Summary: According to researchers, women who are obese and those suffering from anorexia respond differently to taste than those without an eating disorder.
Source: University of Colorado Anschutz Medical Campus.
Flavors either too intense or hard to distinguish.
Researchers at the University of Colorado Anschutz Medical Campus have discovered that women suffering from anorexia nervosa and those who are obese respond differently to taste, a finding that could lead to new treatments for the eating disorders.
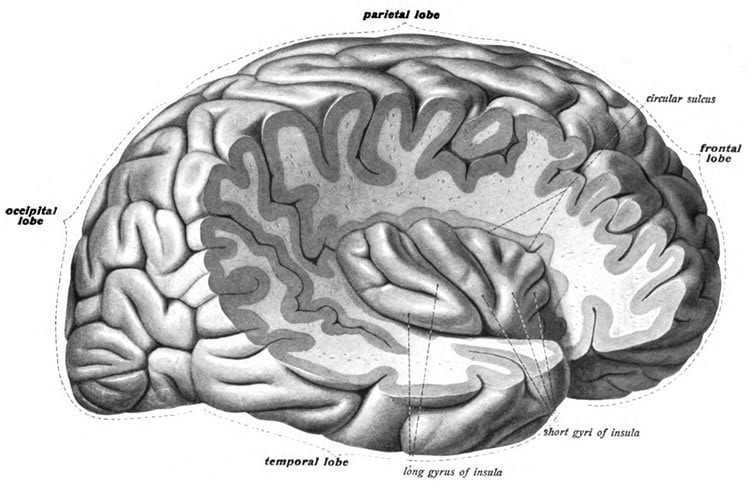
“Taste is an important driver of food intake and invariably associated with distinct neuronal patters in the insula, the brain’s primary taste cortex,” said the study’s lead author Guido Frank, MD, a psychiatrist and associate professor at the CU School of Medicine.
The study was recently published online in the International Journal of Eating Disorders.
Frank and his team set out to find if abnormal eating patterns were associated with changes in the insula’s ability to classify taste stimuli.
Some 106 women of similar age underwent brain imaging while tasting sugar water or a tasteless water solution. Researchers studied how well the insula could differentiate between the flavors.
Individuals with anorexia nervosa or those who were obese, had difficulty distinguishing between ordinary water and sugar water, compared to control subjects and those who had recovered from anorexia nervosa.
“If you can’t differentiate between tastes, that could impact how much you eat,” Frank said. “That could also activate or not activate brain reward circuits.”
These changes, he said, could occur on a variety of levels. For example, leptin and other hormones are altered in obesity and eating disorders, affecting how the brain responds to food. At the same time, the reduced ability of the insula to classify taste could be due to structural changes within this brain region or alternatively could result in altered taste signal processing in different pathways to the insula.
Research indicates that these problems diminish once a person reaches a healthy weight.
While more research is needed, Frank said one possible treatment could be to alter the taste of food.
“Perhaps adjusting flavor intensity by reducing it for those with anorexia and enhancing it for those who are obese,” he said. “It’s something we need to examine more closely.”
Funding: Funding information is not available.
Source: David Kelly – University of Colorado Anschutz Medical Campus
Image Source: This NeuroscienceNews.com image is in the public domain.
Original Research: Abstract for “Extremes of eating are associated with reduced neural taste discrimination” by Guido K.W. Frank, Megan E. Shott, Carrie Keffler and Marc-Andre Cornier in International Journal of Eating Disorders. Published online April 16 2016 doi:10.1002/eat.22538
[cbtabs][cbtab title=”MLA”]University of Colorado Anschutz Medical Campus. “How Obese and Anorexic People React Differently to Taste.” NeuroscienceNews. NeuroscienceNews, 16 May 2016.
<https://neurosciencenews.com/eating-disorders-taste-insula-4245/>.[/cbtab][cbtab title=”APA”]University of Colorado Anschutz Medical Campus. (2016, May 16). How Obese and Anorexic People React Differently to Taste. NeuroscienceNews. Retrieved May 16, 2016 from https://neurosciencenews.com/eating-disorders-taste-insula-4245/[/cbtab][cbtab title=”Chicago”]University of Colorado Anschutz Medical Campus. “How Obese and Anorexic People React Differently to Taste.” NeuroscienceNews.
https://neurosciencenews.com/eating-disorders-taste-insula-4245/ (accessed May 16, 2016).[/cbtab][/cbtabs]
Abstract
Extremes of eating are associated with reduced neural taste discrimination
Objective
Eating disorders are severe psychiatric disorders of unknown etiology. Understanding how neuronal function affects food choices could help personalize treatment based on brain function. Here we wanted to determine whether disordered eating behavior is associated with alterations in the primary taste cortex’s ability to classify taste stimuli, which could interfere with taste reward processing.
Method
One-hundred and six women, 27 healthy comparison (age 26.15 ± 6.95 years), 21 with restricting-type anorexia nervosa (AN; age 23.10 ± 6.14 years), 19 recovered from restricting-type AN (recovered AN; age 26.95 ± 5.31 years), 20 with bulimia nervosa (BN; age 25.15 ± 5.31 years), and 19 with obesity (age 28.16 ± 8.13 years), received sucrose, control solution or no taste stimulation during functional magnetic resonance brain imaging. Multivariate Bayesian pattern analysis (decoding) and cross-validation tested taste classification accuracy (adjusted for comorbidity, medication use, taste perception, interoception, and brain activation volume).
Results
For sucrose versus control solution, classification accuracy differed (F = 2.53, p < 0.041). Post hoc tests indicated higher classification accuracy in healthy comparison compared to women with AN (p < 0.016) or obesity (p < 0.027), and in recovered AN as compared to AN (p < 0.016) or obesity (p < 0.047) groups. Taste stimulation resulted in sparse insula voxel activation across all groups.
Discussion
Reduced classification accuracy across stimuli in women with AN or obesity could indicate low brain encoding discrimination of stimulus quality, which could contribute to altered reward activation and eating drive that is not adjusted to nutritional needs. This deficit appears to normalize with recovery from AN, but adjusting food flavor intensity could aid in the treatment of individuals with AN or obesity.
“Extremes of eating are associated with reduced neural taste discrimination” by Guido K.W. Frank, Megan E. Shott, Carrie Keffler and Marc-Andre Cornier in International Journal of Eating Disorders. Published online April 16 2016 doi:10.1002/eat.22538