Although Lewy Body disease (LBD) is the second-most-common degenerative disease after Alzheimer’s disease, it’s not exactly a household name. It affects more than 1.3 million Americans, is poorly recognized, and diagnosis is often significantly delayed. Patients with LBD simultaneously experience losses in cognitive function, mobility and behavior. The late Robin Williams had this form of dementia as did legendary NHL coach Alger Joseph “Radar” Arbour, which also can cause visual hallucinations and make depression worse. Until now, there has been no way to assess or operationalize many of the cognitive and behavioral symptoms of LBD in clinical practice.
A leading neuroscientist at Florida Atlantic University has developed the “Lewy Body Composite Risk Score” (LBCRS) to quickly and effectively diagnose LBD and Parkinson’s disease dementia (PDD) in about three minutes. The LBCRS is a brief rating scale that can be completed by a clinician to assess clinical signs and symptoms highly associated with the pathology of this disease. With this important tool, a clinician can assess whether the patient has bradykinesia, rigidity, postural instability, or rest tremor without having to grade each extremity. This simple, one-page survey provides structured yes/no questions for six non-motor features that are present in patients with LBD, but are much less commonly found in other forms of dementia.
The LBCRS study, “Improving the Clinical Detection of Lewy Body Dementia with the Lewy Body Composite Risk Score,” recently published in Alzheimer’s & Dementia, the journal of the Alzheimer’s Association, involved 256 patients who were compared with the clinical dementia rating and gold standard measures of cognition, motor symptoms, function and behavior. The test was administered in a “real-world” clinic setting with patients who were referred from the community rather than in a research sample. The clinic sample had a mixture of gender, education, comorbidities, behavioral, affective, motor symptoms, and diagnoses. The LBCRS was able to discriminate between Alzheimer’s disease and LBD with 96.8 percent accuracy, and provided sensitivity of 90 percent and specificity of 87 percent.
For the study, caregivers completed evaluations to determine the presence and severity of non-cognitive symptoms observed in the patient and their impact on the caregiver. Each patient was administered a 30-minute test battery at the time of the office visit to assess their cognitive status. The LBCRS was completed after all other rating scales were scored and the diagnosis was presented to the patient and family.
“Most patients never receive an evaluation by a neurologist skilled in the diagnosis of Lewy body dementia, and significant delays and misdiagnoses occur in most patients with this disease,” said James E. Galvin, M.D., M.P.H., one of the most prominent neuroscientists in the country who developed the LBCRS, and a professor of clinical biomedical science in FAU’s Charles E. Schmidt College of Medicine and a professor in FAU’s Christine E. Lynn College of Nursing. “This new tool has the potential to provide a clearer, more accurate picture for those patients who are unable to be seen by specialists, hastening the correct diagnosis and reducing the strain and burden placed on patients and caregivers.”
Another important aspect of the LBCRS is its ability to improve the sensitivity of diagnosis, thereby reducing the risk of exposure to patients with LBD to medications that can have potentially serious adverse consequences. The survey also increases the potential opportunity to receive appropriate symptomatic therapies in a timely fashion, and lessens the inappropriate exclusion from and inclusion into clinical trials.
“Early detection of Lewy body dementias will be important to enable future interventions at the earliest stages when they are likely to be most effective,” said Galvin. “Our study provides evidence-based methodology that will have applications in clinical practice, participation in clinical trials, prevention studies, community surveys, and biomarkers research.”
Galvin is one of the leading international experts on LBD, and has been working to improve clinical detections by combining biomarkers including high density EEG, functional and structural MRI, PET scans and CSF biomarkers to characterize and differentiate LBD from healthy aging and other neurodegenerative diseases.
Galvin has led efforts to develop a number of dementia screening tools, including the Quick Dementia Rating System (QDRS), AD8, a brief informant interview to translate research findings to community settings. He has done cross-cultural validation of dementia screening methods in comparison with Gold Standard clinical evaluations and biomarker assays. His team also has developed sophisticated statistical models to explore transition points in clinical, cognitive, functional, behavioral and biological markers of disease in healthy aging, mild cognitive impairment, Alzheimer disease, and Parkinson’s disease.
Source: Gisele Galoustian – Florida Atlantic University
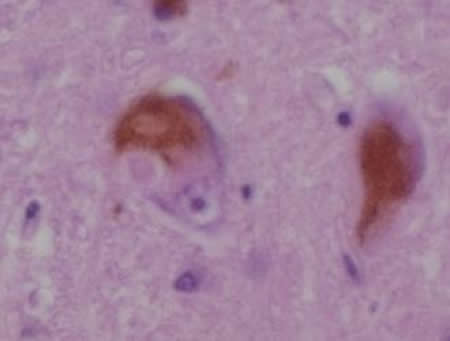
Image Source: The image is credited to Dr. Andreas Becker and is licensed CC BY-SA 3.0
Original Research: Full open access research for “Improving the clinical detection of Lewy body dementia with the Lewy body composite risk score” by James E. Galvin in Alzheimer’s & Dementia: Diagnosis, Assessment & Disease Monitoring. Published online July 2 2015 doi:10.1016/j.dadm.2015.05.004
Abstract
Improving the clinical detection of Lewy body dementia with the Lewy body composite risk score
Introduction
Dementia with Lewy bodies (DLB) is a challenge to diagnose, particularly outside of expert centers with long delays in diagnosis leading to significant burden to patients and caregivers. Although consensus criteria have excellent specificity, there is no standardized way to assess symptoms reducing sensitivity. We developed the Lewy body composite risk score (LBCRS) from autopsy-verified cases to improve the ability to detect DLB in clinic and research populations.
Methods
The LBCRS was tested in a consecutive series of 256 patients compared with the clinical dementia rating and gold standard measures of cognition, motor symptoms, function, and behavior. Psychometric properties including floor and ceiling effects; concurrent, construct, and known-groups validity; and internal consistency of the LBCRS were determined. Receiver operator characteristic (ROC) curves assessed the ability of LBCRS to differentiate (1) DLB from Alzheimer’s disease (AD), (b) DLB from all dementia, and (c) mild cognitive impairment (MCI) due to DLB from MCI due to AD. The LBCRS was completed independent of the clinical evaluation.
Results
Mean LBCRS scores were significantly different between DLB and AD (6.1 ± 2.0 vs. 2.4 ± 1.3, P < .001) and between MCI-DLB versus MCI-AD (3.2 ± 0.9 vs. 1.0 ± 0.8, P < .001). The LBCRS was able to discriminate DLB from other causes of dementia. Using a cutoff score of 3, areas under ROC for DLB versus AD = 0.93 (0.89–0.98) and for MCI-DLB versus MCI-AD = 0.96 (0.91–1.0).
Discussion
The LBCRS increases diagnostic probability that Lewy body pathology is contributing to the dementia syndrome and should improve clinical detection and enrollment for clinical trials.
“Improving the clinical detection of Lewy body dementia with the Lewy body composite risk score” by James E. Galvin in Alzheimer’s & Dementia: Diagnosis, Assessment & Disease Monitoring. Published online July 2 2015 doi:10.1016/j.dadm.2015.05.004






