Summary: eEF1a1 activated by acetylation prevents remyelination, but if the protein is deactivated by deacetylation, myelin sheaths can be rebuilt. The findings shed light on the process of remyelination and could provide avenues of treatment for multiple sclerosis, and other conditions associated with demyelination.
Source: JGU
A research team led by neurobiologist Professor Claire Jacob has identified an important mechanism that can be used to control the restoration of myelin sheaths following traumatic injury and in degenerative diseases. With the insights gained, the researchers were able to regenerate damaged myelin sheaths in mice by treating them with the active substance theophylline, thereby restoring their nerve cell function. The groundbreaking findings are the result of research carried out at Johannes Gutenberg University Mainz (JGU) and the University of Fribourg in Switzerland.
Neurons are composed of axons, i.e., long fiber-like extensions that transmit signals to other cells. Many of them are surrounded by a myelin sheath, a thick fatty layer that protects them and helps to transfer stimuli rapidly. Without myelin, the functional capacity of neurons – and therefore of the whole nervous system – is limited and neurons can easily degenerate. Multiple sclerosis (MS) is one of the diseases associated with myelin sheath degradation. MS patients suffer successive episodes of demyelination resulting in a progressive loss of function of their nervous system. Remyelination of the axons can prevent this.
The aim is to restore the axons’ protective myelin coating
Intact myelin sheaths are a prerequisite for the healthy functioning of the peripheral and central nervous systems. If the peripheral nervous system (PNS) is damaged, in an accident involving injury to the arms or legs for example, the axons and their myelin sheaths can recover relatively well. “Regeneration of the PNS is quite efficient, although it could be improved,” said Professor Claire Jacob, pointing out that even young people do not experience complete regeneration.
However, the central nervous system (CNS) is completely different in this regard as there is no efficient restoration of the axons and therefore of the myelin sheath after a lesion. This means that CNS injuries usually result in permanent paralysis – as in the case of MS when loss of myelin leads to axon degeneration. MS is the most common neurodegenerative disease of the CNS and is attributable to the degradation of the myelin sheath of neurons. The occurrence of successive lesions can cause permanent loss of function of the CNS if myelin sheath restoration is inefficient. The capacity of the body to remyelinate decreases dramatically with age. “In order to promote the restoration of myelin, we need to understand the process that controls the mechanism,” emphasized Jacob.
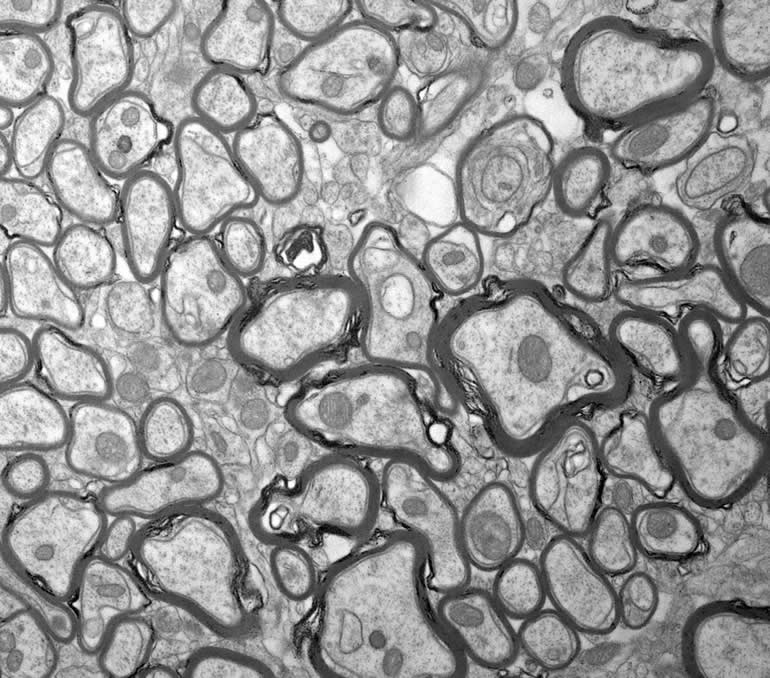
In the recent project, her research group investigated how remyelination occurs in both peripheral and central nervous systems of mice. “First, we wanted to understand the process that blocks remyelination. We subsequently studied how to counteract this blocking effect.” The neuroscientists identified a protein called eEF1A1 as a key factor in the process and found that eEF1A1 activated by acetylation prevents the remyelination process, but if eEF1A1 is deactivated by deacetylation, myelin sheaths can be rebuilt. The protein that deacetylates eEF1A1 is the enzyme called histone deacetylase 2 (HDAC2).
Theophylline promotes myelin reconstruction in both peripheral and central nervous systems
“Once we understood this process, we decided to try to control it by boosting the HDAC2 activity and its synthesis in cells,” said Jacob. This was achieved by using the active substance theophylline, which is also present in tea leaves and has long been used in the treatment of asthma. In a mouse model, the use of theophylline over a period of four days resulted in significant recovery. Restoration of myelin sheaths was particularly impressive in the PNS, where they recovered completely. Regeneration also improved in the CNS, as there was rapid and efficient rebuilding of myelin sheaths in both young and old mice. A low dose of the active substance was sufficient to trigger the improvements – a big plus with regard to the known side effects of theophylline, which occur at higher doses.
“In summary, this study […] shows that theophylline, by activating HDAC2, promotes eEF1A1 deacetylation, increases […] remyelination speed and efficiency after lesion of the PNS and CNS, thus appearing as a very promising compound to test in future translational studies to accelerate and promote remyelination after traumatic lesions or in the context of demyelinating disorders,” write the authors in their paper published in Nature Communications. Currently, funding for corresponding clinical trials in patients is being sought, while a patent application has already been filed.
Professor Claire Jacob has been researching the development of myelin, axon injuries, and their regeneration for 16 years – previously at the University of Fribourg in Switzerland and since October 2018 as head of the Cellular Neurobiology Group at Johannes Gutenberg University Mainz.
About this neurology research article
Source:
American Heart Association
Contacts:
Claire Jacob – JGU
Image Source:
The image is credited to Mert Duman.
Original Research: Open access
“EEF1A1 deacetylation enables transcriptional activation of remyelination” by Mert Duman, Adrien Vaquié, Gianluigi Nocera, Manfred Heller, Michael Stumpe, Devanarayanan Siva Sankar, Jörn Dengjel, Dies Meijer, Teppei Yamaguchi, Patrick Matthias, Thomas Zeis, Nicole Schaeren-Wiemers, Antoinette Hayoz, Sophie Ruff & Claire Jacob. Nature Communications.
Abstract
EEF1A1 deacetylation enables transcriptional activation of remyelination
Remyelination of the peripheral and central nervous systems (PNS and CNS, respectively) is a prerequisite for functional recovery after lesion. However, this process is not always optimal and becomes inefficient in the course of multiple sclerosis. Here we show that, when acetylated, eukaryotic elongation factor 1A1 (eEF1A1) negatively regulates PNS and CNS remyelination. Acetylated eEF1A1 (Ac-eEF1A1) translocates into the nucleus of myelinating cells where it binds to Sox10, a key transcription factor for PNS and CNS myelination and remyelination, to drag Sox10 out of the nucleus. We show that the lysine acetyltransferase Tip60 acetylates eEF1A1, whereas the histone deacetylase HDAC2 deacetylates eEF1A1. Promoting eEF1A1 deacetylation maintains the activation of Sox10 target genes and increases PNS and CNS remyelination efficiency. Taken together, these data identify a major mechanism of Sox10 regulation, which appears promising for future translational studies on PNS and CNS remyelination.






