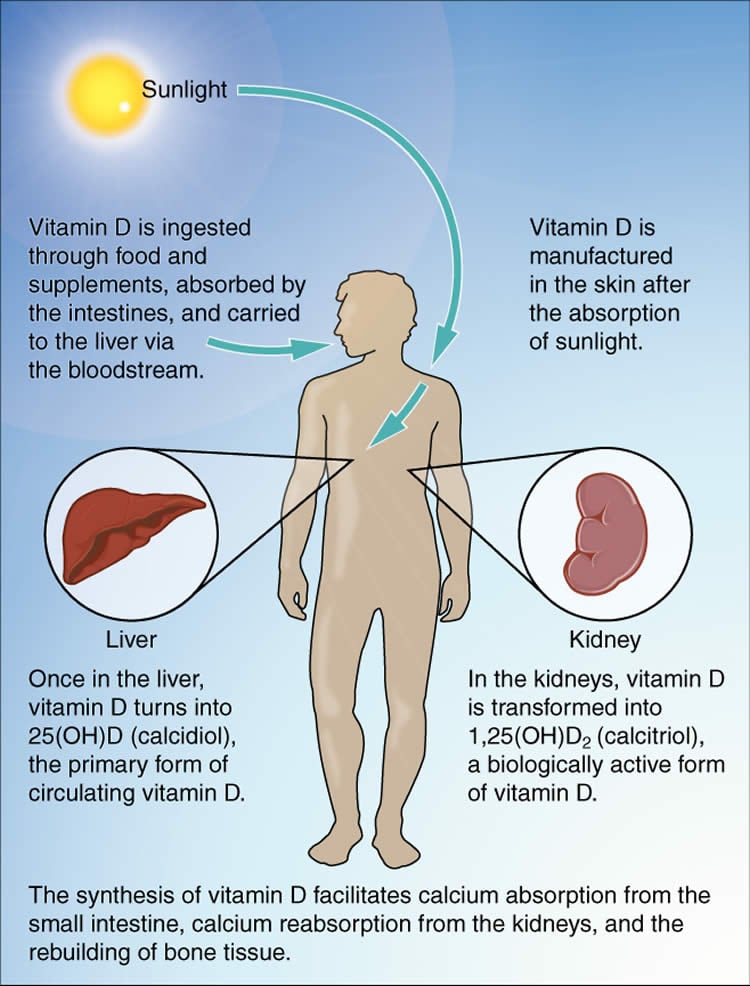
Using a genetic technique called Mendelian randomization to reduce the possibility of confounding the authors examined whether there was an association between genetically reduced vitamin D levels (measured by the level of 25-hydroxyvitamin D, the clinical determinant of vitamin D status) and susceptibility to multiple sclerosis among participants in the International Multiple Sclerosis Genetics Consortium study, which involves 14,498 people with multiple sclerosis and 24,091 healthy controls. The authors found that a genetic decrease in the natural-log-transformed vitamin D level by one standard deviation was associated with a 2-fold increased risk of multiple sclerosis.
While the Mendelian randomization approach used by the authors largely avoids the possibility of confounding or reverse causation, the reliability of these findings may be limited by some of the assumptions made by the researchers during their analysis.
Nevertheless the authors conclude, “genetically lowered vitamin D levels are strongly associated with increased susceptibility to multiple sclerosis. Whether vitamin D sufficiency can delay, or prevent, multiple sclerosis onset merits further investigation in long-term randomized controlled trials.”
The authors also note, “ongoing randomized controlled trials are currently assessing vitamin D supplementation for the treatment and prevention of multiple sclerosis … and may therefore provide needed insights into the role of vitamin D supplementation.”
Funding: JBR is funded by the Canadian Institute of Health Research, (MOP-119462) The Fonds de la Recherche en Santé Québec, the Lady Davis Institute, and the Jewish General Hospital. AL is supported by the Canadian Diabetes Association Postdoctoral Fellowship. The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
Competing Interests: GT has accepted speaker’s fees and consultancy fees from Servier Canada relating to the treatment of hypertension and has participated on an Advisory Board for ISIS Pharmaceuticals for the treatment of dyslipidemia. GT also receives research grants from the Canadian Institute of Health Research and the Heart and Stroke Foundation of Canada. GDS is a member of the Editorial Board of PLOS Medicine. None of these relationships relate to the content/topic of the manuscript under review at PLOS Medicine.
Source: PLOS
Image Source: The image is credited to OpenStax College and is licensed CC BY 3.0
Original Research: Full open access research for “Vitamin D and Risk of Multiple Sclerosis: A Mendelian Randomization Study” by Lauren E. Mokry, Stephanie Ross, Omar S. Ahmad, Vincenzo Forgetta, George Davey Smith, Aaron Leong, Celia M. T. Greenwood, George Thanassoulis, and J. Brent Richards in PLOS Medicine. Published online April 25 2015 doi:10.1371/journal.pmed.1001866
Abstract
Vitamin D and Risk of Multiple Sclerosis: A Mendelian Randomization Study
Background
Observational studies have demonstrated an association between decreased vitamin D level and risk of multiple sclerosis (MS); however, it remains unclear whether this relationship is causal. We undertook a Mendelian randomization (MR) study to evaluate whether genetically lowered vitamin D level influences the risk of MS.
Methods and Findings
We identified single nucleotide polymorphisms (SNPs) associated with 25-hydroxyvitamin D (25OHD) level from SUNLIGHT, the largest (n = 33,996) genome-wide association study to date for vitamin D. Four SNPs were genome-wide significant for 25OHD level (p-values ranging from 6 × 10−10 to 2 × 10−109), and all four SNPs lay in, or near, genes strongly implicated in separate mechanisms influencing 25OHD. We then ascertained their effect on 25OHD level in 2,347 participants from a population-based cohort, the Canadian Multicentre Osteoporosis Study, and tested the extent to which the 25OHD-decreasing alleles explained variation in 25OHD level. We found that the count of 25OHD-decreasing alleles across these four SNPs was strongly associated with lower 25OHD level (n = 2,347, F-test statistic = 49.7, p = 2.4 × 10−12). Next, we conducted an MR study to describe the effect of genetically lowered 25OHD on the odds of MS in the International Multiple Sclerosis Genetics Consortium study, the largest genetic association study to date for MS (including up to 14,498 cases and 24,091 healthy controls). Alleles were weighted by their relative effect on 25OHD level, and sensitivity analyses were performed to test MR assumptions. MR analyses found that each genetically determined one-standard-deviation decrease in log-transformed 25OHD level conferred a 2.0-fold increase in the odds of MS (95% CI: 1.7–2.5; p = 7.7 × 10−12; I2 = 63%, 95% CI: 0%–88%). This result persisted in sensitivity analyses excluding SNPs possibly influenced by population stratification or pleiotropy (odds ratio [OR] = 1.7, 95% CI: 1.3–2.2; p = 2.3 × 10−5; I2 = 47%, 95% CI: 0%–85%) and including only SNPs involved in 25OHD synthesis or metabolism (ORsynthesis = 2.1, 95% CI: 1.6–2.6, p = 1 × 10−9; ORmetabolism = 1.9, 95% CI: 1.3–2.7, p = 0.002). While these sensitivity analyses decreased the possibility that pleiotropy may have biased the results, residual pleiotropy is difficult to exclude entirely.
Conclusions
A genetically lowered 25OHD level is strongly associated with increased susceptibility to MS. Whether vitamin D sufficiency can delay, or prevent, MS onset merits further investigation in long-term randomized controlled trials.
“Vitamin D and Risk of Multiple Sclerosis: A Mendelian Randomization Study” by Lauren E. Mokry, Stephanie Ross, Omar S. Ahmad, Vincenzo Forgetta, George Davey Smith, Aaron Leong, Celia M. T. Greenwood, George Thanassoulis, and J. Brent Richards in PLOS Medicine. Published online April 25 2015 doi:10.1371/journal.pmed.1001866